Monoarticular arthritis
Background
- Monoarticular arthritis (monoarthritis) refers to inflammation of a single joint
- The critical EM question is: Is this septic arthritis?
- Septic arthritis is a joint emergency requiring urgent drainage — delay increases risk of joint destruction
- Other common causes include crystal arthropathy (gout, pseudogout) and traumatic hemarthrosis
- Arthrocentesis is the key diagnostic procedure and should be performed on any hot, swollen joint without clear alternative diagnosis
Clinical Features
History
- Onset (acute vs. subacute), joint involved, trauma history
- Prior episodes (recurrent suggests crystal disease)
- Fever, chills, constitutional symptoms
- Recent infection, skin break, surgery, or injection
- Sexual history (disseminated gonococcal infection)
- History of gout, pseudogout, or autoimmune disease
- Immunosuppression, IV drug use, prosthetic joint
Physical Exam
- Joint warmth, erythema, effusion, decreased range of motion
- Pain with passive range of motion (highly suggestive of intra-articular process)
- Overlying skin: cellulitis, track marks, surgical scars, tophi
- Assess for signs of systemic infection
- Examine other joints (polyarticular process may present initially as monoarticular)
Red Flags for Septic Arthritis
- Fever with acute monoarthritis
- Recent bacteremia, skin infection, or surgical procedure
- Prosthetic joint with new pain/swelling
- Immunosuppressed patient
- IV drug use
- Non-weight-bearing or unable to flex joint
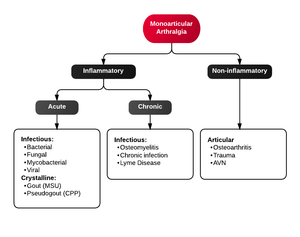
Differential Diagnosis
Monoarticular arthritis
- Acute osteoarthritis
- Avascular necrosis
- Crystal-induced (Gout, Pseudogout)
- Gonococcal arthritis, arthritis-dermatitis syndrome
- Nongonococcal septic arthritis
- Lyme disease
- Malignancy (metastases, osteochondroma, osteoid osteoma)
- Reactive poststreptococcal arthritis
- Trauma-induced arthritis
- Fracture
- Ligamentous injury
- Overuse
- Avascular necrosis
- Decompression sickness
- Spontaneous osteonecrosis
- Hemorrhagic (e.g. hemophilia, systemic anticoagulation
- Seronegative spondyloarthropathies (ankylosing spondylitis, IBD, psoriatic arthritis, reactive arthritis
- RA, SLE
- Sarcoidosis, amyloidosis
- Periarticular pathology
- Transient (Toxic) Synovitis (Hip)
- Slipped Capital Femoral Epiphysis (SCFE)
- Legg Calve Perthes Disease
Septic Arthritis
- Gonococcal arthritis
- Nongonococcal Arthritis
- Arthritis-Dermatitis Syndrome
Crystal-Induced Monoarthritis
Traumatic
- Fracture
- Ligamentous injury
- Overuse
Ischemic
- Avascular necrosis
- Decompression sickness
- Spontaneous osteonecrosis
- Pain in absence of trauma
- Femoral head, medial condyle of knee
Hemorrhagic
- Posttraumatic
- Hemophilia
- Systemic anticoagulation
Neoplastic
- Metastases
- Osteochondroma
- Osteoid osteoma
- Pigmented villonodular synovitis
Systemic Disease
- Remote infection, infectious endocarditis
- Rheumatic fever
- Seronegative (no RF) spondyloarthropathies (ankylosing spondylitis, IBD, psoriatic, reactive arthritis)
- Rheumatoid arthritis, SLE
Periarticular (Non-Articular)
Evaluation
Arthrocentesis (Key Diagnostic Study)
- Perform arthrocentesis on any acute hot, swollen joint unless clear alternative diagnosis
- Do not delay arthrocentesis for imaging
- Overlying cellulitis is a relative contraindication — consult orthopedics
Synovial Fluid Analysis
Arthrocentesis of synoval fluid
| Synovium | Normal | Noninflammatory | Inflammatory | Septic |
| Clarity | Transparent | Transparent | Cloudy | Cloudy |
| Color | Clear | Yellow | Yellow | Yellow |
| WBC | <200 | <200-2000 | 200-50,000 |
>1,100 (prosthetic joint) >25,000; LR=2.9 >50,000; LR=7.7 >100,000; LR=28 |
| PMN | <25% | <25% | >50% |
>64% (prosthetic joint) >90% |
| Culture | Neg | Neg | Neg | >50% positive |
| Lactate | <5.6 mmol/L | <5.6 mmol/L | <5.6 mmol/L | >5.6 mmol/L |
| LDH | <250 | <250 | <250 | >250 |
| Crystals | None | None | Multiple or none | None |
- Viscosity of synovial fluid may actually be decreased in inflammatory or infectious etiologies, as hyaluronic acid concentrations decrease
- The presence of crystals does not rule out septic arthritis; however, the diagnosis is highly unlikely with synovial WBC < 50,000[1]
- WBC >50,000/mm³ with >90% PMNs: highly suggestive of septic arthritis
- Crystals: negatively birefringent (gout), positively birefringent (pseudogout)
- Note: crystals and infection can coexist — always send culture even if crystals present
- Gram stain: positive in ~50% of non-gonococcal septic arthritis
- Culture: gold standard; also send blood cultures
Laboratory
- CBC with differential, ESR, CRP
- Blood cultures (positive in ~50% of septic arthritis)
- Uric acid (may be normal during acute gout flare)
- GC/CT NAAT if disseminated gonococcal infection suspected
Imaging
- X-ray of affected joint: chondrocalcinosis (pseudogout), fracture, joint destruction
- Ultrasound: confirm effusion, guide arthrocentesis
- MRI if osteomyelitis or periarticular abscess suspected
Management
Septic Arthritis
- Emergent orthopedic consultation for surgical drainage/washout
- Empiric IV antibiotics after arthrocentesis:
- Vancomycin (MRSA coverage) for most patients
- Add gram-negative coverage (ceftriaxone or cefepime) for immunocompromised, elderly, or IV drug users
- Ceftriaxone alone if gonococcal arthritis suspected
- Prosthetic joint infection: orthopedic consultation for operative management
Crystal Arthropathy
- Gout: NSAIDs (indomethacin, naproxen), colchicine, or corticosteroids (PO or intra-articular)
- Pseudogout: NSAIDs, colchicine, or intra-articular/systemic corticosteroids
- Avoid allopurinol initiation or changes during acute flare
Traumatic
- Splinting, pain management
- Orthopedic follow-up for hemarthrosis or fracture
Disposition
Admit
- Septic arthritis (for surgical drainage and IV antibiotics)
- Prosthetic joint infection
- Sepsis from joint source
- Unable to rule out septic arthritis with pending cultures in high-risk patient
Discharge
- Crystal arthropathy with adequate pain control
- Traumatic arthritis/hemarthrosis with orthopedic follow-up arranged
- Provide return precautions: fever, worsening pain/swelling, inability to bear weight
- Primary care or rheumatology follow-up for gout/pseudogout management
See Also
External Links
References
- ↑ Shah K, Spear J, Nathanson LA, Mccauley J, Edlow JA. Does the presence of crystal arthritis rule out septic arthritis?. J Emerg Med. 2007;32(1):23-6.