Bronchiolitis (peds)
Background
- Most common reason for infant hospitalizations in the US[1]
- Respiratory syncytial virus (RSV) causes ~70% of cases of bronchiolitis[2]
- <2yr old (peak 2-6mo age)
- Preemies, neonates, congenital heart disease are at risk for serious disease
- Peaks in winter (November to March)
- Duration = 7-14d (worst during days 3-5)
- Inflammation, edema, mucus production, and epithelial necrosis of bronchioles lead to lower airway obstruction
- Hypoxemia due to V/Q mismatch of poorly ventilated alveolar units
Clinical Features
- Symptoms
- Rhinorrhea, cough, irritability, apnea (neonates)
- Signs
- Tachypnea, cyanosis, wheezing, respiratory distress (retractions, nasal flaring)
- Fever is usually low-grade or absent
- If high-grade fever consider otitis media, UTI, or other bacterial infections
- Assess for dehydration (tachypnea may interfere with feeding)
- Sunken fontanelle, decreased PO intake, decreased wet diapers, and lethargy
Differential Diagnosis
Pediatric Shortness of Breath
Pulmonary/airway
- Airway obstruction
- Structural
- Infectious
- Other
Cardiac
- Congenital heart disease
- Vascular ring
- Cardiac tamponade
- Congestive Heart Failure (peds)
- Myocarditis (peds)
Other diseases with abnormal respiration
- Normal neonatal periodic breathing (misinterpreted by caregivers as abnormal)
- Brief resolved unexplained event
- Anemia
- Abdominal distension (e.g. SBO, liver failure
- Neonatal abstinence syndrome
- Decreased perfusion states
- Metabolic acidosis
- CO Poisoning
- Diaphragm injury
- Renal Failure
- Electrolyte abnormalities
- Organophosphate toxicity
- Tick paralysis
- Fever (Peds)
- Panic attack
- Porphyria
Evaluation
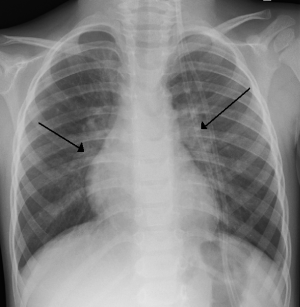
CXR of a child with RSV showing the typical bilateral perihilar fullness.
- Bronchiolitis is a clinical diagnosis
- Consider rapid RSV testing
- Consider CBC and CRP to assess the risk of superimposed bacterial infection
- CXR
- Not routinely necessary : May lead to unnecessary use of antibiotics (atelectasis from airway plugging mimics infiltrate)
- Consider if patient is critically ill or diagnosis unclear
Concurrent infection risk
Infants <60 days with RSV bronchiolitis and fever
- Low risk of bacteremia and meningitis in RSV+, still appreciable UTI risk
- UTI 5.4% in RSV+, 10.1% RSV-
- Bacteremia 1.1% RSV+, 2.3% RSV-
- Meningitis 0% RSV+, 0.9% RSV-
- Recommended to still obtain UA in cases of bronchiolitis w/ fever. BCx and CSF not necessary if >28 days old
Management
- Note that supportive care remains the mainstay of therapy
- Hydration for all infants
Oxygen/High Flow
It is reasonable to not perform continuous oximetry on infants and children with bronchiolitis[7]
- O2 (maintain SaO2 >90%)
- Oxygen saturation alone should not dictate admission (for patients with O2 sat of 88% or above)[8]
- High flow nasal cannula
- Multicenter randomized trial showed infants with bronchiolitis and hypoxemia required less escalation of therapy than standard oxygen [9]
- Primary benefits is from the high flow rate; optimize the flow upon initiation.
- Initial Settings
- Temperature: 37C (usually)
- Initial flow rate: Based on age/weight. Can be started at 1-2 L/kg per min.
- Oxygen (FiO2): 21% to 100%, based on patient’s prior oxygenation; goal of 94% to 99%.
- Nasal CPAP or intubation may be necessary for evolving respiratory failure
Suctioning
There is insufficient data to make an evidence-based recommendation about suctioning.
- Nasopharyngeal suctioning may temporarily relieve symptoms due to decrease in total airway resistance
- The use of routine “deep” suctioning may lead to increased length of stay based on one small study [7]
Nebulized Hypertonic Saline (3%)
AAP recommends as a possible intervention, but 2014 SABRE trial found no change in discharge or adverse events with nebulised HS.[10]
- No decrease in hospital admission in 2017 multi-center, RCT for moderate-severe bronchiolitis, with mild adverse events such as worsening of cough were significantly higher in the HS group[11]
- Only consider administering to infants who require hospitalization[7] (Class B))
- Suction nares / nasal saline drops
Not Indicated
Randomized controlled trials of bronchodilator or corticosteroid therapy have shown mixed results. Bronchodilators could aggravate the symptoms.[12][13][14]
- Albuterol/bronchodilator (Class B)[7]
- May trial if strong family hx of asthma/atopy in older infants, as this may present a greater reactive airway component
- Racemic Epinephrine (Class B)[7]
- Steroids[7][15]
- Consider dexamethasone 0.6-1mg/kg PO or IM x1 in severe cases
- Note that AAP recommends against systemic steroids in any settings[16]
- Antibiotics
- Only indicated if there is strong suspicion of, or proven bacterial infection
Disposition
Consider Admission
- Age <3 months
- Preterm (<34wks)
- Underlying heart/lung disease
- Initial SaO2 <88% [8]
- Sa02 alone should not alone be used as a factor for admission
- Unable to tolerate PO
- Tachypnea with accessory muscle use
- Caregiver unreliable or otherwise unstable home situation
See Also
External Links
- Pediatric Emergency Playbook Podcast: Bronchiolitis
- PEM Morsels: Bronchiolitis Archives
- CDC: Respiratory Syncytial Virus
References
- ↑ Suh M, Movva N, Jiang X, Bylsma LC, Reichert H, Fryzek JP, Nelson CB. Respiratory Syncytial Virus Is the Leading Cause of United States Infant Hospitalizations, 2009-2019: A Study of the National (Nationwide) Inpatient Sample. J Infect Dis. 2022 Aug 15;226(Suppl 2):S154-S163. doi: 10.1093/infdis/jiac120. PMID: 35968878; PMCID: PMC9377046.
- ↑ Papadopoulos NG; Moustaki M; Tsolia M; Bossios A; Astra E; Prezerakou A (2002). Am J Respir Crit Care Med.
- ↑ Well-appearing Young Infants with RSV Infection: Guidance Related To Criteria for Admission. Harbor-UCLA Pediatric Infectious Diseases, October 2017
- ↑ Schroeder AR, et al. Pediatrics 2013;132:e1194-201
- ↑ Well-appearing Young Infants with RSV Infection: Guidance Related To Criteria for Admission. Harbor-UCLA Pediatric Infectious Diseases, October 2017
- ↑ Schroeder AR, et al. Pediatrics 2013;132:e1194-201
- ↑ 7.0 7.1 7.2 7.3 7.4 7.5 Ralston S. et al. Clinical Practice Guideline: The Diagnosis, Management, and Prevention of Bronchiolitis. Pediatrics 134(5) Nov. 2014. 1474 -e150 doi: 10.1542/peds.2014-2742 PDF
- ↑ 8.0 8.1 Schuh S. et al. Effect of oximetry on hospitalization in bronchiolitis: a randomized clinical trial. JAMA. 2014 Aug 20;312(7):712-8. doi: 10.1001/jama.2014.8637
- ↑ Franklin, D., Babl, F. E., Schlapbach, L. J., Oakley, E., Craig, S., Neutze, J., … Schibler, A. (2018). A Randomized Trial of High-Flow Oxygen Therapy in Infants with Bronchiolitis. The New England Journal of Medicine, 378(12), 1121–1131.
- ↑ Everard ML, Hind D, Ugonna K, et al. SABRE: a multicentre randomised control trial of nebulised hypertonic saline in infants hospitalised with acute bronchiolitis. Thorax. 2014;69(12):1105–1112. doi:10.1136/thoraxjnl-2014-205953.
- ↑ Angoulvant F et al. Effect of Nebulized Hypertonic Saline Treatment in Emergency Departments on the Hospitalization Rate for Acute BronchiolitisA Randomized Clinical Trial. June 5, 2017. JAMA Pediatr. Published online June 5, 2017. doi:10.1001/jamapediatrics.2017.1333.
- ↑ Bjornson CL. et al. A randomized trial of a single dose of oral dexamethasone for mild croup. NEJM. 2004;351:1306-1313.
- ↑ Geelhoed GC. et al. Efficacy of a small single dose of oral dexamethasone for outpatient croup: a double blind placebo controlled clinical trial. BMJ. 1996;313:140-142
- ↑ Ralston S. et al. Randomized, placebo-controlled trial of albuterol and epinephrine at equipotent beta-2 agonist doses in acute bronchiolitis. Pediatr Pulmonol. 2005;40:292-299
- ↑ Corneli HM, Zorc JJ, Mahajan P, et al; Bronchiolitis Study Group of the Pediatric Emergency Care Applied Research Net- work (PECARN). A multicenter, random- ized, controlled trial of dexamethasone for bronchiolitis [published correction appears in N Engl J Med 2008;359(18): 1972]. N Engl J Med. 2007;357(4):331–339
- ↑ Clinical Practice Guideline: The Diagnosis, Management, and Prevention of Bronchiolitis. Pediatrics November 2014; 134 (5): e1474–e1502. 10.1542/peds.2014-2742