Decompression sickness
Background
- Also known as "the bends"
- Dissolved nitrogen (and occasionally helium) comes out of solution and forms bubbles in blood and tissue
- Occurs in rapid ascent in diving, and more rarely in military operations rapid ascent in high altitude aviation or hypobarics training
- Although decompression sickness can occur in both astronauts and divers, with similar physiology, the processes of disease differ due to a reduction in ambient pressure in space compared to an increase in ambient pressure when diving.
Diving Physiology
- Pascals Law applies to the diving body (without air filled areas such as lungs) states that the pressure applied to any part of the enclosed liquid will be transmitted equally in all directions through the liquid.
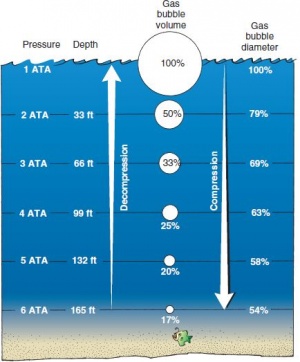
- Boyles Law applies to the diving body's air filled areas such as lungs, sinuses, middle ear, and states that the volume and pressure of a gas at a given temperature are inversely related.
- At 2 ATA (10m/33ft) a given gas would be 1/2 it's volume, at 3 ATA (20m/66ft) it would be 1/3 it's volume and so on.
- Dalton's Law applies to the total pressure of an ideal gas mixture being the sum of the partial pressures of each individual gas.
- Divers may used Enriched Air NITROX mixtures to proportionally increase partial pressures of oxygen and reduce partial pressures of nitrogen while diving.
- At extremes of depth, additional inert gasses such as helium in TRIMIX are used to further reduce partial pressures of both oxygen and nitrogen below toxic levels.
- Henry's Law applies to the dissolvability of gasses into fluids, including body tissues, being proportional to the partial pressure of the gas.
- The increased pressure at depth causes divers to breath their gas mix at increased pressure to defeat the external water pressure.
- Increased inhaled partial pressures of nitrogen increase risk of nitrogen narcosis, and dissolved nitrogen in tissues re-expanding in micro-bubbles on ascent is the essential cause of decompression sickness. This can affect divers at any depth, including commonly-seen recreational diving depths of 20m/60ft or less.
- Increased inhaled partial pressures of oxygen, generally beyond 1.4-1.6atm, increases risk of oxygen toxicity. This is typically not a substantial risk in common depths of recreational divers at 20m/60ft of depth or less, but can be for more advanced divers at deeper depths.
- The increased pressure at depth causes divers to breath their gas mix at increased pressure to defeat the external water pressure.
Clinical Features
- Symptom typically start soon after surfacing
Musculoskeletal System
- Joint pain and swelling (the "bends")
- Muscle weakness and fatigue
- Reduced range of motion and mobility
Nervous System
- Numbness, tingling, and paresthesia
- Confusion, disorientation, and loss of consciousness
- Seizures and stroke like symptoms
Circulatory System
- Arrhythmias and decreased cardiac output
- Shortness of breath and coughing
- Hypotension progressing to shock
Respiratory System
- Pulmonary edema and hemorrhage
- Pneumothorax and pneumomediastinum
- Pulmonary over inflation syndrome
Skin and Integumentary System
- Cutaneous lesions and rashes
- Skin necrosis and gangrene
Gastrointestinal System
- Nausea and vomiting
- Abdominal pain and cramping
- Diarrhea and constipation
Urinary System
- Hematuria and proteinuria
- Renal failure and acute kidney injury
- Urinary retention and incontinence
Eyes and Vision
- Diplopia
- Eye pain and redness
- Retinal hemorrhage and vision loss
Inner Ear and Hearing
- Hearing loss and tinnitus
- Vertigo and balance disturbance
- Ear pain and fullness
Differential Diagnosis
Diving Emergencies
- Barotrauma of descent
- Otic barotrauma
- Pulmonary barotrauma
- Sinus barotrauma
- Mask squeeze
- Barodentalgia (trapped dental air causing squeeze)
- Barotrauma of ascent
- Pulmonary barotrauma (pulmonary overpressurization syndrome)
- Decompression sickness (DCS)
- Arterial gas embolism
- Alternobaric vertigo
- Facial baroparesis (Bells Palsy)
- At depth injuries
- Oxygen toxicity
- Nitrogen narcosis
- Hypothermia
- Contaminated gas mixture (e.g. CO toxicity)
- Caustic cocktail from rebreathing circuit
Evaluation
Workup
- In patients that are ambiguous or decompensated, consider additional workup without delaying definitive treatment
- Other considerations
Diagnosis
Decompression sickness is a clinical diagnosis
- Pain may be reduced by BP cuff inflation over the joint to 150-200 mmHg
Type I (Pain only DCS)
- Involves the joints and extremities, with constitutional symptoms
- Usually only single joint is involved, most commonly:
- Shoulder
- Elbow
- Knee
- Skin and lymphatics
- Pruritus, stinging, paresthesias, hot/cold sensations
- Fine scarletiniform rash from nitrogen movement through sweat glands
- Cutis marmorata - marbling rash, purplish-bluish discoloration, otherwise common and normal in infants
- Pitting edema, peripheral swelling from lymphatic blockage
Type II (Serious DCS)
- Some consider multiple joint involvement qualifies as Type II
- Spinal cord involvement
- Ascending paralysis
- Signs often cannot be traced to single location in the cord (may have skip lesions)
- Limb weakness, paresthesias, or paralysis
- Urinary retention, fecal incontinence, or priapism
- Vestibular ("staggers") involvement
- Vertigo, hearing loss, tinnitus
- Differentiated from inner ear barotrauma which usually occurs on descent
- Vertigo, hearing loss, tinnitus
- Pulmonary "chokes"
- Cough, hemoptysis, dyspnea, substernal chest pain
Type III (Type II + gas embolism)
- Variety of stroke symptoms/signs
- May spontaneously resolve
Management
Treatment based almost solely on case reports and series
- ABCs/BLS/ACLS
- Denitrogenation with 100% NRB regardless of SpO2, and continue 2 hours after symptom resolution
- Keep supine, Trendelenburg not recommended[4]
- Initiate IV crystalloid fluids, rate of 250 cc/hr for first few hours
- Hyperbaric oxygen
- If due to high altitude aviation or hypobarics
- Descend to ground level ASAP
- Many divers carry insurance covering diving accidents and related medical problems, including costs of transfer for hyperbarics, through the Divers Alert Network - a worldwide, non-profit cooperative dedicated to dive safety. Coverage for transfer costs may require DAN arrange the transfer. Expert consultation over the phone, similar to Poison Control, may also be available. Whether or not you can confirm the patient has such coverage, and unless your facility has hyperbaric treatment available in-house, you should consider contacting them:
- Divers Alert Network 24/7 hotline - +1-919-684-9111
- If patient requires transport to another facility, consider ground transport, air transport at max of 1000 ft, or air transport with pressurization capability
- O2 with tight fitting mask during flight
- Consider adjuncts such as Lidocaine, Perfluorocarbon emulsions
Disposition
- Hyperbaric chamber and admission
Prognosis
- One study showed at an average of 6.1 yrs, almost 50% of patients had impairments[7]
- These include impaired urination, defecation, and sexual function
See Also
- Scuba diving emergencies
- Arterial gas embolism
- Diving Medicine
- Hyperbaric Medicine
- Ebullism syndrome
External Links
References
- ↑ Navy Department. US Navy Diving Manual. Revision 6. Vol 5: Diving Medicine and Recompression Chamber Operations. NAVSEA 0910-LP-106-0957. Washington, DC: Naval Sea Systems Command, 2008.
- ↑ Francis TJ, et al. Central nervous system decompression sickness: latency of 1070 human cases. Undersea Biomed Res. 1988; 15:403–417.
- ↑ Freiberger JJ, et al. The relative risk of decompression sickness during and after air travel following diving. Aviat Space Environ Med. 2002; 73:980–984.
- ↑ Moon RE, ry sl. Guidelines for treatment of decompression illness. Aviat Space Environ Med. 1997; 68:234–243.
- ↑ Marx et al. Rosen's Emergency Medicine - Concepts and Clinical Practice. 8th Ed. 2013. Ch 143. Pg. 1925.
- ↑ Edmonds C et al. Diving and Subaquatic Medicine, Fifth Edition. 2015. Decompression Sickness: Treatments. Pg 173.
- ↑ Vann RD, et al. Decompression illness. Lancet. 2011; 377(9760):153-164.