Arrhythmogenic right ventricular dysplasia
Background
- Second most common cause of sudden cardiac death in young patients [1]
- Up to 20% of sudden cardiac deaths in young people
- Usually occurs in people of Greek or Italian descent
- Male:Female = 3:1
- 1:1000-10,000 in the US
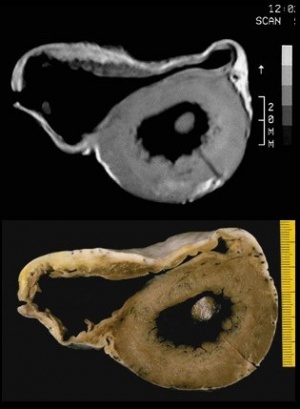
- Fibro-fatty replacement of right ventricular myocardium
- Two forms:
- Autosomal dominant
- Variable penetrance
- Autosomal recessive
- Naxos disease (Palmoplantar keratoderma) [2]
- Autosomal dominant
Clinical Features
- Palpitations (27%)
- Syncope (26%)
- Ventricular dysrhythmias/cardiac arrest (23%)
- Especially occurring during exercise
- Family history of unexplained syncope or sudden death
- Dysrhythmias refractory to antidysrhythmic meds
- Asymptomatic (40%)
- Usually these patients are identified through genetic testing of an affected or symptomatic family member
- Right ventricular failure (6%)
- Dilated cardiomyopathy
- Dyspnea
- Atypical chest pain (6%)
Differential Diagnosis
Cardiomyopathy
- Dilated cardiomyopathy
- Hypertrophic cardiomyopathy
- Restrictive cardiomyopathy
- Peripartum cardiomyopathy
- Takotsubo cardiomyopathy
- Arrhythmogenic right ventricular dysplasia
Syncope Causes
- Cardiovascular-mediated syncope
- Dysrhythmias:
- Cardiovascular disease
- Neurally mediated syncope
- Vasovagal:
- Fear, pain, emotion, valsalva, breath-holding spell
- Situational (associated with):
- Vasovagal:
- Orthostatic hypotension-mediated syncope:
- Volume depletion:
- Autonomic Dysreflexia
- Autonomic failure due to meds
- Other serious causes
- Stroke
- SAH
- TIA
- Vertebrobasilar Insufficiency
- Subclavian steal
- Heat syncope
- Hypoglycemia
- Hyperventilation
- Asphyxiation
- Seizure
- Narcolepsy
- Psychogenic (anxiety, conversion disorder, somatic symptom disorder)
- Toxic (drugs, carbon monoxide, etc.)
T Wave Inversions
- Normal in pediatrics
- Myocardial infarct (NSTEMI)
- Myocardial ischemia (Wellen's) - T waves go up, then down
- Hypokalemia - T waves go down, then up (or camel humped, one upright TW and upright U-wave in severe hypokalemia)
- Hyperkalemia
- Pulmonary embolism (RV strain)
- Pulmonary hypertension, acute or chronic
- Pulmonary disease - hyperventilation, pneumothorax, pneumonia
- LVH with strain pattern
- RVH
- Bundle branch block (both left and right)
- WPW
- Pericarditis (stage 3)
- CNS T waves (diffuse, deep)
- Arrhythmogenic right ventricular dysplasia (may also have epsilon wave)
- HOCM
- Paced rhythm
- Elevated intracranial pressure
Evaluation
ECG
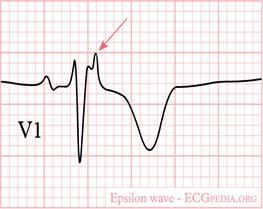
- Epsilon wave
- Seen in 30-50% of cases
- Most specific finding
- Small positive deflection at the end of the QRS complex
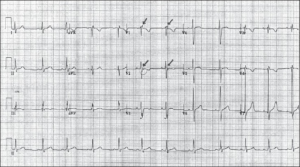
- V1-V3 T wave inversions
- Seen in 85% of cases
- Especially in patients >14 yrs old)
- Localised QRS widening
- 110 ms in V1-V3
- Sudden VT episodes with LBBB morphology
- Prolonged S-wave upstroke
- 55 ms in V1-3
- Seen in 95% of cases
Imaging
Major and minor criteria rely on echo and cardiac MRI
- Echocardiography
- Hypokinetic and dilated right ventricle
- Dilation of RVOT
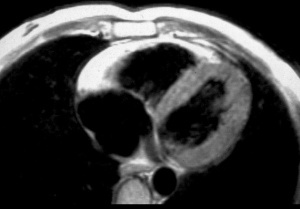
- Cardiac MRI [3]
- Fibro-fatty infiltration
- Thinning of right ventricular myocardium
- RV aneurysm
- RV dilatation
- Regional wall motion abnormalities
- Global systolic dysfunction
- Histological studies provide post-mortem diagnosis
- May prompt testing in family members
Management
- Beta blockers or amiodarone to suppress ventricular dysrhythmias
- Sotalol is preferred
- ICD implantation if high-risk features
- Ablation of conduction pathways
- Treat heart failure with diuretics, ACE inhibitors
- Heart transplant
Disposition
- Admission under cardiology if symptomatic
- Admission under cardiology if high-risk features[4]:
- Syncope due to cardiac arrest
- Recurrent dysrhythmias not suppressed by drug therapy
- Cardiac arrest in first-degree relative
- Incidental finding: Cardiology follow-up for further risk assessment and possible ICD placement or ablation
See Also
References
- ↑ https://litfl.com/arrhythmogenic-right-ventricular-cardiomyopathy-arvc/
- ↑ Protonotarios, N., and Tsatsopoulou, A. (2006). Naxos disease: Cardiocutaneous syndrome due to cell adhesion defect. Orphanet Journal of Rare Diseases, 1(4).
- ↑ https://litfl.com/arrhythmogenic-right-ventricular-cardiomyopathy-arvc/
- ↑ https://litfl.com/arrhythmogenic-right-ventricular-cardiomyopathy-arvc/
- Anderson EL. Arrhythmogenic right ventricular dysplasia. Am Fam Physician. 2006 Apr 15;73(8):1391-8.
- Perez Diez D, Brugada J. Diagnosis and Management of Arrhythmogenic Right Ventricular Dysplasia. E-Journal of the ESC Council for Cardiology Practice, European Society of Cardiology 2008.