Placenta previa
Background
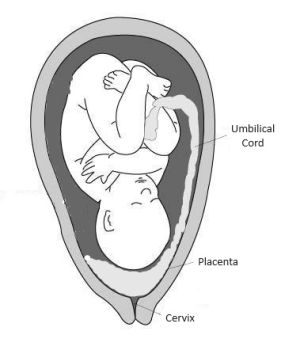
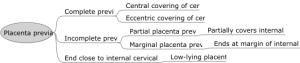
- Placenta that implants over or near the internal cervical os
- Complete — entirely covers the os
- Partial — partially covers the os
- Marginal — edge within 2 cm of the os
- Occurs in ~0.5% of pregnancies at term[1]
- Leading cause of antepartum hemorrhage in the third trimester
- Do NOT perform digital or speculum exam — may provoke life-threatening hemorrhage
Risk Factors
- Prior cesarean delivery or uterine surgery
- Prior placenta previa (recurrence 4-8%)
- Advanced maternal age (>35)
- Multiparity
- Cigarette smoking
- Cocaine use
- Assisted reproduction (IVF)
Clinical Features
- Painless, bright red vaginal bleeding — typically in late 2nd or 3rd trimester
- Initial "sentinel bleed" often self-limited
- May present with profuse hemorrhage and hemodynamic instability
- Uterus is soft and non-tender (distinguishes from abruption)
- Fetal heart tones usually normal unless maternal shock present
Differential Diagnosis
Abdominal Pain in Pregnancy
The same abdominal pain differential as non-pregnant patients, plus:
<20 Weeks
- Ectopic pregnancy
- First trimester abortion
- Complete abortion
- Threatened abortion
- Inevitable abortion
- Incomplete abortion
- Missed abortion
- Septic abortion
- Round ligament stretching
- Incarcerated uterus
- Malposition of the uterus
>20 Weeks
- Labor/Preterm labor
- Placental abruption
- Placenta previa
- Vasa previa
- Uterine rupture
- Vaginal trauma
- HELLP syndrome
- Cholestasis of pregnancy
- Chorioamnionitis
- Incarcerated uterus
- Acute fatty liver of pregnancy
- Malposition of the uterus
- Placenta accreta
- Placenta increta
- Placenta percreta
Any time
- Hemorrhagic ovarian cyst
- Fibroid degeneration or torsion
- Ovarian torsion
- Constipation
Evaluation
- Transabdominal ultrasound — first-line to confirm placental position
- Transvaginal US is safe and more accurate than transabdominal[2]
- Labs
- Fetal monitoring — continuous cardiotocography
- Consider Kleihauer-Betke test to quantify fetomaternal hemorrhage
Management
Hemodynamically Unstable / Active Hemorrhage
- Aggressive IV fluid resuscitation with crystalloid
- Activate massive transfusion protocol as needed
- Emergent cesarean delivery — consult OB/GYN immediately
- Goal: maternal stabilization takes priority
Stable Patient
- Admit to labor and delivery
- Strict bed rest, NPO
- Continuous fetal monitoring
- OB/GYN consultation for delivery planning
- If preterm (<34 weeks): antenatal corticosteroids for fetal lung maturity
- If preterm with contractions: tocolysis may be considered
Disposition
- All patients with placenta previa and vaginal bleeding require admission
- Asymptomatic previa diagnosed on routine US — outpatient OB follow-up with pelvic rest