Background
- Abbreviation: TIA
- New Definition: a brief episode of neurologic dysfunction caused by focal brain, spinal cord or retinal ischemia, with clinical symptoms typically lasting less than one hour, and without evidence of acute infarction. [1]
- Should be viewed as analogous to unstable angina
- Classic Definition: A sudden, focal neurologic deficit that lasts for less than 24 hours, is presumed to be of vascular origin, and is confined to an area of the brain or eye perfused by a specific artery[1]
- Since 15% of strokes are preceded by TIA, timely eval of high risk conditions like Atrial Fibrillation and Carotid Stenosis is important
Clinical Features
Differential Diagnosis
Evaluation
- Labs
- POC glucose
- CBC
- Chemistry
- Coags
- Troponin
- T&S
- ECG
- In large ICH or stroke, may see deep TWI and prolong QT, occ ST changes
- Head CT (non-contrast)
- In ischemia stroke CT has sensitivity 42%, specificity 91%[2]
- In acute ICH the sensitivity is 95-100%[3]
- The goal of CTH is to identify stroke mimics (ICH, mass lesions, etc .)[4]
- Also consider:
- CTA brain and neck
- To check for large vessel occlusion for potential thrombectomy
- Determine if there is carotid stenosis that warrants endarterectomy urgently
- Pregnancy test
- CXR (if infection suspected)
- UA (if infection suspected)
- Utox (if ingestion suspected)
MR Imaging (for Rule-Out CVA or TIA)
- MRI Brain with DWI, ADC (without contrast) AND
- Cervical vascular imaging (ACEP Level B in patients with high short-term risk for stroke):[5]
- MRA brain (without contrast) AND
- MRA neck (without contrast)
- May instead use Carotid CTA or US (Carotid US slightly less sensitive than MRA)[6] (ACEP Level C)
Management
- Little acute management (given normally resolution of symptoms)
- Consider Aspirin 325 mg PO (once hemorrhage ruled-out) for low risk TIA (ABCD2 score < 4)
- Consider dual antiplatelet therapy for high risk TIA (ABCD2 score ≥ 4)[7]
- Load with Aspirin 325 mg chewed, followed by ASA 81 mg PO daily
- Load with Clopidogrel 300 mg PO followed by 75 mg daily for 3 weeks only
Medication Dosing
Aspirin 325mg chewed, then 81mg PO daily PO
Clopidogrel 300mg PO load, then 75mg daily x 3 weeks PO"Clopidogrel Dual antiplatelet for high-risk TIA (ABCD2 >" contains a listed ">" character as part of the property label and has therefore been classified as invalid.
Disposition
ACEP Guidelines[5]
- Level B: In adult patients with suspected TIA, do not rely on current existing risk stratification instruments (eg, age, blood pressure, clinical features, duration of TIA and presence of diabetes [ABCD2] score) to identify TIA patients who can be safely discharged from the ED.
- In contrast to the 2009 AHA/ASA recommendations that were based on limited research, the ABCD2 does not sufficiently identify the short-term risk for stroke to use alone as a risk-stratification instrument.
- Multiple other risk-stratification instruments have been evaluated less frequently than the ABCD2 score. None have demonstrated the ability to identify individual patients at sufficiently low short-term risk for stroke to use alone as a risk-stratification instrument.
- Level B: A rapid ED based diagnostic protocol can be used to safely identify patients at short-term risk for stroke.
- Study based on observation units and outpatient TIA clinics[8]
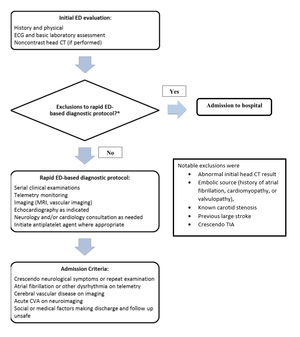
Example of a rapid ED protocol for TIA
Prognosis
Canadian TIA Score
- The score offers better performance than ABCD2 in predicting stroke risk after TIA, particularly low risk. [9]
Item Scoring
- Clinical Findings:
- 1. First TIA (in lifetime) (2 pt)
- 2. Symptoms ≥10 minutes (2 pt)
- 3. Past history of carotid stenosis (2 pt)
- 4. Already on antiplatelet therapy (3 pt)
- 5. History of gait disturbance (1 pt)
- 6. History of unilateral weakness (1 pt)
- 7. History of vertigo (-3 pts)
- 8. Initial triage diastolic blood pressure ≥110 mm Hg (3 pt)
- 9. Dysarthria or aphasia (history or examination) (3 pt)
- Investigations in the emergency department:
- 1.Atrial fibrillation on electrocardiogram (2 pt)
- 2.Infarction (new or old) on computed tomography (1 pt)
- 3.Platelet count≥400×109/L (2 pt)
- 4.Glucose ≥15 mmol/L (3pt)
| Points
|
Stroke Risk
|
Risk of Stroke or Carotid Revascularization in 7 Days
|
| -3-3
|
Low
|
.5%
|
| 4-8
|
Medium Risk
|
2.3%
|
| ≥9
|
High
|
5.9%
|
ABCD2 Score[10]
- Risk of stroke at 2d, 7d, and 90d from TIA
- Although prognostic, evidence-based admission thresholds have not been determined
- None with score <3 had CVA within one week in study
- Studies have failed to validate the ABCD2 score, and may cause physicians to incorrectly classify ~8% of patients as low risk, with sensitivity of the score for high risk patients only ~30%[11][12]
Scoring
- Age >60yr (1 pt)
- BP (SBP >140 OR diastolic >90) (1 pt)
- Clinical Features
- Isolated speech disturbance (1 pt)
- Unilateral weakness (2 pts)
- Duration of symptoms
- 10-59 min (1 pt)
- >60 min (2 pts)
- Diabetes mellitus (1 pt)
| Points
|
Stroke Risk
|
Two Days
|
Seven Days
|
90 Days
|
| 0-3
|
Low
|
1.0%
|
1.2%
|
3.1%
|
| 4-5
|
Moderate
|
4.1%
|
5.9%
|
9.8%
|
| 6-7
|
High
|
8.1%
|
11.7%
|
17.8%
|
- According to the 2018 Canadian Heart and Stroke Guideline, the Clinical component of the ABCD2 score is the most important prognostic feature[13]
- Very high risk for recurrent stroke are the following symptoms that have occurred within the last 48 hours
- Transient, fluctuating or persistent unilateral weakness (face, arm and/or leg)
- Transient, fluctuating or persistent language/speech disturbance
- And/or fluctuating or persistent symptoms without motor weakness or language/speech disturbance
Calculators
ABCD2 Score for TIA
ABCD2 Score — TIA Stroke Risk
| Criteria
|
Select
|
| A — Age
|
1 <60 years (0) ≥60 years (+1)
|
| B — Blood Pressure
|
1 SBP <140 and DBP <90 (0) SBP ≥140 or DBP ≥90 (+1)
|
| C — Clinical Features
|
1 Other symptoms (0) Speech disturbance without weakness (+1) Unilateral weakness (+2)
|
| D — Duration of symptoms
|
1 <10 minutes (0) 10–59 minutes (+1) ≥60 minutes (+2)
|
| D — Diabetes
|
1 No (0) Yes (+1)
|
| ABCD2 Score
|
/ 7
|
| Interpretation — 2-Day Stroke Risk After TIA
|
| 0–3
|
Low risk — 1.0% risk of stroke within 2 days.
|
| 4–5
|
Moderate risk — 4.1% risk. Consider urgent workup and admission.
|
| 6–7
|
High risk — 8.1% risk. Admit for urgent evaluation and treatment.
|
| References
|
- Johnston SC, Rothwell PM, Nguyen-Huynh MN, et al. Validation and refinement of scores to predict very early stroke risk after transient ischaemic attack. Lancet. 2007;369(9558):283-292. PMID 17258668.
|
External Links
See Also
References
- ↑ 1.0 1.1 Albers GW, et al. The TIA Working Group. Transient ischemic attack: proposal for a new definition. N Engl J Med. 2002; 347:1713–1716.
- ↑ Mullins ME, Schaefer PW, Sorensen AG, Halpern EF, Ay H, He J, Koroshetz WJ, Gonzalez RG. CT and conventional and diffusion-weighted MR imaging in acute stroke: study in 691 patients at presentation to the emergency department. Radiology. 2002 Aug;224(2):353-60.
- ↑ Suarez JI, Tarr RW, Selman WR. Aneurysmal subarachnoid hemorrhage. N Engl J Med. 2006; 354(4):387–396.
- ↑ Douglas VC, Johnston CM, Elkins J, et al. Head computed tomography findings predict short-term stroke risk after transient ischemic attack. Stroke. 2003;34:2894-2899.
- ↑ 5.0 5.1 ACEP Clinical Policy: Suspected Transient Ischemic Attack full text
- ↑ Nederkoorn PJ, Mali WP, Eikelboom BC, et al. Preoperative diagnosis of carotid artery stenosis. Accuracy of noninvasive testing. Stroke. 2002;33:2003-2008.
- ↑ Johnston SC, Easton JD, Farrant M, Barsan W, Conwit RA, Elm JJ, Kim AS, Lindblad AS, Palesch YY. Clopidogrel and Aspirin in Acute Ischemic Stroke and High-Risk TIA. N Engl J Med. 2018 Jul 19;379(3):215-225.
- ↑ Ross MA, Compton S, Medado P, et al. An emergency department diagnostic protocol for patients with transient ischemic attack: a randomized controlled trial. Ann Emerg Med. 2007;50:109-119
- ↑ Perry JJ et al. Prospective validation of Canadian TIA Score and comparison with ABCD2 and ABCD2i for subsequent stroke risk after transient ischaemic attack: multicentre prospective cohort study.BMJ 2021 Feb 4.
- ↑ Johnston SC, et al. Validation and refinement of scores to predict very early stroke risk after transient ischaemic attack.Lancet. 2007; 369(9558):283-92.
- ↑ Stead LG, Suravaram S. An assessment of the incremental value of the ABCD2 score in the emergency department evaluation of transient ischemic attack. Ann Emerg Med. 2011 Jan;57(1):46-51.
- ↑ Ghia D, Thomas P. Low positive predictive value of the ABCD2 score in emergency department transient ischaemic attack diagnoses: the South Western Sydney transient ischaemic attack study. Intern Med J. 2012 Aug;42(8):913-8.
- ↑ Boulanger JM, Lindsay MP, Gubitz G, et al. Canadian Stroke Best Practice Recommendations for Acute Stroke Management: Prehospital, Emergency Department, and Acute Inpatient Stroke Care, 6th Edition, Update 2018. Int J Stroke. 2018;:1747493018786616.



