Bacterial vaginosis
Background
- Is a vaginal dysbiosis resulting from replacement of the normally dominant Lactobacillus species in the vagina, with high concentrations of anaerobic bacteria.
- Is not an infection, nor is it sexually transmitted, although it is associated with sexual activity.
- Accounts for up to 50% of cases of vaginitis
- Associated with preterm labor and premature rupture of membranes
Clinical Features
- Whitish-gray vaginal discharge and odor
- Lack of discharge makes diagnosis less likely
- May have history of "physiologic whiff test" after contact with male ejaculate which is alkaline (like KOH)
Differential Diagnosis
Vulvovaginitis
- Bacterial vaginosis
- Candida vaginitis
- Trichomonas vaginalis
- Contact vulvovaginitis
- Bubble baths and soaps
- Deodorants, powders, and douches
- Clothing
- Atrophic vaginitis due to lack of estrogen (AKA Vulvovaginal atrophy)
- Lichen sclerosus
- Tinea cruris
- Chlamydia/Gonorrhea infection
- Pinworms
- Vaginal foreign body
- Toilet paper
- Other
- Genitourinary syndrome of menopause
- Foreign body
- Allergic reaction
- Normal physiologic discharge
Evaluation
Work-up
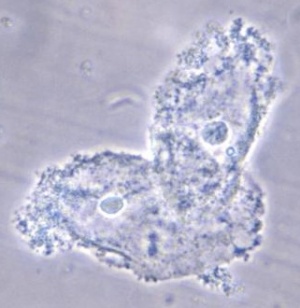
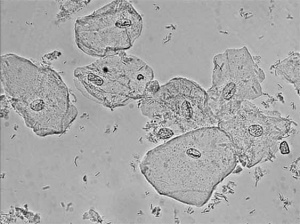
- Wet mount shows clue cells: vaginal epithelial cells with "stippled appearance" due to coverage by bacteria
- Whiff Test: fishy odor with 10% KOH prep
- CDC recommends testing all women with BV for HIV and other STDs [1]
Diagnosis
Amsel criteria (3/4 must be present)
- Homogeneous, thin, gray-white discharge
- Positive whiff test
- Vaginal pH>4.5
- Clue cells on wet mount (at least 20% of epithelial cells)
Management
- No need to treat if asymptomatic
- In pregnant patients, consider treating to prevent preterm birth, though evidence is conflicting[2]
- Consider partner treatment to reduce risk of recurrence[3]
- Does not need a test of cure
Antibiotics
First Line Therapy[4]
- Metronidazole 500 mg PO Twice Daily for 7 days OR
- Metronidazole gel 0.75%, one full applicator (5 g) intravaginally, Daily for 5 days OR
- Clindamycin cream 2%, one full applicator (5 g) intravaginally Nightly for 7 days
Metronidazole does not cause a disulfiram-like reaction with alcohol.[5]
Alternative Regimin
- Clindamycin 300 mg PO BID for 7 days OR
- Clindamycin ovules 100 mg intravaginally qHS for 3 days (do not use if patient has used latex condom in last 72 hours)
Other regimens have been studied and have varying efficacy compared to placebo but due to cost and availability do not represent alternatives outside of absolute contraindications to preferred regimens.
Pregnant
- Metronidazole 500mg PO Twice a day x 7 days[4]
- Metronidazole 250mg PO Three times a day has also been studied[6][7]
- Although metronidazole crosses the placenta, no evidence of teratogenicity or mutagenic effects among infants has been reported in multiple cross-sectional, case-control, and cohort studies of pregnant women[4]
Prophylaxis (Sexual Assault)
- Metronidazole 500mg PO Twice a day x 7 days[8]
Disposition
- Discharge
See Also
References
- ↑ Workowski KA, Bachmann LH, Chan PA, et al. Sexually Transmitted Infections Treatment Guidelines, 2021. MMWR Recomm Rep. 2021;70(4):1-187. doi:10.15585/mmwr.rr7004a1
- ↑ Cochrane Database of Systemic REviews. January 2013. Antibiotics for treating bacterial vaginosis in pregnancy. https://www.ncbi.nlm.nih.gov/pubmedhealth/PMH0010584/
- ↑ Vodstrcil LA, et al. Male-Partner Treatment to Prevent Recurrence of Bacterial Vaginosis. N Engl J Med. 2025 Mar 6;392(10):947-957. doi: 10.1056/NEJMoa2405404. PMID: 40043236.
- ↑ 4.0 4.1 4.2 CDC Sexually Transmitted Infections Treatment Guidelines, 2021.[1]
- ↑ Is combining metronidazole and alcohol really hazardous?[2]
- ↑ Reduced incidence of preterm delivery with metronidazole and erythromycin in women with bacterial vaginosis[3]
- ↑ Effect of metronidazole in patients with preterm birth in preceding pregnancy and bacterial vaginosis: a placebo-controlled, double-blind study[4]
- ↑ Sexual Assault and Abuse and STIs – Adolescents and Adults[5]