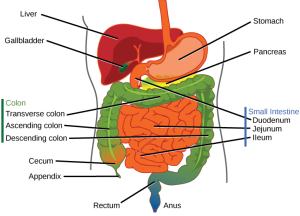
Undifferentiated lower gastrointestinal bleeding
(Redirected from Lower GI Bleeding)
Background
- Loss of blood from the GI tract distal to the ligament of Treitz
- Diverticulosis cause majority; other conditions include colitis, angiodysplasia, polyps, colorectal cancer, hemorrhoids, anal fissures, inflammatory bowel disease
- Majority of cases originate distally to ileocecal valve, rather than small intestines[1]
- Consider recent procedures such as abdominal surgeries or colonoscopies/polypectomies
- Must consider upper GI bleed (especially rapid transit) as a source, as a significant number of lower GI bleeds have a concurrent upper GI bleed, brisk or not[2]
- 80% of lower GI bleeding will resolve spontaneously[3]
Medication Risk Factors
- Obtain a thorough medication history to assess for new antiplatelets or anticoagulants
Clinical Features
Type of blood
- Hematochezia
- Usually represents lower GI bleeding
- Left colonic bleeding tends to be bright red, whereas right colonic is usually maroon and mixed with stool[4]
- May represent upper GI source if bleeding is brisk; usually accompanied by hematemesis and hemodynamic instability
- Melena
- Usually represents bleeding from upper GI source (see upper GI bleed)
- May represent slow bleeding or slow stool transit from lower GI source
Differential Diagnosis
Undifferentiated lower gastrointestinal bleeding
- Upper GI Bleeding
- Diverticular disease
- Vascular ectasia / angiodysplasia
- Inflammatory bowel disease
- Infectious colitis
- Mesenteric Ischemia / ischemic colitis
- Meckel's diverticulum
- Colorectal cancer / polyps
- Hemorrhoids
- Aortoenteric fistula
- Nearly 100% mortality if untreated
- Consider in patients with gastrointestinal bleeding and known abdominal aortic aneurysms or aortic grafts
- Rectal foreign body
- Rectal ulcer (HIV, Syphilis, STI)
- Anal fissure
Evaluation
- Digital rectal exam for guaiac or assessment of anorectal structural abnormalities
- Note that guaiac tests have low sensitivity, many false positive etiologies (red meat, red jello, certain fruits/veggies, iron), and may not change management clinically
- Consider chart review to search for prior colonoscopy/endoscopy results
Workup
- CBC
- Consider q3-12hr serial Hgb, depending on suspected severity of bleed
- Initial Hgb may be normal if bleeding is acute
- CMP
- BUN may be elevated if bleeding occurs from site high in GI tract, due to heme digestion to nitrogenous substances reflected in BUN[5]
- Coags
- Type and screen/cross
- Consider:
Definitive studies
- Consider:
- Anoscopy if source of bleeding cannot be identified on external exam
- Proctoscopy (22cm from anal verge)
- Sigmoidoscopy (60cm from anal verge)
Management
- NPO, if there is foreseeable endoscopy or surgery
- Fluid resuscitation for all
- Consider transfusing pRBCs/platelets for unstable patients or with very low hemoglobin (<7). with cardiovascular disease use trigger of 8 and target of 10 hemoglobin.
- Base decision to transfuse on individual clinical factors. Active bleeding and tachycardia may call for transfusion despite a normal Hgb
Categorize as stable versus unstable using shock index: <1 stable; >1 unstable or suspect active bleeding
- Unstable
- CT angiography is preferred for hemodynamically unstable patients due to speed[7]
- Positive CTA demonstrating extravasation/blush calls for IR consult for transcatheter arteriography and subsequent embolization.
- Consult GI for emergent colonoscopy, as it is the diagnostic/therapeutic procedure of choice (within 12-24 hours); upper endoscopy may be needed if CTA does not reveal source of GI bleeding
- Patients with a positive CTA are more likely to have a source found on subsequent colonoscopy
- Consult surgery if endoscopy and IR embolization fail or are not available
- CT angiography is preferred for hemodynamically unstable patients due to speed[7]
- Stable
- See "Disposition"
Major Bleed and Existing Coagulopathy
- Correct coagulopathy
- PCC (preferred) or FFP for patients on warfarin
- Vitamin K 10mg IV (best bioavailability in critical patients)
- Consider targeted reversal agents for DOACs in life-threatening LGIB refractory to initial resuscitation treatments, if the DOAC was taken in the past 24 hours: See Anticoagulant reversal for life-threatening bleeds
- Platelets should be administered to thrombocytopenic patients to a goal of 30-50, depending if endoscopy is planned[8]
- ACG recommends against Tranexamic acid as it has no evidence for benefit but may increase VTE
Special situations
- Marathon runners - 16% will have hematochezia within 24-48 hrs of race and 85% will be guaiac positive[9]
- Non-actionable unless abdominal pain present
Medication Dosing
Vitamin K 10mg IV
Disposition
Discharge
- Oakland score can help determine if outpatient management is feasible; a score of <8 can be considered for safe discharge[10]
- Based on a recent meta-analysis, the Oakland score, compared to other LGIB risk scores, has good performance in predicting safe discharge, major bleeding, and need for transfusion[11]
- Bleeding from hemorrhoids, anal fissures, or known IBD (hemodynamically stable)
- Minor, self-terminating bleed with no other indication for admission (shock index >1; low risk score calculated)
Admission
- Melena
- Significant anemia
- Hemodynamic instability
- Identified as high risk based on Oakland score
See Also
Gastrointestinal Bleeding Pages
- Adults
- Pediatrics
References
- ↑ Farrell JJ, Friedman LS. Review article: the management of lower gastrointestinal bleeding. Aliment Pharmacol Ther. 2005 Jun 1;21(11):1281-98. doi: 10.1111/j.1365-2036.2005.02485.x. PMID: 15932359.
- ↑ Amin SK, Antunes C. Lower Gastrointestinal Bleeding. [Updated 2023 Jul 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448126
- ↑ Farrell JJ, Friedman LS. Review article: the management of lower gastrointestinal bleeding. Aliment Pharmacol Ther. 2005 Jun 1;21(11):1281-98. doi: 10.1111/j.1365-2036.2005.02485.x. PMID: 15932359.
- ↑ Frost J, Sheldon F, Kurup A, Disney BR, Latif S, Ishaq S. An approach to acute lower gastrointestinal bleeding. Frontline Gastroenterol. 2017 Jul;8(3):174-182. doi: 10.1136/flgastro-2015-100606. Epub 2015 Jun 29. PMID: 28839906; PMCID: PMC5558275.
- ↑ Patel, Sneha MD; Peraza, Jellyana MD; Hasani, Aliaskar MD; Luther, Sanjana MD; Chugh, Rishika MD; Tokayer, Aaron MD, FACG. 611 Finding the Ideal BUN to Creatinine Ratio in an Upper GI Bleed. The American Journal of Gastroenterology 114():p S355, October 2019. | DOI: 10.14309/01.ajg.0000591980.77707.20
- ↑ Serur A, Rhee R, Ramjist J. Current Nonoperative Therapeutic Interventions for Lower Gastrointestinal Hemorrhage. Clin Colon Rectal Surg. 2020 Jan;33(1):22-27. doi: 10.1055/s-0039-1695033. Epub 2019 Nov 11. PMID: 31915422; PMCID: PMC6946602.
- ↑ Oakland K, Chadwick G, East JE, et al. Diagnosis and management of acute lower gastrointestinal bleeding: guidelines from the British Society of Gastroenterology. Gut 2019;67:776-789.
- ↑ Sengupta, N., Feuerstein, J. D., Jairath, V., Shergill, A. K., Strate, L. L., Wong, R. J., & Wan, D. (2023). Management of Patients With Acute Lower Gastrointestinal Bleeding: An Updated ACG Guideline. The American journal of gastroenterology, 118(2), 208–231. https://doi.org/10.14309/ajg.0000000000002130
- ↑ Sullivan SN, Wong C. Runners' diarrhea. Different patterns and associated factors. J Clin Gastroenterol 1992;14:101-104.
- ↑ Oakland K, Jairath V, Uberoi R, Guy R, Ayaru L, Mortensen N, Murphy MF, Collins GS. Derivation and validation of a novel risk score for safe discharge after acute lower gastrointestinal bleeding: a modelling study. Lancet Gastroenterol Hepatol. 2017 Sep;2(9):635-643. doi: 10.1016/S2468-1253(17)30150-4. Epub 2017 Jun 23. PMID: 28651935.
- ↑ Almaghrabi M, Gandhi M, Guizzetti L, et al. Comparison of Risk Scores for Lower Gastrointestinal Bleeding: A Systematic Review and Meta-analysis. JAMA Netw Open. 2022;5(5):e2214253. doi:10.1001/jamanetworkopen.2022.14253