Arthrocentesis
Indications
General arthrocentesis indications
- Suspicion of septic arthritis
- Suspicion of crystal induced arthritis
- Evaluation of therapeutic response for septic arthritis
- Unexplained arthritis with synovial effusion
- Evaluation of joint capsule integrity if overlying laceration
- Relative: therapeutic (decrease intra-articular pressure, injection of anesthetics/steroids)
Contraindications
General arthrocentesis contraindications
- No absolute contraindications for diagnostic arthrocentesis
- Do not inject steroids into a joint that you suspect is already infected
- Relative Contraindications:
- Overlying cellulitis
- Coagulopathy
- Joint prosthesis (refer to ortho)
Equipment Needed
General arthrocentesis equipment
- Betadine or Chlorhexadine
- Sterile gloves/drape
- Sterile gauze
- Lidocaine
- Syringes
- Small syringe (6-12cc) for injection of local anesthetic
- Large syringe (one 60cc or two 30cc) for aspiration
- Needles
- 18 gauge: knee
- 20 gauge: most other joints
- 25 gauge: MTP joints
- 27 gauge for anesthetic injection
- Collection tubes (red top and purple for crystal analysis)
- Culture bottles
- Consider utilizing U/S to assess for effusion
Procedure
General Setup
- Prep area with betadine or chlorhexadine using circular motion moving away from joint x 3
- Drape joint in sterile fashion
- Inject lidocaine with 25-30ga needle superficially and then into deeper tissues
- Insert 18ga needle (for larger joints) into joint space while pulling back on syringe
- Stop once you aspirate fluid; aspirate as much fluid as possible
- Send: cell count, culture, Gram Stain, crystal analysis
Specific Procedure
See joint-specific page for procedures
- Arthrocentesis: shoulder
- Arthrocentesis: elbow
- Arthrocentesis: wrist
- Arthrocentesis: finger
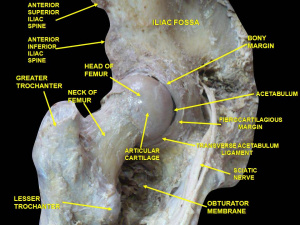
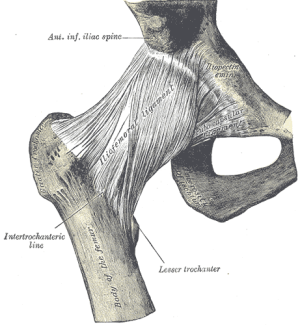
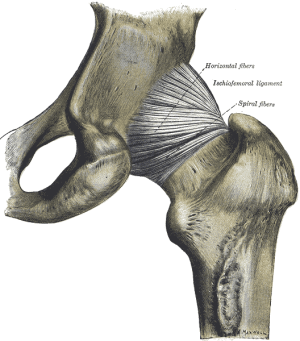
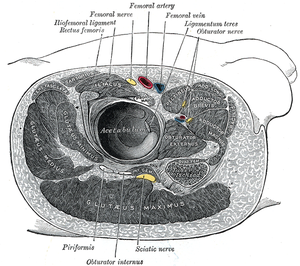
- Arthrocentesis: hip
- Arthrocentesis: knee
- Arthrocentesis: toe
Complications
General arthrocentesis complications
- Pain
- Infection
- Re-accumulation of effusion
- Damage to tendons, nerves, or blood vessels
Evaluation
Arthrocentesis of synoval fluid
| Synovium | Normal | Noninflammatory | Inflammatory | Septic |
| Clarity | Transparent | Transparent | Cloudy | Cloudy |
| Color | Clear | Yellow | Yellow | Yellow |
| WBC | <200 | <200-2000 | 200-50,000 |
>1,100 (prosthetic joint) >25,000; LR=2.9 >50,000; LR=7.7 >100,000; LR=28 |
| PMN | <25% | <25% | >50% |
>64% (prosthetic joint) >90% |
| Culture | Neg | Neg | Neg | >50% positive |
| Lactate | <5.6 mmol/L | <5.6 mmol/L | <5.6 mmol/L | >5.6 mmol/L |
| LDH | <250 | <250 | <250 | >250 |
| Crystals | None | None | Multiple or none | None |
- Viscosity of synovial fluid may actually be decreased in inflammatory or infectious etiologies, as hyaluronic acid concentrations decrease
- The presence of crystals does not rule out septic arthritis; however, the diagnosis is highly unlikely with synovial WBC < 50,000[1]
See Also
- Arthrocentesis
- Septic arthritis
- Septic arthritis (peds)
External Links
- http://www.youtube.com/watch?v=fZ2dcZhoGP8 Arthrocentesis
- http://emprocedures.com/arthrocentesis/introduction.htm
References
- ↑ Shah K, Spear J, Nathanson LA, Mccauley J, Edlow JA. Does the presence of crystal arthritis rule out septic arthritis?. J Emerg Med. 2007;32(1):23-6.