Branchial cleft anomaly
(Redirected from Branchial cleft)
Background
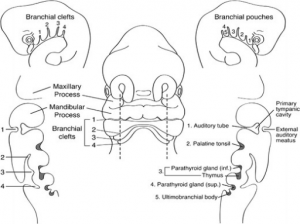
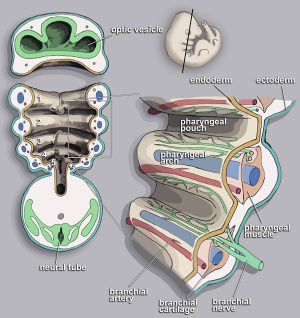
Frontal schematic representation of a 5-mm human embryo at the fifth week of gestation. Sagittal sections taken through the branchial apparatus demonstrate the anatomic relationship of external clefts and internal pouches as well as the derivation of important head and neck structures. The sixth arch is very small and not visualised as a separate, discrete structure from pouch 4/5.
- During 4th week of embryonic development, five branchial arches grow into distinct parts of head and neck
- All consist of arteries, nerves, muscle, skeletal tissue
- If arches fail to fuse--> soft tissue anomaly on lateral neck may form, called branchial cleft anomaly
- Anomalies include cysts (most common), fistulas, sinus tracts
- 2nd branchial cleft anomalies most common
Clinical Features
- Lateral neck soft tissue anatomy
- Typically asymptomatic unless superinfected causing cellulitis or abscess formation
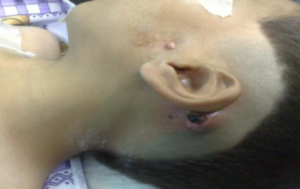
- First branchial cleft cyst
- Lump in parotid/auricular region
- Facial nerve palsy
- May drain through neck and external auditory canal
- Second branchial cleft cyst
- Most common
- Present in late childhood or early adulthood
- Swelling below angle of mandible and anterior to sternocleidomastoid
- Sinus tracts travel into the deep neck structures and drain into tonsillar fossa
- Fistulae cause mucus drainage from cutaneous opening at lateral neck
- Very rarely become squamous cell carcinoma
- Third and fourth branchial cleft cyst
- Difficult to differentiate between the two
- Located lower in neck, anterior or posterior to sternocleidomastoid
- Preference for left side
Differential Diagnosis
Acute
- Reactive lymphadenopathy- most common
- Viral URI
- EBV
- CMV
- Strep/staph
- HIV
- Toxoplasmosis
- Bartonella henselae- kitten or flea exposure
- Tuberculous lymphadenitis (scrofula)
- Descending infections from oral cavity
- Sialoadenitis (can also be chronic)
- Trauma-related
- Hematoma
- Pseudoaneurysm or AV fistula
Subacute (weeks to months)
- Cancer
- HPV-related squamous cell carcinoma
- Upper aerodigestive tract squamous cell carcinoma
- Metastatic disease
- Lymphoma
- Parotid tumors
- Systemic diseases
Chronic
- Thyroid nodules or cancer
- Goiters
- Graves' disease
- Hashimoto thyroiditis
- Iodine deficiency
- Lithium use
- Toxic multinodular
- Congenital cysts
- Thyroglossal duct cyst- 2nd most common benign neck mass
- Dermoid cyst
- Carotid body tumor
- Glomus jugulare or vagale tumor
- Laryngocele
- Lipoma/liposarcoma
- Parathyroid cysts or cancer
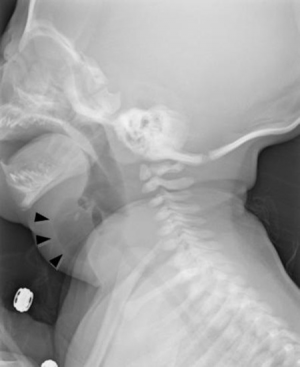
Evaluation
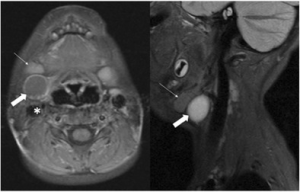
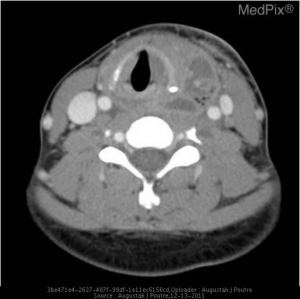
MRI of wwo-year-old child with a rounded and well-defined T1 isointense, T2 hyperintense lesion with thin peripheral enhancement (thick white arrows). It is located posterior to the right submandibular gland (thin white arrow) and anterior to the sternocleidomastoid muscle and carotid sheath (asterisk). This was confirmed to represent a second branchial cleft cyst following surgical excision.
Workup
- Consider one of the following:
Diagnosis
- Typically via imaging (see workup for options)
Management
- Surgical excision is definitive treatment (high risk of recurrence if not completely excised)
- Antibiotics if superinfection present
Disposition
- Discharge with outpatient surgical referral (if no systemic signs of infection present)
- Admit for sepsis