Hyperthyroidism
Background
- Hyperthyroidism: Excess circulating hormone resulting from thyroid gland hyperfunction
- Thyrotoxicosis: Excess circulating thyroid hormone originating from any cause
Causes
Primary Hyperthyroidism
- Graves disease (toxic diffuse goitre)
- Toxic multinodular goitre
- 2nd most common cause
- Multiple autonomously functioning nodules [3]
- Milder, more gradual disease than Graves' hyperthyroidism
- Toxic nodular (adenoma) goitre
- Single hyperfunctioning nodule
- Similar presentation to multinodular goitre, but less common [4]
Secondary Hyperthyroidism
- Thyrotropin-secreting pituitary adenoma
- Thyroiditis
- Hashimoto thyroiditis
- Autoimmune disorder
- Thyroid antibodies and lymphocytic infiltration [5]
- Painless goitre
- Initially gland is overactive (hyperthyroidism state) followed by hypothyroidism
- Subacute painful thyroiditis (de Quervain thyroiditis)[6]
- May be caused by viral infection
- Viral prodrome followed by anterior neck pain
- Tender thyroid (palpation, head movement, swallowing)
- 50% have symptoms of hyperthyroid lasting 3 - 6 weeks
- 1/3 have hypothyroidism for up to 6 months
- Subacute painless thyroiditis [7]
- Small, non-tender goitre
- Mild symptoms
- Autoimmune
- Postpartum thyroiditis [8]
- 3 phases:
- Thyrotoxic phase 2 -6 months postpartum (20-30% have only this phase)
- Hypothyroid phase lasting 2 -3 months (but may be permanent) (40% have this phase only)
- Euthyroid phase within first postpartum year
- Some women develop permanent hypothyroidism
- 70% recurrence in subsequent pregnancies
- 3 phases:
- Suppurative thyroiditis [9]
- Rare
- Life-threatening
- Infection usually bacterial, but can be parasitic, mycobacterial, or fungal
- Usually have pre-existing thyroid disorder and immune compromise
- Radiation thyroiditis
- Hashimoto thyroiditis
Other causes:
- Apathetic thyrotoxicosis (elderly, masking comorbidities)
- Metastatic thyroid cancer
- Iodine-induced thyrotoxicosis
- Amiodarone-induced thyroiditis [10]
- Possible mechanisms:
- Drug-induced destructive thyroiditis
- Hyperthyroidism caused by iodine load (amiodarone contains a large amount of iodine)
- Drug-induced thyroiditis may also occur with interleukin-2, Interferon-α, lithium, tyrosine kinase inhibitors, HAART
- Possible mechanisms:
- Molar pregnancy
Spectrum of Thyroid Disease
- Myxedema coma << hypothyroidism < euthyroid > hyperthyroidism >> thyroid storm
Clinical Features
Constitutional signs:
Neuropsychiatric:
- Emotional lability
- Fine tremor
- Anxiety
- Muscle wasting
- Confusion
- Hyperreflexia
- Coma
- Periodic paralysis
- Psychosis
Ophthalmologic:
- Diplopia
- Lid lag
- Eye irritation
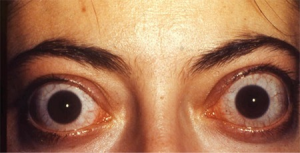
- Exophthalmos
- Ophthalmoplegia
Endocrine:
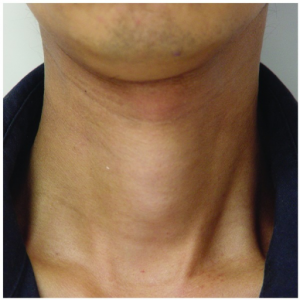
- Neck fullness/tenderness (thyroid gland)
Cardiorespiratory:
- Dyspnea
- Widened pulse pressure
- Palpitations
- Systolic hypertension
- Chest pain
- Sinus tachycardia
- Atrial fibrillation
- Occurs in 10-20% of patients and can revert to sinus rhythm when hyperthyroidism treated
- Atrial flutter
- CHF
GI:
- Diarrhea
- Hyperactive bowel sounds
Reproductive:
- Oligomenorrhea
- Gynecomastia
- Telangiectasia
Gynecologic:
- Menorrhagia
- Sparse pubic hair
Hematologic:
Dermatologic:
- Hair loss
- Pretibial myxedema
- Warm, moist skin
- Palmar erythema
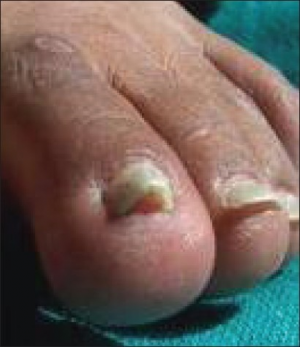
- Onycholysis
Apathetic hyperthyroidism: (elderly patients)[11]
- Placid apathetic facies
- Depression
- Lethargy
- Muscular weakness and wasting
- Excessive weight loss
- Cardiac dysrhythmias
- Absent or small goiter
- Absence of ocular symptoms
- Agitation and confusion
Differential Diagnosis
Tachycardia
- Anemia
- Dehydration
- Fever
- Infection, Sepsis
- Anion gap acidosis
- Hyperthyroid
- Arrhythmia
- PE
- CHF
- MI
- Tamponade
- Myocardial contusion
- Cardiac valvular disease
- Hyper/hypoglycemia
- Drug intoxication
- Drug withdrawal
- Toxicity
- Pain
- Psych (anger, fear)
Palpitations
- Arrhythmias:
- Non-arrhythmic cardiac causes:
- Psychiatric causes:
- Drugs and Medications:
- Alcohol
- Caffeine
- Drugs of abuse (e.g. cocaine)
- Medications (e.g. digoxin, theophylline)
- Tobacco
- Misc
Evaluation
Workup
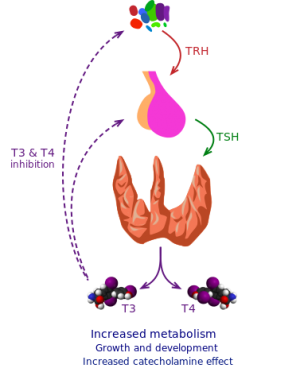
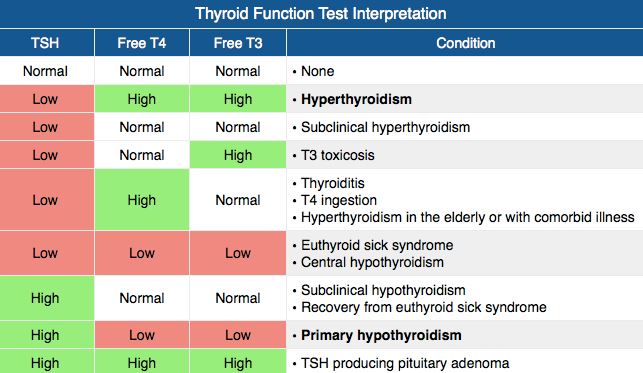
- TSH (↓)
- Free T4 (↑)
- Free T3 (↑)
Diagnosis
Management
- If asymptomatic or mild symptoms, no treatment required in ED
- If symptomatic, consider Thyroid storm
Disposition
- If asymptomatic or no thyroid storm, discharge with outpatient follow-up.
- Admit for significant symptoms or thyroid storm.
See Also
References
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Thiessen, M. (2018). Thyroid and Adrenal Disorders. Rosen's emergency medicine: Concepts and clinical practice (9th ed.). Philadelphia, PA: Elsevier/Saunders
- ↑ Rehman SU et al. Thyroid Disorders in Elderly Patients. South Med J. 2005;98(5):543-549.