Syphilis
Background
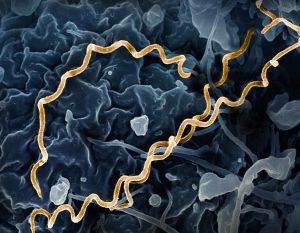
- Syphilis is caused by the spirochete Treponema pallidum. [1]
- Usually sexually transmitted
- Causes a wide range of systemic manifestations that are characterized by episodes of active disease interrupted by periods of latency
- Approximately 30% of asymptomatic contacts examined within 30 days of exposure have infection
Pathogenesis
- Spirochetes penetrate intact mucous membranes or microscopic dermal abrasions.
- Transmission through sexual contact with infectious lesions, infection in utero, blood transfusion, and organ transplantation[2]
- Blood from a patient with incubating or early syphilis is infectious.
- Characterized by multiple stages separated by periods of latency: primary, secondary, latent and tertiary
Clinical Features
Primary Syphilis
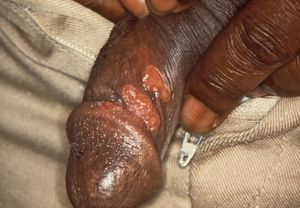
- Primary lesion appears after an incubation of 2-6 weeks
- Single painless papule that becomes eroded and indurated, cartilaginous consistency on palpation
- Minority of patients can have multiple lesions or atypical appearance
- Occurs at point of contact: penis, rectum, mouth, external genitalia, cervix, or labia
- Heals in 4-6 weeks
- Regional lymphadenopathy that is painless and firm
Secondary Syphilis
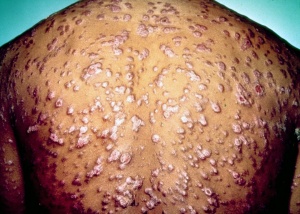
- Characterized by generalized mucocutaneous lesions and lymphadenopathy but can also be found in other tissues[3]
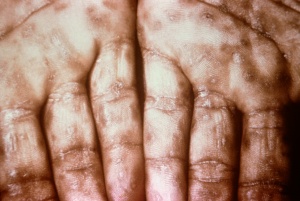
- Skin lesions are usually maculopapular, pale red or pink, non-pruritic, discrete, and distributed on the trunk and proximal extremities. They may be subtle.
- They progress to more wide spread papular lesions that frequently involve the palms and soles.
- Appears 6-8 weeks after the chancre heals and subsides within 2-6 weeks
- Healing chancre may still be present in ~15% of cases. The stages may overlap more frequently in HIV patients. [4]
- In intertriginous areas, papules can enlarge to produce broad, moist, pink or gray-white infectious lesions called condylomata lata
- CSF abnormalities are detected in as many as 40% during this stage. CNS involvement can be symptomatic or asymptomatic.
- Constitutional symptoms may accompany or precede secondary syphilis. Can include: sore throat, fever, weight loss, malaise, anorexia, headache, and meningismus
- Less common complications include: hepatitis, nephropathy, gastritis, proctitis, rectosigmoid mass, arthritis, periositis, optic neuritis, iritis, uveitis, pupillary abnormalities
Latent Syphilis
- Detectable by serologic testing only (FTA-ABS and TP-PA)
- May intermittently be present in the bloodstream and transmitted through blood transfusion or organ donation
- Spontaneous cure is rare
- Non-treponemal tests may be negative in 30% of latent cases. Therefore in suspected cases a TP-PA test is used in addition to CSF (CSF-VRDL and FTA-ABS)sampling for neurosyphilis diagnosis.[5]
Tertiary Syphilis
- Characterized by progressively destructive mucocutaneous, musculoskeletal, or parenchymal lesions, aortitis or CNS manifestations
- The most common manifestation in the US today is neurosyphilis in HIV infected persons.
- Historical manifestations:
- Gumma: granulomatous lesion
- Cardiovascular syphilis: involves the vasa vasorum of the ascending aorta and can result in aneurysm formation
- Late symptomatic neurosyphilis: tabes dorsalis and paresis
- Ocular syphilis should be considered equivalent to neurosyphilis[6]
System Specific
CNS
- CSF-VDRL preferred test[7]
- Continuum of involvement from asymptomatic patient with CSF abnormalities to meningitis and focal neurologic deficits
- RPR titers of ≥ 1:32 are at higher risk of having neurosyphilis, even higher if HIV infected.
- Demonstrable in up to 25% of patients with latent infection and up to 40% of primary or secondary cases [8]
- Patients with early syphilis who have CSF findings may need to be treated as with neurosyphilis, especially in the setting of HIV
- Meningeal: Headache, nausea/vomiting, neck stiffness, cranial nerve involvement, seizures, changes in mental status, uveitis, iritis or hearing loss
- Meningovascular: Meningitis together with inflammatory vasculitis leading to stroke syndrome
- Parenchymal: Paresis, hyperactive reflexes, Argyll Robertson pupils, illusions/delusions/hallucinations, memory defects, speech changes.
- Argyll Robertson pupil: small, irregular pupil that reacts to accommodation but not to light
- Tabes dorsalis presents with a wide based gait ataxia, foot drop, paresthesias, bladder dysfunction, impotence, areflexia, loss of positional, deep pain and temperature sensations• Cardiovascular
Cardiovascular
- 10-40 years after infection
- Endarteritis obliterans of the vasa vasorum leads
- Aortitis, aortic regurgitation, saccular aneurysm (usually ascending), coronary ostial stenosis
Gumma
- Commonly involves skin and skeletal system
- Solitary lesions ranging from microscopic to several centimeters
- Granulomatous inflammation with central area of necrosis due to endarteritis obliterans
- Painless, indurate nodular or ulcerative lesions
Congenital Syphilis
- Transmission across the placenta may occur at any stage of pregnancy[9]
- Treatment before the 16th week of pregnancy should prevent fetal damage
- Treatment before the third trimester should treat the infected fetus
- Most common clinical problem is a healthy-appearing baby with a positive serologic test
Differential Diagnosis
- Ulcerative STDs
- Proctitis
- Genital Herpes
- Chancroid
- Behçet's disease
- Lymphogranuloma Venereum
- Gonorrhea
- Candidiasis
- Chlamydia
- Granuloma Inguinale
- HIV
- Bacteremia
- Aortic Insufficiency
- Dementia
- Diabetic Retinopathy
- Sepsis
- Alopecia
- Tuberculosis
- Immunodeficiency
- Rocky Mountain Spotted Fever
- Myocarditis
- Measles
- Rubella
- Meningitis
- Tularemia
- Lyme Disease
Sexually transmitted diseases
- Chancroid
- Chlamydia trachomatis
- Granuloma inguinale
- Hepatitis B
- Herpes Simplex Virus-2
- HIV
- Human papillomavirus
- Lymphogranuloma venereum
- Neisseria gonorrhoeae
- Trichomonas
- Syphilis
Evaluation
Nontreponemal Tests:[10]
VDRL and RPR may be falsely negative for up to four weeks after the appearance of a chancre and cannot reliably rule out primary syphilis. Both are only 70-80% sensitive.
- Rapid Plamsa Reagin (RPR)*
- Faster and easier to perform
- Venereal Disease Research Laboratory (VDRL)*
- Standard for CSF examination
- Toludine Red Unheated Serum Test (TRUST)
Most commonly in the ED, the VDRL and RPR will be the ordered screening test
Treponemal Test:[10]
- Fluorescent treponemal antibody absorption (FTA-ABS)
- Microhemagglutination test for antibodies to Treponema pallidum (MHA-TP)
- Treponemal pallidum particle agglutination assay (TP-PA)
- Treponema pallidum enzyme immunoassay (TP-EIA)
- Pleocytosis (>5 WBC/uL), increased protein (>45mg/dL) or VDRL reactivity
- May be confounded by HIV infection[11]
- CSF VDRL test is highly specific but is relatively insensitive. Further testing with treponemal antibodies may be necessary.
HIV-infected patients
- All newly diagnosed HIV patients should be tested for syphilis and vice versa
- RPR titer and CD4 count can be used to identify patients at higher risk for neurosyphilis for lumbar puncture
RPR and TPPA testing
- Syphilis total antibodies can persist for many years. A positive result does not necessarily indicate active disease. In patients with positive syphilis total antibodies, the RPR provides information on active versus past infection.
- For assessing treatment efficacy in patients who have been treated for syphilis, "Syphilis Treatment Follow-up (RPR with Titer)"should be ordered. Successful treatment is generally indicated by a 4-fold reduction in RPR titer (e.g., 1:32 to 1:8).
| Total antibodies | RPR | TPPA | Interpretation |
|---|---|---|---|
| negative | not done | not done | infection unlikely |
| positive | positive | not done | recent infection likely |
| positive | negative | positive | past or present infection |
| positive | negative | negative | false positive syphilis antibodies |
Management
Treatment is primary with penicillin with dosing and type of penicillin determined by the stage of disease[12]
Treat those exposed within the past 3 months.
Early Stage
This is classified as primary, secondary, and early latent syphilis less than one year.
Treatment Options:
- Penicillin G Benzathine 2.4 million units IM x 1
- Repeat dose after 7 days for pregnant patients and HIV infection
- Doxycycline 100mg oral twice daily for 14 days as alternative
Congenital Syphilis:
- Penicillin G 50,000 units/kg IV q4-6h x 10-14 days
- Penicillin G Procaine 50,000 units/kg IM daily x 10-14 days
- Penicillin G Benzathine 50,000 units/kg IM x 1
Older Children:
- Penicillin G Benzathine 50,000 units/kg IM x 1 (max 2.4 million units)
Late Stage
Late stage is greater than one year duration, presence of gummas, or cardiovascular disease
Treatment Options:
- Penicillin G Benzathine 2.4 million units IM weekly x 3 weeks
- Doxycycline 100mg oral twice daily for 4 weeks as alternative
Neurosyphilis
There are 3 Major options with none showing greater efficacy than others:
- Penicillin G 3-4 million units IV every 4 hours x 10-14 days
- Penicillin G 24 million units continuous IV infusion x 10-14 days
- Penicillin G Procaine 2.4 million units IM daily + probenecid 500mg oral every 6 hours for 10-14 days.
- Alternative:
- Ceftriaxone 2gm IV once daily for 10-14 days
- Desensitization to the penicillin allergy is still the preferred method of treatment for patients with early and late stage disease (especially during pregnancy)
Pregnancy
- Penicillin, dosage depends on stage [13]
Jarisch-Herxheimer Reaction
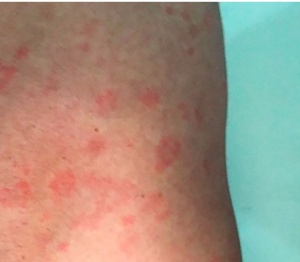
- Reaction to treatment consisting of fever, chills, myalgias, headache, tachycardia, increased respiratory rate, leukocytosis, vasodilation with mild hypotension
- Usually resolves within 12-24 hours
- Symptom based treatment
Disposition
- Primary and late stage syphilis can be discharge however close follow up should be provided for each with primary care provider or health department
- Neurosyphilis should be admitted
See Also
References
- ↑ Lukehart SA. Chapter 169. Syphilis. In: Longo DL, Fauci AS, Kasper DL, Hauser SL, Jameson J, Loscalzo J. eds. Harrison's Principles of Internal Medicine, 18e.New York, NY: McGraw-Hill; 2012.
- ↑ Workowski KA, Berman S, Centers for Disease Control and Prevention (CDC). Sexually transmitted diseases treatment guidelines, 2010. MMWR Recomm Rep. 2010;59(RR-12):1–110.
- ↑ Chapel TA. The signs and symptoms of secondary syphilis. Sex Transm Dis. 1980;7(4):161–164.1.
- ↑ Chesson HW, Heffelfinger JD, Voigt RF, Collins D. Estimates of primary and secondary syphilis rates in persons with HIV in the United States, 2002. Sex Transm Dis 2005; 32:265.
- ↑ The laboratory diagnosis of syphilis. Can J Infect Dis Med Microbiol. 2005 Jan-Feb; 16(1): 45–51. PMID: 18159528
- ↑ Clinical Advisory: Ocular Syphilis in the United States https://www.cdc.gov/std/syphilis/clinicaladvisoryos2015.htm
- ↑ Marra CM, Tantalo LC, Maxwell CL, Ho EL, Sahi SK, Jones T. The rapid plasma reagin test cannot replace the venereal disease research laboratory test for neurosyphilis diagnosis. Sex Transm Dis. 2012 Jun;39(6):453-7.
- ↑ Lukehart SA. Chapter 169. Syphilis. In: Longo DL, Fauci AS, Kasper DL, Hauser SL, Jameson J, Loscalzo J. eds. Harrison's Principles of Internal Medicine, 18e.New York, NY: McGraw-Hill; 2012
- ↑ Rosenberg AA, Grover T. The Newborn Infant. In: Hay WW, Jr., Levin MJ, Deterding RR, Abzug MJ. eds. CURRENT Diagnosis & Treatment: Pediatrics, 22e.New York, NY: McGraw-Hill; 2013.
- ↑ 10.0 10.1 Larsen SA, Steiner BM, Rudolph AH. Laboratory diagnosis and interpretation of tests for syphilis. Clin. Microbiol. Rev. 1995;8(1):1–21.
- ↑ Ghanem KG1, Moore RD, Rompalo AM, Erbelding EJ, Zenilman JM, Gebo KA. Lumbar puncture in HIV-infected patients with syphilis and no neurologic symptoms. Clin. Infect Dis. 2009 Mar 15;48(6):816-21.
- ↑ Kaplan JE, Benson C, Holmes KH, et al. Guidelines for prevention and treatment of opportunistic infections in HIV-infected adults and adolescents: recommendations from CDC, the National Institutes of Health, and the HIV Medicine Association of the Infectious Diseases Society of America. MMWR Recomm Rep. 2009;58(RR-4):1–207
- ↑ Mackay G. Chapter 43. Sexually Transmitted Diseases & Pelvic Infections. In:DeCherney AH, Nathan L, Laufer N, Roman AS. eds. CURRENT Diagnosis & Treatment: Obstetrics & Gynecology, 11e. New York, NY: McGraw-Hill; 2013