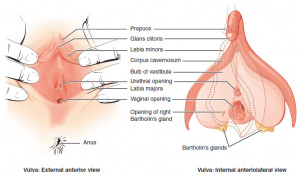
Atrophic vaginitis
Background
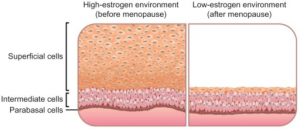
Influence of estrogen on the vaginal epithelium. Before menopause, high levels of estrogen stimulate maturation of the vaginal epithelium to generate a thick layer of mature superficial cells. After menopause, lack of estrogen leaves the epithelium much thinner, with very few or no superficial cells.
- Also known as: vulvovaginal atrophy, vaginal atrophy, genitourinary syndrome of menopause, and estrogen deficient vaginitis
- Primarily occurs in peri or postmenopausal women
Risk Factors
- Conditions or medications that induce a low estrogen state:
- Natural menopause
- Bilateral oophorectomy
- Spontaneous premature ovarian failure
- Ovarian failure due to radiation or chemo
- Medications: tamoxifen, danazol, medroxyprogesterone, leuprolide, ganirelix
- Postpartum reduction in estrogen production
- Prolactin elevation
Clinical Features
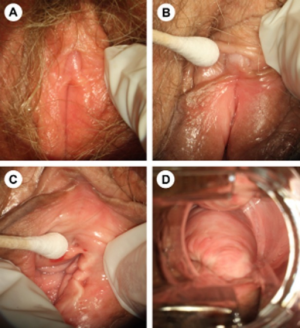
Atrophy of the vulva, clitoris, and vagina consistent with atrophic vaginitis. (A) Vaginal atrophy is associated with pale, dry, shiny vulvar tissue and loss of adipose tissue in the labia majora and labia minora. (B) The prepuce and clitoris are often pale and reduced in size, while examination shows that (C) the introitus may be narrowed and friable. (D) In vaginal atrophy, the vaginal walls lack rugae and may be pale and/or erythematous.
Symptoms are generally progressive and gradually worsen as women progress through menopause
- Vaginal dryness
- Vaginal burning/irritation
- Decreased vaginal lubrication
- Dyspareunia
- Vulvar or vaginal bleeding
- Vaginal discharge
- Pelvic pressure
- UTI symptoms or recurrent UTIs
Differential Diagnosis
- Infection (candidiasis, bacterial vaginosis, trichomoniasis, desquamative inflammatory vaginitis)
- Reaction to irritants (soaps, deodorants, lubricants, clothing)
- Vulvovaginal lichen planus
- Vulvar lichen sclerosus
- If bleeding present, malignancy should be excluded
Vulvovaginitis
- Bacterial vaginosis
- Candida vaginitis
- Trichomonas vaginalis
- Contact vulvovaginitis
- Bubble baths and soaps
- Deodorants, powders, and douches
- Clothing
- Atrophic vaginitis due to lack of estrogen (AKA Vulvovaginal atrophy)
- Lichen sclerosus
- Tinea cruris
- Chlamydia/Gonorrhea infection
- Pinworms
- Vaginal foreign body
- Toilet paper
- Other
- Genitourinary syndrome of menopause
- Foreign body
- Allergic reaction
- Normal physiologic discharge
Evaluation
- History
- Menstrual and medication history to assess for causes of hypoestrogenism
- Complete ROS to rule out other causes of urogenital symptoms
- Consider symptoms that may be secondary to infection, inflammation, local irritation
- Ask about history of pelvic radiation
- Thorough sexual history
- Pelvic Exam
- External genitalia may show scarce pubic hair, diminished elasticity, introital narrowing, or fusion of labia minora
- Loss of labial fat pad
- Pale, dry epithelium that is smooth and shiny with loss of rugation
- Use caution as exam can cause pain and bleeding
- Assess for introital stenosis with gloved finger before inserting speculum
- Labs
- Not usually necessary in ED unless concern for other causes
Management
- Topical estrogen cream or tablets[1]
- Generic estradiol 10-mcg insert vaginally daily x 2 weeks, then twice weekly indefinitely (lower cost option)
- May take as long as 2-3 months to see maximal benefit
- Warm patients about possible side effects of breast or perineal pain and uterine bleeding
- Should not be used if history of cancer to reproductive organs or postmenopausal bleeding
Disposition
- Refer to gynecologist
References
- ↑ Winter et al, UTIs and Estrogen: the Overlooked Link https://www.acepnow.com/article/utis-and-estrogen-the-overlooked-link/