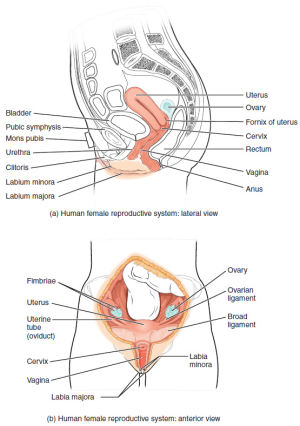
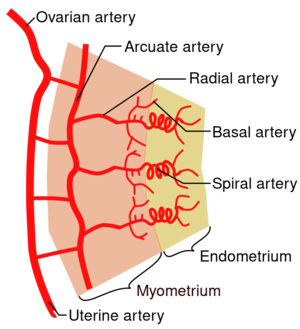
Nonpregnant vaginal bleeding
(Redirected from Vaginal Bleeding (Non-Pregnant))
This page is for women of reproductive age. For younger patients, see prepubertal vaginal bleeding.
Background
- This page is for the generalized approach to undifferentiated vaginal bleeding in non-pregnant women
- Normal menstruation:
- 28 +/- 7 day cycles
- 3-7 days of bleeding
- Usual amount bleeding per period 10-35 cc
- Each normal sized tampon or pad holds 5 cc when soaked through
- Bleeding from the uterine corpus that is irregular in volume, frequency or duration, in absence of pregnancy, is abnormal
- Vaginal bleeding before the age of menarche may be the result of infection, trauma (ex. sexual assault, foreign body) or a structural lesion
Vaginal bleeding definitions
- Menorrhagia: >7 day (prolonged) or >80 mL/day (excessive) uterine bleeding at regular intervals
- Metrorrhagia: irregular vaginal bleeding outside the normal cycle
- Menometrorrhagia: excessive irregular vaginal bleeding
- Intermenstrual bleeding: variable amounts between regular menstrual periods
- Midcycle spotting: spotting just before ovulation (due to decline in estrogen)
- Polymenorrhea: frequent and light bleeding
- Postcoital bleeding: vaginal bleeding after intercourse, suggesting cervical pathology
- Postmenopausal bleeding: recurrence of bleeding >6 mo after menopause
- Amenorrhea: bleeding that is absent for > 6 months
Clinical Features
- Vaginal bleeding in a non-pregnant woman
Differential Diagnosis
Nonpregnant Vaginal Bleeding
Systemic Causes
- Cirrhosis
- Coagulopathy (Von Willebrand disease, ITP)
- Group A strep vaginitis (prepubertal girls)
- Hormone replacement therapy
- Anticoagulants
- Selective Serotonin Reuptake Inhibitors (SSRIs)
- Hypothyroidism
- Polycystic Ovary Syndrome
- Secondary anovulation
Reproductive Tract Causes
- Adenomyosis
- Atrophic endometrium
- Dysfunctional uterine bleeding
- Endometriosis
- Leiomyoma (Fibroid)
- Foreign Body
- Infection (vaginitis, PID)
- IUD
- Neoplasia (especially in women >45 years old or in younger women with other risk factors)
- Vaginal Trauma
Evaluation
Work-Up
- Urine pregnancy
- Complete blood count
- Coags (if history of or suspect coagulopathy)
- TSH, prolactin (if suspect endocrine disorder)
- C. trachomatis and N. gonorrhoeae testing if risk of infection (consider with post-coital bleeding)
- Consider follow up for non-emergent pelvic ultrasound
- No indication for emergent ultrasound in ED
PALM-COEIN Classification of Vaginal Bleeding[1]
- PALM: structural causes
- Polyp (AUB-P)
- Adenomyosis (AUB-A)
- Leiomyoma (AUB-L)
- Malignancy and hyperplasia (AUB-M)
- COEIN: nonstructural causes
- Coagulopathy (AUB-C)
- Ovulatory dysfunction (AUB-O)
- Endometrial (AUB-E)
- Iatrogenic (AUB-I)
- Not yet classified (AUB-N)
Diagnosis
- Common etiologies by age:
- Age 12-18: most commonly immature hypothalamic-pituitary-ovarian axis, also consider bleeding dyscrasia
- Age 19-39: most commonly structural lesion (fibroid, polyp) or PCOS
- Age 40+: most commonly endometrial atrophy, also consider malignancy especially in post-menopausal[2]
- Hemodynamically stable patient in ED must rule-out:
- Pregnancy
- Trauma
- Bleeding dyscrasia
- Infection
- Retained vaginal foreign body
- If work up negative, can refer for further outpatient work up
Management
If you are concerned for malignancy, hormonal therapy should be avoided unless discussed with OBGYN, as these medications may interfere with possible biopsy results.
Mild Bleeding
- Iron supplementation
- 324mg ferrous sulfate tablet PO TID (each tab contains 65mg of elemental iron)
- NSAIDs
Moderate continued bleeding
Patients may benefit from initiation of short or long-term birth control for acute cessation.
Combined OCPs
- Any combined OCP that contains 35 ug of ethinyl estradiol TID for 7 days. (e.g., Ortho-Novum 1/35®)[3]
- 88% success, median time 3 days [4]
- Contraindications
- Cigarette smoking if older than 34 years
- Hypertension
- History of VTE
- Cerebrovascular disease
- CAD or valvular disease
- History of breast cancer
- Diabetes with vascular involvement
- Surgery with immobilization
- Liver cirrhosis
- Other pro-coagulative conditions (e.g. Lupus, Factor V Leiden)
- 20 mg PO TID for 7 days[3]
- 76% success, median time 3 days
- Alternative, not officially endorsed by ACOG: 150mg IM x 1 then 20 mg PO TID x 3 days
- In a trial of 48 patients all had cessation in 5 days.[5]
- Contraindications
- History of VTE
- History of arterial thromboembolic events
- History of breast cancer
- Liver disease
Life Threatening
- Establish large bore IV access
- Prepare for emergent blood transfusion uncrossmatched O-negative blood if typed blood is not available.
- It is possible to temporize bleeding w/ intravaginal packing with kerlix soaked in with thrombin
- If bleeding is due to a traumatic cause emergent surgical repair is necessary
- Tranexamic acid [6]
- Coordinate with OBGYN prior to administration due to the increased thrombotic risk
- Acutely 1.0-1.3 grams IV
- Then 1-1.3 g TID PO for 5 days
Pharmacologic Treatment Regimens For Acute Abnormal Uterine Bleeding[7][8]
| Drug | Suggested Dose | Contraindications |
| Conjugated equine estrogen | 25 mg IV every 4-6 h until bleeding stops, up to 24 h | Active or past thromboembolic disease, breast cancer, or liver disease |
| Combination oral contraceptive pills | 1 pill TID PO for 7 days or 1 pill bid PO for 5 days, then 1 pill daily until pack is finished | > 35 y who smoke, history of DVT or PE, breast cancer, liver disease, known thromboembolic disorders, pregnancy, ischemic heart disease, cerebrovascular disease, or uncontrolled hypertension |
| Progestin-only oral contraceptive pills (medroxyprogesterone acetate) | 20 mg TID PO for 7 days or 10 mg daily PO for 10 days | Active or past DVT or PE, liver disease, or breast cancer |
| NSAIDs: Ibuprofen | 200-400 mg 3-4 times/day PO for 5 days | Advanced renal disease |
| Antifibrinolytic agents (tranexamic acid) | 1.3 g TID PO for up to 5 days | Active intravascular clotting or subarachnoid hemorrhage |
Disposition
- Most can be discharged home with OB/GYN follow-up
- For severe anemia or persistent exceedingly heavy flow, consider admission and/or discussion with OB/GYN
- Surgical options, when medical management fails, include hysterectomy, endometrial baloon tamponade, dilatation and curettage, uterine artery embolization
See Also
Vaginal bleeding (main)
External Links
References
- ↑ The International Federation of Gynecology and Obstetrics
- ↑ https://www.ebmedicine.net/topics/gynecologic-obstetric/bleeding
- ↑ 3.0 3.1 Management of acute abnormal uterine bleeding in nonpregnant reproductive-aged women. Committee Opinion No. 557. American College of Obstetricians and Gynecologists. Obstet Gynecol 2013; 121:891–6. https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2013/04/management-of-acute-abnormal-uterine-bleeding-in-nonpregnant-reproductive-aged-women
- ↑ Munro MG, Mainor N, Basu R, Brisinger M, Barreda L. Oral medroxyprogesterone acetate and combination oral contraceptives for acute uterine bleeding: a randomized controlled trial. Obstet Gynecol. 2006 Oct;108(4):924-9. doi: 10.1097/01.AOG.0000238343.62063.22. PMID: 17012455.
- ↑ Ammerman SR, Nelson AL. A new progestogen-only medical therapy for outpatient management of acute, abnormal uterine bleeding: a pilot study. Am J Obstet Gynecol. 2013. 208(6):499.e1-e5.
- ↑ Leminen and Hurskainen. Tranexamic acid for the treatment of heavy menstrual bleeding: efficacy and safety. Int J Womens Health. 2012; 4: 413–421.
- ↑ American College of Obstetricians and Gynecologists. ACOG Committee Opinion No. 557: management of acute abnormal uterine bleeding in nonpregnant reproductiveaged women. Obstet Gynecol. 2013;121(4):891-896
- ↑ Tibbles CD. Selected gynecologic disorders: abnormal uterine bleeding in the nonpregnant patient. In: Marx JA, Hockberger RS, Walls RM, eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. Philadelphia, PA: Mosby-Elsevier; 2010: 1325-1332.