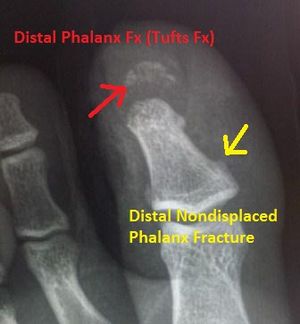
Distal phalanx (finger) fracture
Background
- Fracture of distal portion of distal phalanx is also known as a "Tuft fracture"
- Hand: finger slammed in door
- Foot: stubbed toe or dropped a heavy object
Finger (phalanx) fracture types
- Proximal Phalanx (Finger) Fracture
- Middle Phalanx (Finger) Fracture
- Distal Phalanx (Finger) Fracture
Clinical Features
- Pain and/or swelling of the digit
- Sensation usually intact
- Pain on palpation
Differential Diagnosis
Distal Finger (Including Nail) Injury
- Distal interphalangeal dislocation (finger)
- Distal phalanx (finger) fracture
- Finger amputation
- Fingertip avulsion
- Finger infection
- Nailbed laceration
- Nail avulsion
- Subungual hematoma
Hand and Finger Fracture Types
Evaluation
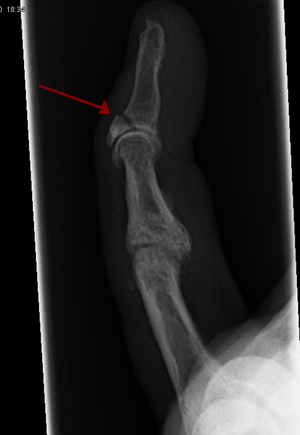
Distal phalanx fracture concerning for Mallet finger
Imaging
- Hand and/or finger x-rays
Diagnosis
- Comminuted tuft fracture
- Stable
- Longitudinal fracture
- Usually non-displaced and stable
- Transverse fracture
- Evaluate for angulation/displacement
- Intraarticular fracture
- Evaluate additionally for:
- Tendon damage
- Second fracture
Management
General Fracture Management
- Acute pain management
- Open fractures (excluding distal phalanx fractures) require immediate IV antibiotics and urgent surgical washout
- Neurovascular compromise from fracture requires emergent reduction and/or orthopedic intervention
Specific Management
- Nonoperative
- Nondisplaced: Splint with the DIP joint in extension (splint should extend past the tip of the distal phalanx
- Most cases
- Eval nail bed
- Is a Nailbed laceration underneath possible?
- Digital blocks can be helpful for evaluation and management
- Do not attempt to reduce comminuted tuft fracture
- Nondisplaced: Splint with the DIP joint in extension (splint should extend past the tip of the distal phalanx
- Call Hand or Ortho (institution dependent) for complex finger injuries
- Nailbed laceration with distal phalanx fractures can be complicated and result in an open fracture
Prophylactic Antibiotics
Controversial but in general, prophylactic antibiotics are indicated for grossly contaminated open wounds, and can be considered in high risk patients (ex. diabetics, peripheral artery disease). Otherwise, NOT indicated in open distal phalanx fracture (aka tuft fracture) as long as:
- Fracture is at distal phalanx (i.e. tuft fracture)
- Intact digital arteries
- Clean wound
Disposition
- Refer for:
- Tendon dysfunction
- Nerve dysfunction
- Displacement or angulation
- Intraarticular fracture
- Complex involving Nailbed laceration