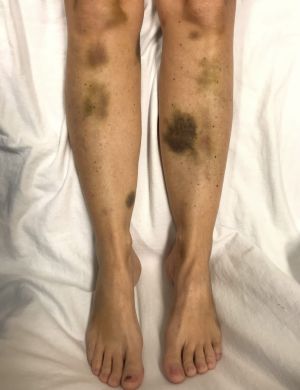
Thrombotic thrombocytopenic purpura
(Redirected from Thrombotic Thrombocytopenic Purpura (TTP))
Background
- Untreated mortality is >90%
- Similar clinical symptoms but different pathophysiology than HUS
- HUS more common in pediatrics
- Microangiopathic Hemolytic Anemia (MAHA) + low Platelets is TTP until proven otherwise
- MAHA is non-immune hemolysis (Coomb's-negative hemolysis) causing RBC fragmentation producing schistocytes
- Can occur as a result of Plavix (clopidogrel) use, especially within the first 2 weeks
Pathophysiology
- Insufficient ADAMTS-13 activity allows vWF multimers to accumulate in microcirculation which leads to platelet aggregation/thrombocytopenia and hemolysis of RBCs. Platelet clots are transient, but the symptoms especially neuro, can be in flux.
Risk Factors
- Congenitally deficient ADAMTS-13 activity AND:
- Pregnancy OR
- Infection OR
- Inflammation OR
- Medication use (quinolones, ticlopidine, clopidogrel)
Clinical Features
Pentad (rarely all present)[1]
- Microangiopathic Hemolytic Anemia (MAHA)
- Thrombocytopenia
- Fever
- Renal pathology
- CNS abnormalities (headache, seizure, altered mental status, CVA, coma)
- Neuro symptoms are often transient, may not be present in ED
- TTP pentad mnemonic = FAT RN
- Fever, Anemia, Thrombocytopenia, Renal, Neuro Symptoms
- All features DO NOT need to be present at the same time
- Consider diagnosis without the full pentad
Differential Diagnosis
- Other MAHAs (eg, HUS, DIC, malignant hypertension)
- ITP
- Sepsis
- SLE
- HELLP syndrome
- Anemia, platelet count, and LDH tend to be more severe in TTP; LFTs more severe in HELLP
Microangiopathic Hemolytic Anemia (MAHA)
- Disseminated Intravascular Coagulation (DIC)
- Thrombotic Thrombocytopenic Purpura (TTP)
- Hemolytic Uremic Syndrome (HUS)
- HELLP syndrome
- Heparin-Induced Thrombocytopenia (HIT)
- Hereditary spherocytosis
- Paroxysmal nocturnal hemoglobinuria (PNH)
- Malignant hypertension
- Scleroderma
- Antiphospholipid Syndrome (APS)
- Other medical causes: malignancy, renal allograft rejection, vasculitides like polyarteritis nodosa and Wegener's granulomatosis
- Drugs: chemotherapy; Clopidogrel (Plavix) associated with TTP
- Nonvascular causes: prosthetic valve (more common with mechanical, more common at aortic valve), LVAD, TIPS, coil embolization, patched AV shunt, AVM
Thrombocytopenia
Decreased production
- Marrow infiltration (tumor or infection)
- Viral infections (rubella, HIV)
- Marrow suppression (commonly chemotherapy or radiation)
- Congenital thrombocytopenia
- Fanconi anemia
- Alport syndrome
- Bernand Soulier
- Vitamin B12 and/or folate deficiency
Increased platelet destruction or use
- Idiopathic thrombocytopenic purpura
- Thrombotic Thrombocytopenic Purpura (TTP)
- Hemolytic Uremic Syndrome (HUS)
- Disseminated Intravascular Coagulation (DIC)
- Viral infections (HIV, mumps, varicella, EBV)
- Drugs (heparin, protamine)
- Postransfusion or Posttransplantation
- Autoimmune destruction (SLE or Sarcoidosis)
- Mechanical destruction
- Artificial valves
- ECMO
- HELLP syndrome
- Excessive hemorrhage
- Hemodialysis, extracorporeal circulation
- Splenic Sequestration
- Occurs in Sickle cell disease and Cirrhosis
Drug Induced
- sulfa antibiotics, ETOH, ASA, thiazide diuretics/furosemide
Comparison by Etiology
| ITP | TTP | HUS | HIT | DIC | |
|---|---|---|---|---|---|
| ↓ PLT | Yes | Yes | Yes | Yes | Yes |
| ↑PT/INR | No | No | No | +/- | Yes |
| MAHA | No | Yes | Yes | No | Yes |
| ↓ Fibrinogen | No | No | No | No | Yes |
| Ok to give PLT | Yes | No | No | No | Yes |
Evaluation
Workup
- CBC with peripheral smear (anemia, microspherocytes, thrombocytopenia are suggestive findings)
- Microangiopathic hemolytic anemia produces schistocytes
- LDH (elevated)
- Haptoglobin (decreased)
- Reticulocyte count (appropriate)
- Urinalysis (hemoglobinuria)
- Creatinine (possibly elevated)
- LFTs (increased bilirubin)
- PT/PTT/INR (normal; differentiates from DIC)
- Urine pregnancy (significant association between pregnancy and TTP)
Diagnosis
- Plasma ADAMTS-13 Level:
- Ideally drawn prior to initiation of treatment, but results rarely available in the ER.
- Level Interpretation
- <10 IU/dL Confirms the diagnosis
- 10-20 IU/dL Equivocal result
- >20 IU/dL within normal, consider other diagnoses
- PLASMIC Score: <5 features effectively rules out TTP (99% NPV)[2]
- Platelets <30 x 109/L
- Hemolysis with reticulocye count >2.5%, indirect bilirubin >2mg/dL, or low haptoglobin
- MCV <90fL
- INR <1.5
- Creatinine <2mg/dL
- No Current Cancer
Management
Management ideally done in consultation with heme/onc[3]
- Plasma exchange (plasmapheresis)
- Replaces defective or insufficient ADAMTS-13 and clears vWF multimers
- FFP Transfusion
- Contains ADAMTS-13
- Should only be initiated if delay in plasmapheresis
- Glucocorticoids
- Consider 1 mg/kg prednisone PO or methylprednisolone 125 mg IV[4][5]
- Biologic Therapies: ISTH guidelines now recommend adding both empiric rituximab and caplacizumab for patients with high pretest probability while awaiting ADAMTS-13 levels.[6]
- Rituximab is a monoclonal antibody against CD20 and is used in many autoimmune disorders
- Caplacizumab is a monoclonal antibody blocking platelet-vWF interactions and thus formation of microvascular thrombosis.
- Caplacizumab may be withheld in patients with whom no ADAMTS-13 can be obtained as there are concerns for increased bleeding risk with this therapy
- In patients with low pretest probability, consider empiric plasma exchange and steroids and withhold these biologics pending ADAMTS-13 results.
- Transfusion of pRBCs (only severe bleeding)
- Generally only indicated if plasma exchange cannot be performed immediately
- Splenectomy - 2nd line therapy after stabilization
- Inhibitor antibody is made in the spleen
- Platelet transfusion is AVOIDED
- Only used for life-threatening bleeding or intracranial hemorrhage under guidance from hematologist
- Platelet infusion may lead to acutely worsened thrombosis, renal failure, and death
Disposition
- Admit for plasma exchange
Medication Dosing
- Methylprednisolone 125 mg IV (or prednisone 1 mg/kg PO) IV/PO
See Also
References
- ↑ George J: Clinical practice. Thrombotic thrombocytopenic purpura. N Engl J Med 2006; 354:1927
- ↑ Paydary K, Banwell E, Tong J, Chen Y, Cuker A. Diagnostic accuracy of the PLASMIC score in patients with suspected thrombotic thrombocytopenic purpura: A systematic review and meta-analysis. Transfusion. 2020 Sep;60(9):2047-2057. doi: 10.1111/trf.15954. Epub 2020 Aug 5. PMID: 32757237.
- ↑ George J. How I treat patients with thrombotic thrombocytopenic purpura: 2010. Blood 2010; 116:4060
- ↑ Bell WR, Braine HG, Ness PM, Kickler TS. Improved survival in thrombotic thrombocytopenic purpura-hemolytic uremic syndrome. Clinical experience in 108 patients. N Engl J Med 1991; 325:398.
- ↑ Balduini CL, Gugliotta L, Luppi M, et al. High versus standard dose methylprednisolone in the acute phase of idiopathic thrombotic thrombocytopenic purpura: a randomized study. Ann Hematol 2010; 89:591.
- ↑ Zheng XL, Vesely SK, Cataland SR, Coppo P, Geldziler B, Iorio A, Matsumoto M, Mustafa RA, Pai M, Rock G, Russell L, Tarawneh R, Valdes J, Peyvandi F. ISTH guidelines for treatment of thrombotic thrombocytopenic purpura. J Thromb Haemost. 2020 Oct;18(10):2496-2502. doi: 10.1111/jth.15010. Epub 2020 Sep 11. PMID: 32914526; PMCID: PMC8091490.