Ectopic pregnancy
Background
- Leading cause of maternal death in first trimester and overall third leading cause of maternal death
- Occur in 2% of all pregnancies[1] and as high as 6-16% in those presenting to the ED[2]
- Pregnancy in patient with prior tubal ligation or IUD in place is ectopic until proven otherwise (25-50% are ectopic)
- Even if an IUP is visualized, there is a small risk of heterotopic ectopic pregnancy
- General Population = 1 per 4000
- IVF Population = 1 per 100
Risk Factors[3][4]
Risk factors absent in almost half of patients
| Risk Factor | Odds Ratio |
| Previous tubal surgery | 21 |
| Previous ectopic pregnancy | 8.3 |
| Diethylstilbestrol exposure | 5.6 |
| Previous PID | 2.4 to 3.7 |
| Assisted Fertility | 2 to 2.5 |
| Smoker | 2.3 |
| Previous intrauterine device use | 1.6 |
Specific Types by Location
Most common location is the ampulla of the fallopian tube
Cervical Ectopic
- Very rare with delayed diagnoses due to decreased accuracy of US
- As high as 10% with reproductive IVF
Interstitial Ectopic
- Typically presents after 8 wks, with rupture possibly occurring as early as 5 wks
- Implantation in myometrium in proximal part of fallopian tube, commonly misdiagnosed on ultrasound as intrauterine pregnancy
- 65% diagnosis on ultrasound and laparascopy is gold standard
- US characteristics:
- Empty uterus
- Gestational sac separate from endometrium
- Gestational sac > 1 cm from lateral aspect of uterine cavity
- < 5 mm mantle surrounding the sac
Clinical Features
Must consider in all women of childbearing age with abdominal and/or pelvic pain
- Ruptured
- Shock
- Rebound tenderness
- Non-ruptured (early)
Differential Diagnosis
Vaginal Bleeding in Pregnancy (<20wks)
- Ectopic pregnancy
- Subchorionic hematoma
- First Trimester Abortion
- Complete Abortion
- Incomplete Abortion
- Inevitable Abortion
- Missed Abortion
- Septic abortion
- Threatened Abortion
- Gestational trophoblastic disease
- Consider when pregnancy-induced hypertension is seen before 24 wks of gestation
- Heterotopic pregnancy
- Implantation bleeding
- Molar pregnancy
- Non-pregnancy related bleeding
- Cervicitis
- Fibroids
- Implantation bleeding
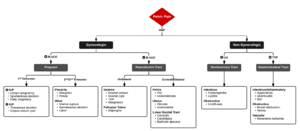
Acute Pelvic Pain
Gynecologic/Obstetric
- Normal variants may be noted on exam but generally do not cause pain or other symptoms
- Nabothian cysts: Epithelial cells within mucous glans that appear as yellow inclusions on the cervix
- Cervical Ectropion: Edothelial cells on the exterior of the cervix
- Parous cervix: The is no longer round but may have multiple shapes after birth
- Pregnancy-related
- Ectopic pregnancy
- Spontaneous abortion, threatened or incomplete
- Septic abortion
- Pelvic organ prolapse
- Acute Infections
- Vulvovaginitis
- Adnexal Disorders
- Hemorrhage/rupture of ovarian cyst
- Ovarian torsion
- Twisted paraovarian cyst
- Other
- Myoma (degenerating)
- Genitourinary trauma
- Ovarian hyperstimulation syndrome
- Sexual assault
- Recurrent
- Mittelschmerz
- Primary/Secondary Dysmenorrhea
- Pelvic Congestion Syndrome
- Endometriosis
Genitourinary
Gastrointestinal
- Gastroenteritis
- Appendicitis
- Bowel obstruction
- Perirectal abscess
- Diverticulitis
- Inflammatory bowel disease
- Irritable bowel syndrome
- Mesenteric adenitis
Musculoskeletal
- Abdominal wall hematoma
- Psoas hematoma, psoas abscess
- Hernia
Vascular
- Pelvic thrombophlebitis
- Abdominal aortic aneurysm
- Ischemic bowel (Mesenteric Ischemia)
Evaluation
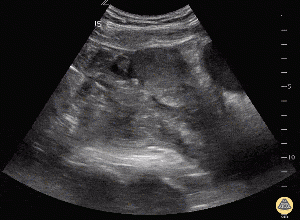
Ultrasound shows ectopic pregnancy[6]
Work-Up
- hemoglobin (or CBC)[7]
- Beta-HCG (quantitative)
- Type and Screen with Rh Factor
- FAST and Pelvic US
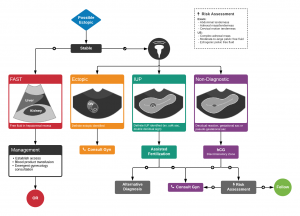
Diagnostic Algorithm
Using this algorithm should always favor considering ectopic if there is any evolution or change in a patient's clinical exam[8]
| Clinical Signs and Symptoms | Risk Group | Percent Risk of Ectopic (%) |
| Peritoneal irritation or cervical motion tenderness | High | 29 |
| No fetal heart tones; no tissue at cervical os; pain present | Intermediate | 7 |
| Fetal heart tones or tissue at cervical os; no pain | <1 |
Step one
- Assess for Shock
- Beware that paradoxical bradycardia can be present with significant hemoperitoneum[10]
- If patient is a high risk for ectopic based on above estimation then immediately contact OBGYN
Step Two
Perform a Pelvic US
- Consider Transabdominal Ultrasound for B-HCG: >6000 mIU/ml (but if negative or indeterminate must do Pelvic ultrasound regardless of B-HCG)
Is there an Intrauterine Pregnancy?
- If there is an IUP and there was no assisted reproductive fertility used then ectopic ruled out and heterotopic unlikely (less than 1:30,000)[11]
- If fertility assistance was used then still consider a heterotopic (1% risk)[12]
Step Three
- If HCG above Discriminatory Zone (>1,500-3,000 mIU/ml) and not visualized it should be an ectopic pregnancy until proven otherwise
Step Four
- Arrange close follow-up for patients with no visualized IUP and B-HCG( (<1,500-3,000 mIU/ml), with minimal to no pain and hemodynamically stable.
- Patients should have a 48hr repeat B-HCG level checked to determine if appropriate doubling is occurring.
Repeat B-hCG Levels
| Pregnancy Type | B-hCG Change |
| Normal |
|
| Ectopic |
|
| Miscarriage |
|
- A single hCG level cannot reliably distinguish intrauterine from ectopic pregnancy[17]
- The discriminatory zone (typically 1,500-3,500 mIU/mL depending on institution) is the hCG level above which a gestational sac should be visible on transvaginal ultrasound[18]
Management
Emergency Treatment
- OB/GYN Consult
- RhoGAM for all Rh-negative women
- If unstable:
- Urgent surgical laparotomy
- Consider T&S and/or blood transfusion (e.g., MTP) as temporizing measure
Definitive Treatment
- Medical management with methotrexate (ACOG)
- Single dose regimen[19]
- Methotrexate 50mg/m2 IM day 1
- If hCG decreases by <15% between days 4 and 7, another 50mg/m2 IM methotrexate on day 7
- Absolute contraindications
- Breast-feeding
- Laboratory evidence of immunodeficiency
- Preexisting blood dyscrasias (bone marrow hypoplasia, leukopenia, thrombocytopenia, or clinically significant anemia)
- Known sensitivity to methotrexate
- Active pulmonary disease
- Peptic ulcer disease
- Hepatic, renal, or hematologic dysfunction
- Alcoholism
- Alcoholic or other chronic liver disease
- Coexistant viable IUP
- Does not have timely access to medical institution, or unwilling/unable to comply with post-MTX monitoring
- Relative contraindications
- Adnexal mass >3.5 cm in largest diameter
- Presence of fetal heart rate
- Free fluid visualized in Pouch of Douglas
- Beta-HCG >5000mIU/mL
- Note: Need to counsel patient to return after 4 and 7 days to recheck hCG values to check for satisfactory decline
- Also note that 30-60% of women experience "separation pain" ~1 week after starting methotrexate[20]
- Thought to be due to tubal distention from tubal abortion or hematoma formation
- Nevertheless, presentation of abdominal pain at this time still warrants an US to look for tubal rupture, which may be indicated by increase in pelvic free fluid, decrease in Hb
- Size of ectopic mass may actually increase before involution, and this is not associated with treatment failure
- Single dose regimen[19]
- Surgical treatment
- Laparascopic salpingectomy or salpingostomy
Disposition
- Most are admitted and/or go to the OR
- Smaller, minimally symptomatic ectopic pregnancies being treated with methotrexate may be discharged in consultation with OB/GYN
Medication Dosing
- Methotrexate 50 mg/m2 IM IM — Repeat on day 7 if hCG decreases <15% between days 4-7; see ACOG contraindications
See Also
External Links
References
- ↑ Centers for Disease Control and Prevention. Current trends ectopic pregnancy - United States, 1990-92. MMWR Morb Mortal Wkly Rep. 1995; 44:46-48.
- ↑ Houry D and Keadey M. Complications in pregnancy part I: Early pregnancy. EBM. 2007; 9(6):1-28.
- ↑ Ankum WM, Mol BW, Van der Veen F, Bossuyt PM. Risk factors for ectopic pregnancy: a meta-analysis. Fertil Steril. 1996;65:1093–9
- ↑ Mol BW, Ankum WM, Bossuyt PM, Van der Veen F. Contraception and the risk of ectopic pregnancy: a meta-analysis. Contraception. 1995;52:337–41.
- ↑ Norris DL, Young JD. UTI. EM Clin N Am. 2008; 26:413-30.
- ↑ http://www.thepocusatlas.com/obgyn/
- ↑ Lozeau AM, Potter B. Diagnosis and management of ectopic pregnancy. Am Fam Physician. 2005;72;1707-1714, 1719-1720
- ↑ American College of Obstetricians and Gynecologists. Medical management of tubal pregnancy. Number 3, December 1998. Clinical management guidelines for obstetricians-gynecologists. Int J Gynaecol Obstet. 1999;65:97–103
- ↑ Buckley RG, King K et. al. History and physical examination to estimate the risk of ectopic pregnancy: validation of a clinical prediction model. Ann Emerg Med. 1999;34:589–94
- ↑ Hick JL, et al. Vital signs fail to correlate with hemoperitoneum from ruptured ectopic pregnancy. The American Journal of Emergency Medicine. 2001; 19(6)488–491.
- ↑ Mukul LV, Teal SB. Current management of ectopic pregnancy. Obstet Gynecol Clin N Am. 2007; 34:403-419.
- ↑ Yeh HC, Goodman JD, Carr L, et al. Intradecidual sign: a ultrasound criterion of early intrauterine pregnancy. Radiology. 1986;161:463-467
- ↑ Barnhart KT, Sammel MD, Rinaudo PF, et al. Symptomatic patients with an early viable intrauterine pregnancy: HCG curves redefined. Obstet Gynecol. 2004; 104(1):50-55. PMID 15229000.
- ↑ Barnhart KT, Guo W, Cary MS, et al. Differences in serum human chorionic gonadotropin rise in early pregnancy by race and value at presentation. Obstet Gynecol. 2016; 128(3):504-511. PMID 27500347.
- ↑ Silva C, Sammel MD, Zhou L, et al. Human chorionic gonadotropin profile for women with ectopic pregnancy. Obstet Gynecol. 2006; 107(3):605-610. PMID 16507930.
- ↑ Doubilet PM, Benson CB, Bourne T, Blaivas M. Diagnostic criteria for nonviable pregnancy early in the first trimester. N Engl J Med. 2013; 369(15):1443-1451. PMID 24106937.
- ↑ Murray H, Baakdah H, Bardell T, Tulandi T. Diagnosis and treatment of ectopic pregnancy. CMAJ. 2005; 173(8):905-912. PMID 16217116.
- ↑ Connolly A, Ryan DH, Stuber AR, Postma HJ. Reevaluation of discriminatory and threshold levels for serum beta-hCG in early pregnancy. Obstet Gynecol. 2013; 121(1):65-70. PMID 23262929.
- ↑ Bachman EA and Barnhart K. Medical Management of Ectopic Pregnancy: A Comparison of Regimens. Clin Obstet Gynecol. 2012 Jun; 55(2): 440–447.
- ↑ Lipscomb GH et al. Management of separation pain after single-dose methotrexate therapy for ectopic pregnancy. Obstet Gynecol. 1999 Apr;93(4):590-3.