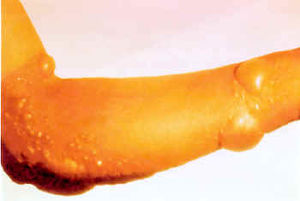
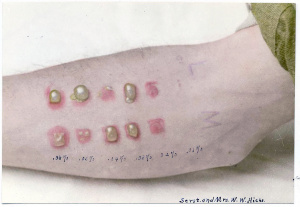
Blister chemical agents
Background

WWII Lewisite poster

Dropping of white phosphorus bomb.
- Highly persistent
- Skin primary route of exposure when in liquid form; pulmonary and GI tracts as routes in vapor form
Types
- Lewisite (L)
- Sulfur mustard (H)
- Phosgene oxime (CX)
Pathophysiology
- Alkylation of DNA, RNA, and protein causing cell death
- Depletes glutathione causing cellular membrane breakdown
Clinical Features
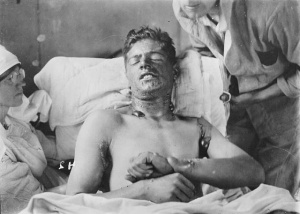
Chemical burn caused by exposure to mustard gas (World War I).
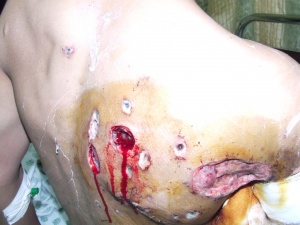
White phosphorus injuries
- Skin – Initially pruritus and stinging pain, superficial bullae appear over 24 hours. Blisters do not contain toxin
- GI – abdominal pain, nausea, vomiting, diarrhea, and weight loss
- Respiratory –
- Usually only upper respiratory tract affected
- Sinus congestion, sore throat, hoarseness. Rarely pulmonary edema
- Epithelial sloughing and pseudomembranes causing inability to clear pathogens and dead tissue.
- Mucous membranes and actively reproducing cells most vulnerable to severe damage
- Ocular damage – occurs within 4-8 hours
- conjunctivitis, chemosis, blepharospasm, and corneal perforation at even low level exposures
- Bone Marrow – Leukopenia first (3-5 days), followed by anemia and thrombocytopenia
Differential Diagnosis
Chemical weapons
- Blister chemical agents (Vesicants)
- Lewisite (L)
- Sulfur mustard (H)
- Phosgene oxime (CX)
- Pulmonary chemical agents (Choking agents)
- Incendiary agents
- Cyanide chemical weapon agents (Blood agents)
- Prussic acid (AKA hydrogen cyanide, hydrocyanic acid, or formonitrile)
- Nerve Agents (organophosphates)
- Acetylcholinesterase inhibitors
- Household and commercial pesticides (diazinon and parathion)
- G-series (sarin, tabun, soman)
- V-series (VX)
- Lacrimating or riot-control agents
- Pepper spray
- Chloroacetophenone
- CS
Evaluation
Management
- Immediate decontamination, 0.5% hypochlorite solution will inactivate sulfur mustard but not appropriate for pediatric patients
- Supportive care, ABCs
- Thermal burn-type care
- Fluid losses less than with thermal burns
- No antidotes for mustard agents
- N-acetylcysteine, glutathione
- G-CSF for patients with bone marrow suppression
- British antilewisite (BAL) – chelating agent to reduce systemic effects from lewisite exposure.
- Won’t alter the blistering effects on skin or airway.
- Only used for patients with shock or severe pulmonary injury given BAL side effect
- Relative contraindications to BAL: Renal disease, pregnancy