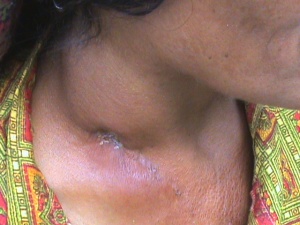
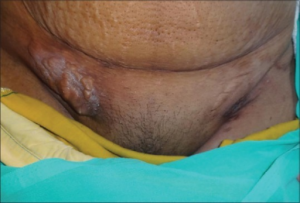
Tuberculous lymphadenitis
(Redirected from Scrofula)
Background
- Also known as "scrofula" when involves cervical lymph nodes
- Most common form of extrapulmonary TB
- TB causes up to 43% of peripheral lymphadenopathy in the developing world [1]
- In the US, more common among Asian Pacific Islanders and in females
- Most cases occur in the setting of reactivation of latent infection
Clinical Features
- Enlarging, painless, red, firm, mass, most commonly in the anterior or posterior cervical chain
- Can be complicated by ulceration, fistula, or abscess formation
- Systemic signs and symptoms are uncommon, except patients with HIV (in whom lymphadenitis is usually generalized)
Differential Diagnosis
Lymphadenitis
Infectious
- Reactive adenitis
- Bacterial lymphadenitis
- Tuberculous lymphadenitis
- Cellulitis
- Cat-scratch disease
- Parotitis
- Lymphangitis
- Toxoplasmosis
- Tularemia
- Viral disease
- Fungal disease
- Reactive adenitis
Non-Infectious
- Malignancy
- Lymphoma
- Metastatic cancer
- Rheumatologic Disease
- Kawasaki Disease
- Systemic lupus erythematosus
- Sarcoidosis
- Juvenile Idiopathic Arthritis
- Langerhans Cell Histiocytosis
- Cutaneous Lesions:
- Bacillary angiomatosis
- Purpura
- Hematomas
- Angiomas
- Dermatofibromas
- Nevi
- Drug reaction
- Postvaccination
- Sarcoidosis
- Salivary gland diagnoses
Neck mass
Acute
- Reactive lymphadenopathy- most common
- Viral URI
- EBV
- CMV
- Strep/staph
- HIV
- Toxoplasmosis
- Bartonella henselae- kitten or flea exposure
- Tuberculous lymphadenitis (scrofula)
- Descending infections from oral cavity
- Sialoadenitis (can also be chronic)
- Trauma-related
- Hematoma
- Pseudoaneurysm or AV fistula
Subacute (weeks to months)
- Cancer
- Systemic diseases
Chronic
- Thyroid nodules or cancer
- Goiters
- Graves' disease
- Hashimoto thyroiditis
- Iodine deficiency
- Lithium use
- Toxic multinodular
- Congenital cysts
- Branchial cleft cyst
- Thyroglossal duct cyst- 2nd most common benign neck mass
- Dermoid cyst
- Carotid body tumor
- Glomus jugulare or vagale tumor
- Laryngocele
- Lipoma/liposarcoma
- Parathyroid cysts or cancer
Evaluation
- Fine needle aspiration: sensitivity and specificity (77 and 93% respectively)[2]
- Excisional biopsy (if FNA is not diagnostic)
- highest diagnostic yield
- Submit specimens for histology, culture, and Nucleic acid amplification testing
- caseating granulomas on histopathology is highly suggestive of TB
- CT can be useful to identify involved lymph nodes for biopsy
- CXR: most do not have evidence of active pulmonary TB in nonendemic countries
- Sputum smear and culture: positive only in approximately 20% of cases[3]
Management
- Medical therapy
- Rifampicin, isoniazid, ethambutol, and pyrazinamide (RIPE therapy) given daily x 2 months
- Followed by rifampicin and isoniazid (given either daily or three times weekly) x 4 months
- Surgical excision may be performed if medical therapy fails
- Do not I&D, can result in permanent sinuses and prolonged drainage
Disposition
See Also
External Links
References
- ↑ Dandapat MC, Mishra BM, Dash SP, Kar PK. Peripheral lymph node tuberculosis: a review of 80 cases. Br J Surg. 1990;77(8):911-2.
- ↑ Lau SK. Efficacy of fine needle aspiration cytology in the diagnosis of tuberculous cervical lymphadenopathy. J Laryngol Otol. 1990;104(1):24-7.
- ↑ Polesky A. Peripheral tuberculous lymphadenitis: epidemiology, diagnosis, treatment, and outcome. Medicine (Baltimore). 2005;84(6):350-62.