Dehydration (peds)
This page is for pediatric patients. For adult patients, see: dehydration
Background
1kg body wt = to 1 liter fluid
Clinical Features
- Decreased urine output
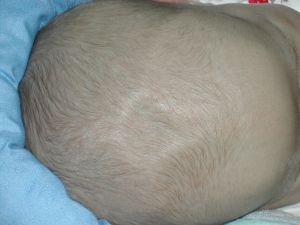
- Sunken fontanelle
- Most reliable: [1]
- Abnormal capillary refill
- Abnormal respiratory pattern
- Decreased skin turgor
Differential Diagnosis
Evaluation
Management
- Ondansteron for vomiting
- Mild to moderate dehydration: start with trial of oral rehydration therapy or half strength apple juice[2][3]
- Part of ACEP Choosing wisely
- Provide ORS solution (e.g. Pedialyte) at 50 to 100 mL/kg over 2-4 hours in small doses q5min
- If the child vomits, wait 15 minutes then try again
- Provide additional ORS to replace ongoing GI losses
- Consider Fluid Repletion (IVF) only if severely dehydrated, not tolerating oral intake or failed oral rehydration therapy
See Also
External Links
References
- ↑ Steiner, M. J. (2004) ‘Is This Child Dehydrated?’, JAMA, 291(22), p. 2746. doi: 10.1001/jama.291.22.2746
- ↑ Freedman SB, Willan AR, Boutis K, Schuh S. Effect of Dilute Apple Juice and Preferred Fluids vs Electrolyte Maintenance Solution on Treatment Failure Among Children With Mild Gastroenteritis: A Randomized Clinical Trial. JAMA. 2016 May 10;315(18):1966-74. doi: 10.1001/jama.2016.5352. PMID: 27131100. https://pubmed.ncbi.nlm.nih.gov/27131100/
- ↑ SGEM#158: Tempted by the Fruit of Another – Dilute Apple Juice for Pediatric Dehydration https://www.thesgem.com/2016/06/sgem158-tempted-by-the-fruit-of-another-dilute-apple-juice-for-pediatric-dehydration/