Heparin-induced thrombocytopenia
(Redirected from Heparin-Induced Thrombocytopenia (HIT))
Background
- Pathologic activation / consumption of platelets due to antibodies against heparin-platelet complex
- Can be caused by unfractionated heparin or LMWH (10 times more common in unfractionated)
- Occurs in 0.5-5% of patients treated with heparin[1]
- Thrombosis occurs in 35-75% of patients ; 20-30% die within 1 month[1]
- HYPER-coagulable, despite low platelet count
- activated platelets bound in clot, thus low platelet count
- bleeding is unusual
Type 1 HIT
- Onset within 48h of initiating heparin
- Drop in platelet count due to platelet activation by heparin
- Platelet count usually normalizes in a few days with continued heparin treatment[2]
Type 2 HIT
- Immune-mediated process
- Onset typically 5-10 days after exposure to heparin
- Complicated by thrombosis[2]
Clinical Features
- The 4 T's: (formal scoring system below)
- Thrombocytopenia
- Timing (5-14d)
- Thrombosis
- No oTher cause
Immediate Symptoms
- Flushing
- Tachycardia
- Hypotension
- Dyspnea
Delayed Symptoms
- >50% decrease in platelet count (median nadir is ~60K; rarely <20K)
- DVT or PE
- Cerebral vein or adrenal vein thrombosis
- Limb arterial occlusion
- CVA
- MI
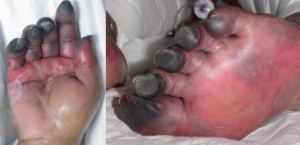
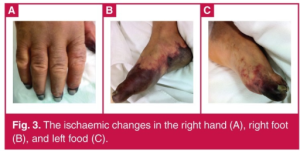
- Skin necrosis
Differential Diagnosis
Thrombocytopenia
Decreased production
- Marrow infiltration (tumor or infection)
- Viral infections (rubella, HIV)
- Marrow suppression (commonly chemotherapy or radiation)
- Congenital thrombocytopenia
- Fanconi anemia
- Alport syndrome
- Bernand Soulier
- Vitamin B12 and/or folate deficiency
Increased platelet destruction or use
- Idiopathic thrombocytopenic purpura
- Thrombotic Thrombocytopenic Purpura (TTP)
- Hemolytic Uremic Syndrome (HUS)
- Disseminated Intravascular Coagulation (DIC)
- Viral infections (HIV, mumps, varicella, EBV)
- Drugs (heparin, protamine)
- Postransfusion or Posttransplantation
- Autoimmune destruction (SLE or Sarcoidosis)
- Mechanical destruction
- Artificial valves
- ECMO
- HELLP syndrome
- Excessive hemorrhage
- Hemodialysis, extracorporeal circulation
- Splenic Sequestration
- Occurs in Sickle cell disease and Cirrhosis
Drug Induced
- sulfa antibiotics, ETOH, ASA, thiazide diuretics/furosemide
Comparison by Etiology
| ITP | TTP | HUS | HIT | DIC | |
|---|---|---|---|---|---|
| ↓ PLT | Yes | Yes | Yes | Yes | Yes |
| ↑PT/INR | No | No | No | +/- | Yes |
| MAHA | No | Yes | Yes | No | Yes |
| ↓ Fibrinogen | No | No | No | No | Yes |
| Ok to give PLT | Yes | No | No | No | Yes |
Microangiopathic Hemolytic Anemia (MAHA)
- Disseminated Intravascular Coagulation (DIC)
- Thrombotic Thrombocytopenic Purpura (TTP)
- Hemolytic Uremic Syndrome (HUS)
- HELLP syndrome
- Heparin-Induced Thrombocytopenia (HIT)
- Hereditary spherocytosis
- Paroxysmal nocturnal hemoglobinuria (PNH)
- Malignant hypertension
- Scleroderma
- Antiphospholipid Syndrome (APS)
- Other medical causes: malignancy, renal allograft rejection, vasculitides like polyarteritis nodosa and Wegener's granulomatosis
- Drugs: chemotherapy; Clopidogrel (Plavix) associated with TTP
- Nonvascular causes: prosthetic valve (more common with mechanical, more common at aortic valve), LVAD, TIPS, coil embolization, patched AV shunt, AVM
Evaluation
- Serotonin release assay (SRA) = gold standard
- Anti-PF4 plus SRA has combined sensitivity of 99% [3]
- Positivity determined by optical density (OD) reported with assay (same concept as a titer)
- OD <1 = <5% chance of HIT
- OD 1.4 = 50% chance of HIT
- OD >2 = 90% chance of HIT
Pre-test Probability Scoring (The 4 T Score)[4]
- Thrombocytopenia
- 2 points: platelets > 50% fall AND nadir > 20k
- 1 points: patient 30-50% fall OR nadir 10-19k
- Timing
- 2 points: clear onset 5-10 days OR platelet fall < 1 day with prior heparin exposure within 30 days
- 1 point: likely onset 5-10 days OR fall < 1 day with prior heparin exposure 30-100 days
- Thrombosis
- 2 points: new thrombosis or skin necrosis at injection sites
- 1 point: suspected thrombosis or progressive/recurrent thrombosis
- Likelihood of other causes
- 2 points: none apparent
- 1 point: possible
- Scoring
- ≤3 is low risk and do not require further testing or heparin discontinuation
- ≥4 should have serologic testing performed, heparin discontinued, and alternative anticoagulation started
Management
- Discontinue all heparin products [5]
- Do not give platelets (may precipitate thrombosis)
- Start anticoagulation with no heparin based compound such as a direct thrombin inhibitor: [lepirudin (unless renal failure), argatroban (unless hepatobiliary disease), bivalirudin] or direct Xa inhibitor (fondaparinux, danaparoid)
- 4T Score ≥4 with/without thrombosis and average bleeding risk should receive therapeutic dose
- 4T Score ≥4 with/without thrombosis and high bleeding risk should receive prophylactic dose
- Avoid warfarin until platelets >100K-150K
- Those already on warfarin should receive vitamin K to restore protein C & S levels
Disposition
- Admit (with hematology consult)
Calculators
4Ts Score for HIT
| Criteria | 0 Points | 1 Point | 2 Points |
|---|---|---|---|
| Thrombocytopenia | 1 <30% fall or nadir <10 | 30–50% fall or nadir 10–19 | >50% fall and nadir ≥20 |
| Timing of platelet fall | 1 <4 days without recent heparin | Consistent but unclear; or fall after day 10 | 5–10 days; or ≤1 day if recent heparin |
| Thrombosis or other sequelae | 1 None | Progressive/recurrent or suspected | Confirmed new thrombosis or skin necrosis |
| Other causes for thrombocytopenia | 1 Definite other cause present | Possible other cause | No other cause apparent |
| 4Ts Score | / 8 | ||
| 0–3 | Low probability (~5% risk of HIT). HIT antibody testing usually not needed. |
|---|---|
| 4–5 | Intermediate probability (~14% risk). Send HIT antibody; consider alternative anticoagulation. |
| 6–8 | High probability (~64% risk). Start alternative anticoagulant; send confirmatory testing. |
|
See Also
References
- ↑ 1.0 1.1 Lovecchio F. Heparin-induced thrombocytopenia. Clin Toxicol (Phila). 2014 Jul;52(6):579-83
- ↑ 2.0 2.1 Warkentin T. et al. Heparin-induced thrombocytopenia: recognition, treatment, and prevention: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy. Chest. 2004 Sep;126(3 Suppl):311S-337S
- ↑ Warkentin TE, et al. Chest. 2008;133(6 Suppl):340S-380S.
- ↑ Janz TG, Hamilton GC: Disorders of Hemostasis, in Marx JA, Hockberger RS, Walls RM, et al (eds): Rosen’s Emergency Medicine: Concepts and Clinical Practice, ed 7. St. Louis, Mosby, Inc., 2010, (Ch) 120: p 1578-1589.
- ↑ Cuker A, Arepally GM, Chong BH, Cines DB, Greinacher A, Gruel Y, Linkins LA, Rodner SB, Selleng S, Warkentin TE, Wex A, Mustafa RA, Morgan RL, Santesso N. American Society of Hematology 2018 guidelines for management of venous thromboembolism: heparin-induced thrombocytopenia. Blood Adv. 2018 Nov 27;2(22):3360-3392. doi: 10.1182/bloodadvances.2018024489. PMID: 30482768; PMCID: PMC6258919.