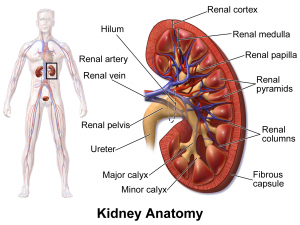
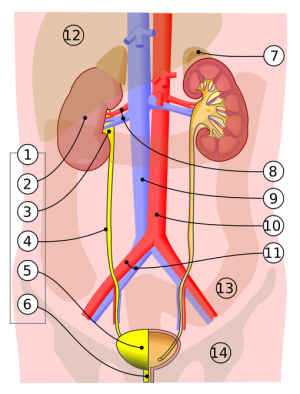
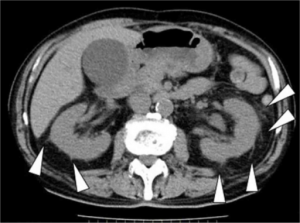
Pyelonephritis
Background
Definitions
- UTI = significant bacteriuria in presence of symptoms
- Described by location: urethritis, cystitis, or pyelonephritis
Genitourinary infection
"UTI" frequently refers specifically to acute cystitis, but may also be used as a general term for all urinary infections; use location-specific diagnosis.
- Renal/perirenal
- Ureteral
- Infected urolithiasis
- Bladder
- Acute cystitis ("UTI")
- Chronic cystitis
- Urethra/periurethra
Clinical Features
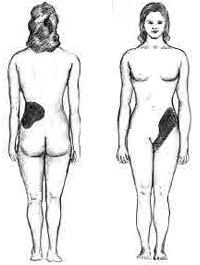
Diagram showing the typical location of pain[1]
- Pyelo = Cystitis symptoms AND fever/chills/nausea/vomiting
- CVAT alone may be referred pain from cystitis
- CVAT is only physical examination finding that increases likelihood of a UTI
Complications
- Acute bacterial nephritis
- CT shows ill-defined focal areas of decreased density
- Renal/Perinephric abscesses
- Sign/symptoms similar to pyelo (fever, CVAT, dysuria)
- Occurs in setting of ascending infection with obstructed pyelo
- Associated with DM and Renal Stones
- Also occurs due to bacteremia with hematogenous seeding (Staph)
- Emphysematous pyelonephritis
Differential Diagnosis
Major
- Acute cystitis
- Infected kidney stone
Flank Pain
- Vascular
- Abdominal aortic aneurysm
- Renal artery embolism
- Renal vein thrombosis
- Aortic dissection
- Mesenteric ischemia
- Renal
- Pyelonephritis
- Perinephric abscess
- Perinephric hematoma
- Papillary necrosis
- Renal cell carcinoma
- Obstructive uropathy
- May or may not be due to nephrolithiasis
- Renal infarction
- Renal hemorrhage
- Ureter
- Nephrolithiasis
- Blood clot
- Stricture
- Tumor (primary or metastatic)
- Bladder
- Tumor
- Varicose vein
- Cystitis
- GI
- Biliary colic
- Pancreatitis
- Perforated peptic ulcer
- Appendicitis (appendix may be pushed to RUQ in pregnancy)
- Inguinal Hernia
- Diverticulitis
- Cancer
- Bowel obstruction
- Gynecologic
- Ectopic Pregnancy
- PID/TOA
- Ovarian cyst
- Ovarian torsion
- Endometriosis
- Mittelschmerz or benign ovulatory pain
- GU
- Other
- Shingles
- Lower lobe pneumonia
- Retroperitoneal hematoma, abscess, or tumor
- Epidural abscess
- Epidural hematoma
- Rib contusion/fracture
Dysuria
- Genitourinary infection
- Acute cystitis ("UTI")
- Pyelonephritis
- Urethritis
- Chronic cystitis
- Infected nephrolithiasis
- Prostatitis
- Epididymitis
- Renal abscess/perinephric abscess
- Emphysematous pyelonephritis
- Nephrolithiasis
- Urethral issue
- Urethritis
- Urolithiasis
- Urethral foreign body
- Urethral diverticulum
- Allergic reaction (contact dermatitis)
- Chemical irritation
- Urethral stricture or obstruction
- Trauma to vagina, urethra, or bladder
- Gynecologic
- Vaginitis/cervicitis
- PID
- Genital herpes
- Pelvic organ prolapse
- Fistula
- Cystocele
- Other
- Diverticulitis
- Interstitial cystitis
- Behavioral symptom without detectable pathology
Evaluation
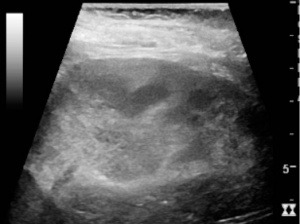
Renal ultrasound showing acute pyelonephritis with increased cortical echogenicity and blurred delineation of the upper pole.[2]
Workup
- Urinalysis
- Urine culture
- Consider imaging (CT or ultrasound) if any of the following:
- CT sensitivity 72%, specificity 58%[3]
- History of Renal Stone
- Poor response to antibiotics
- Male
- Elderly
- Diabetic
- Severely ill
- Blood cultures are NOT indicated (organisms in blood culture matched those in urine culture 97% of time)
Diagnosis
- Urinalysis
- Clumps and/or high WBCs
- Nitrite
- Very high specificity (>90%) in confirming diagnosis of UTI
- Low sensitivity (enterococcus, pseudomonas, acinetobacter are not detected)
Management
Antibiotics
Treatment is targeted at E. coli, Enterococcus, Klebsiella, Proteus mirabilis, S. saprophyticus.
Outpatient
Consider one dose of Ceftriaxone 1g IV or Gentamicin 7mg/kg IV if the regional susceptibility of TMP/SMX or Fluoroquinolones is <80%
- Ciprofloxacin 500mg PO BID x7 days OR
- Trimethoprim-Sulfamethoxazole DS 160/800mg PO BID x14 days OR[4]
- Cephalexin 500mg QID PO x 10-14 days (OR consider 1000mg BID) OR
- Cefdinir 300mg BID PO x 10-14 days OR
- Cefpodoxime 200mg PO BID x 10 days OR[5]
- Cefixime 400mg PO daily x 10 days OR[6]
- Levofloxacin 750mg PO QD x7 days[7]
Adult Inpatient Options
- Ciprofloxacin 400mg IV q12hr OR
- Ceftriaxone 1gm IV QD (Preferred in pregnancy) OR
- Cefotaxime 1-2gm IV q8hr OR
- Gentamicin 3mg/kg/day divided q8hr +/- ampicillin 1–2 gm q4hr OR
- Piperacillin/Tazobactam 3.375 gm IV q6hr OR
- Cefepime 2gm IV q8hr OR
- Imipenem/Cilastatin 500mg IV q8hr
Pediatric Outpatient Options
- Cephalexin 25-50mg/kg/day PO divided q6-8h x 10-14 days (max 500mg/dose) OR
- Cefixime 8mg/kg PO daily x 10-14 days (max 400mg) OR
- Cefdinir 14mg/kg/day PO divided BID x 10 days (max 600mg/day) OR
- Cefpodoxime 10mg/kg/day PO divided BID x 10 days (max 200mg/dose) OR
- TMP/SMX 6-12mg/kg/day (TMP) PO divided BID x 10-14 days
Pediatric Inpatient Options
- Ceftriaxone 75mg/kg IV QD OR
- Cefotaxime 50mg/kg IV q8hrs OR
- Ampicillin 25mg/kg IV q6hrs + 2.5mg/kg IV q8hrs
- Ampicillin/Sulbactam 3g IM/IV q6 hours x 14 days
Disposition
Discharge
- Consider if young, otherwise healthy, tolerating PO
Admission
Consider admission if:[8]
- Elderly (>60)
- Renal Calculi
- Obstruction
- Recent hospitalization/instrumentation
- DM
- Immunocompromised
- Unable to tolerate PO
- Pregnancy
- Solitary kidney or other anatomic abnormality
Disposition
- Admit all second trimester pregnant patients with OBGYN consult
- Urology consult during the inpatient admission for pediatric patients due to the risk for urologic scarring
- Consider advanced imaging to rule out abscess of urolithiasis if patient has failed 3 days of therapy
Special Populations
Elderly
- Elderly patients with pyelonephritis: 20% present with primary respiratory or GI symptoms. Also 33% are afebrile.[9]
See Also
References
- ↑ Urinary Tract Infection Common Clinical and Laboratory Features of Acute Pyelonephritis". netterimages.com. Retrieved 14 July 2019.
- ↑ Content initially copied from: Hansen, Kristoffer; Nielsen, Michael; Ewertsen, Caroline (2015). "Ultrasonography of the Kidney: A Pictorial Review". Diagnostics. 6 (1): 2. doi:10.3390/diagnostics6010002. ISSN 2075-4418. PMC 4808817. PMID 26838799. (CC-BY 4.0)
- ↑ Perirenal fat stranding is not a powerful diagnostic tool for acute pyelonephritis International Journal of General Medicine
- ↑ Gupta K, Hooton TM, Naber KG, et al. International Clinical Practice Guidelines for the Treatment of Acute Uncomplicated Cystitis and Pyelonephritis in Women. Clinical Infectious Diseases. 2011;52(5):e103-e120. doi:10.1093/cid/ciq257
- ↑ Colgan R, Williams M. Diagnosis and treatment of acute uncomplicated cystitis. Am Fam Physician. 2011 Oct 1;84(7):771-6.
- ↑ Acute Pyelonephritis in Adults. Johnson, JR and Russo, TA. New England Journal of Medicine 2018; 378:48-59.
- ↑ Sandberg T. et al. Ciprofloxacin for 7 days versus 14 days in women with acute pyelonephritis: a randomised, open-label and double-blind, placebo-controlled, non-inferiority trial. Lancet. 2012 Aug 4;380(9840):484-90.
- ↑ Norris DL, Young JD. UTI. EM Clin N Am. 2008; 26:413-30.
- ↑ Norris DL, Young JD. UTI. EM Clin N Am. 2008; 26:413-30.