Congestive heart failure (peds)
(Redirected from Congestive Heart Failure (peds))
This page is for pediatric patients. For adult patients, see: congestive heart failure
Background
- Pediatric congestive heart failure (CHF) affects 12,000-35,000 children in the United States each year[1]
- The causes and clinical presentation varies differently compared to adults
Causes
- Structural
- Acquired
- Arrhythmia
- Cardiomyopathy
- Myocarditis (peds)
- Myocardial ischemia (rare)
- Drugs/toxins
- Systemic lupus erythematosus
Clinical Features
Symptoms[2]
- Difficulty breathing
- Feeding difficulty - irritability with feeding, prolonged feeding time, refusal to feed
- If an infant has to decide between feeding and breathing, he/she will choose to breathe
- Sweating with feeds
- "Exercise intolerance"
- Failure to thrive
- Fussiness
- Older children: fatigue, exercise intolerance, dyspnea, orthopnea, abdominal pain, dependent edema[3]
Physical Exam
- Tachycardia
- Tachypnea with labored breathing and accessory muscle use
- Grunting with nasal flaring
- Rales
- S3 gallop
- Hepatomegaly
- Cyanosis, cool/mottled extremities
- Decreased capillary refill
- Edema of face and limbs
Differential Diagnosis
Pulmonary/airway
- Airway obstruction
- Anaphylaxis, angioedema
- Aspirated foreign body
- Asthma exacerbation
- Pneumonia
- Pneumothorax
- Respiratory distress syndrome
- Meconium aspiration syndrome
- Bronchiolitis (peds), URI
- Pertussis
- Bronchopulmonary dysplasia
- Croup
- Epiglottitis
- Bacterial tracheitis
- Tracheomalacia
- Cystic fibrosis exacerbation
- Pulmonary edema
- Pulmonary hypertension, cor pulmonale
- Inhalation exposure
- Rib fractures, Flail chest, pulmonary contusion
- Nonaccidental trauma
Cardiac
Other diseases with abnormal respiration
- Normal neonatal periodic breathing (misinterpreted by caregivers as abnormal)
- Brief resolved unexplained event
- Anemia
- Neonatal abstinence syndrome
- Decreased perfusion states
- Metabolic acidosis
- CO Poisoning
- Diaphragm injury
- Renal Failure
- Electrolyte abnormalities
- Fever (Peds)
Evaluation
Workup
- Blood Work
- CBC
- BMP
- Mg
- LFT
- BNP
- Troponin
- Blood gas
- Inflammatory markers such as ESR/CRP if concern for myocarditis, although these are nonspecific
- EKG
- Sinus tachycardia - most common
- May find other etiologies to CHF such as ECG abnormalities pointing towards myocarditis, restrictive cardiomyopathy, heart block, arrhythmias
- CXR
- Will help assess for cardiomegaly, pulmonary congestion, interstitial edema, pleural effusions
Diagnosis
- Definitive diagnosis typically via echocardiography
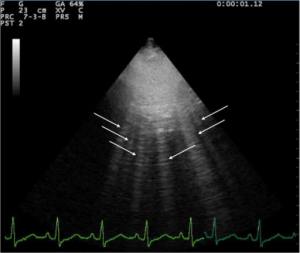
Lung ultrasound of pulmonary edema
- A lines and B lines
- A lines:
- Appear as horizontal lines
- Indicate dry interlobular septa.
- Predominance of A lines has 90% sensitivity, 67% specificity for pulmonary artery wedge pressure <= 13mm Hg
- A line predominance suggests that intravenous fluids may be safely given without concern for pulmonary edema
- B lines ("comets"):
- White lines from the pleura to the bottom of the screen
- Highly sensitive for pulmonary edema, but can be present at low wedge pressures
- A lines:
Management
- Management tailored to severity of disease
- Noninvasive ventilation
- HFNC
- CPAP
- BiPAP
- Diuretics
- Inotropes/Catecholamines
- To be used if cardiac function significantly depressed
- Dopamine (preferred drug for decompensated CHF)
- Low dose Epinephrine for refractory hypotension
- Pediatric Cardiology consult
Disposition
- In general CHF exacerbation will require admission
- NICU/PICU if unstable
See Also
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5105230/
- https://www.pedscases.com/congenital-congestive-heart-failure
- https://pedemmorsels.com/tag/congenital-heart-disease/
External Links
References
- ↑ Rossano JW, Kim JJ, Decker JA, et al. Prevalence, morbidity, and mortality of heart failure-related hospitalizations in children in the United States: a population-based study. J Card Fail 2012; 18:459
- ↑ Judge et al. Congenital Heart Disease In Pediatric Patients: Recognizing The Undiagnosed And Managing Complications In The Emergency Department. Pediatr Emerg Med Pract. 2016. May;13(5):1-28
- ↑ Jayaprasad. Heart Failure in Children. Heart Views. 2016 Jul-Sep;17(3):92-99