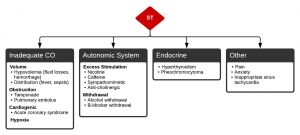
Sinus tachycardia
Background
- Sinus rhythm at a rate above the upper limit of normal
- In adults, usually >100 bpm
- In pediatric patients it varies by age until age 8 or 9 (see pediatric vital signs)
- Usually seen as a secondary response to a primary medical condition
Causes of sinus tachycardia
- Emotional or psychiatric causes
- Pain, anger, or anxiety
- Response to fever (about 10 bpm per degree C > 37.0)
- SIRS (from infection or other causes)
- Dehydration/hypovolemia
- Anemia
- Drug/alcohol intoxication (particularly sympathomimetic or anticholinergic drugs, but may also be seen in aspirin, theophylline, or other ingestions)
- Drug/alcohol withdrawal
- Anion gap acidosis
- Hyperthyroidism
- PE
- CHF
- Cardiac tamponade
- Myocardial contusion
- Cardiac valvular disease
- Hyper or hypoglycemia
- Myocardial infarction
- Pheochromocytoma
Clinical Features
- Tachycardia
- +/- Palpitations
Differential Diagnosis
Narrow-complex tachycardia
- Regular
- AV Node Independent
- Sinus tachycardia
- Atrial tachycardia (uni-focal or multi-focal)
- Atrial fibrillation
- Atrial flutter
- Idiopathic fascicular left ventricular tachycardia
- AV Node Dependent
- AV Node Independent
- Irregular
- Multifocal atrial tachycardia (MAT)
- Sinus tachycardia with frequent PACs, PJCs, PVCs
- Atrial fibrillation
- Atrial flutter with variable conduction
- Digoxin Toxicity
Wide-complex tachycardia
Assume any wide-complex tachycardia is ventricular tachycardia until proven otherwise (it is safer to incorrectly assume a ventricular dysrhythmia than supraventricular tachycardia with abberancy)
- Regular
- Monomorphic ventricular tachycardia
- PSVT with aberrant conduction:
- PSVT with bundle branch block^
- PSVT with accessory pathway
- Atrial flutter with bundle branch block^
- Sinus tachycardia with bundle branch block^
- Accelerated idioventricular rhythm (consider if less than or ~120 bpm)
- Metabolic
- Irregular
- Atrial fibrillation/atrial flutter with variable AV conduction AND bundle branch block^
- Atrial fibrillation/atrial flutter with variable AV conduction AND accessory pathway (e.g. WPW)
- Atrial fibrillation + hyperkalemia
- Polymorphic ventricular tachycardia
^Fixed or rate-related
Palpitations
- Arrhythmias:
- Non-arrhythmic cardiac causes:
- Psychiatric causes:
- Drugs and Medications:
- Alcohol
- Caffeine
- Drugs of abuse (e.g. cocaine)
- Medications (e.g. digoxin, theophylline)
- Tobacco
- Misc
Evaluation
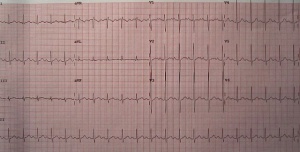
Sinus tachycardia on 12-lead ECG
Workup
- ECG
- History and physical exam
- Look for intoxication/withdrawal, infection, dehydration, bleeding, or a psychiatric/emotional state
- Consider orthostatic vital signs
- If history and physical are unable to explain the tachycardia, limited labs and imaging studies may be indicated:
- CBC
- BMP
- Utox
- Urine pregnancy
- Consider:
- Empiric treatment for anxiety or pain (e.g. benzodiazepine or NSAID)
- Urinalysis
- TSH
- Troponin
- CXR
- Consider workup for PE (e.g. D-dimer or CTA)
Diagnosis
- Based on ECG
- Look for regular rate and presence of p-waves to support diagnosis of sinus tachycardia
Management
- Tailored to specific cause of sinus tachycardia:
- Fluids for dehydration
- Blood for hemorrhage
- Anticoagulation/thrombolytics for PE
- Antibiotics and fluids for sepsis
- Benzodiazepines for alcohol withdrawal
- Supportive care for intoxication
- If no cause identified, treat with caution
- Beta blockers or other antiarrhythmics are not appropriate for unexplained sinus tachycardia as patient may require elevated heart rate to maintain appropriate cardiac output depending on underlying cause
- May consider discharge with strict return precautions if no clear cause identified and no serious pathology suspected after careful work-up
- Ensure close follow-up and strict return precautions
Disposition
- Depends on cause of tachycardia:
- Home for pain, fever, or anxiety resolving with appropriate treatment
- Certain withdrawal or intoxication syndromes may require ED observation or admission
- ICU for severe sepsis
- OR for life-threatening hemorrhage