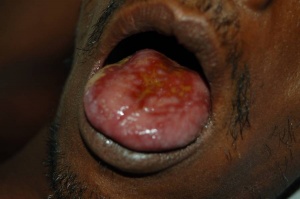
Paraquat toxicity
Background
- Paraquat is an herbicide that has a rapid and large distribution and can be fatal even with small ingestions. It has a high case-fatality rate (>50%)[1] which makes it a frequent means of suicide in the developing world, as well as a dangerous accidental occupational exposure.
- Paraquat exerts its toxic effects via multiple proposed mechanisms, including lipid peroxidation and generation of reactive oxygen species, direct mitochondrial toxicity, and apoptosis.
Clinical Features
Overall, pulmonary and renal toxicities predominate and are the primary cause of mortality. GI toxicity is nearly universal and is probably an under-recognized cause of mortality secondary to erosion and perforation.
- Gastrointestinal: predominate early
- Paraquat tongue
- Esophageal and gastric erosion
- Nausea and vomiting
- Pulmonary: occurs due to distribution to pneumocytes
- Pneumonitis
- Pulmonary fibrosis (delayed)
- Multiorgan failure
- Acute renal failure
- Hepatic necrosis
- Myocardial necrosis
- Internal bleeding
Differential Diagnosis
Toxic Ingestion
Oral Burns/Mucositis
- Burns
- Infectious Causes
- [[Aphthous stomatitis|Aphthous Ulcer
- Herpes simplex infection
- Coxsackie virus
- Tonsillitis
- Methotrexate/chemotherapy toxicity
Acute Dyspnea
Acute dyspnea
Emergent
- Pulmonary
- Airway obstruction
- Anaphylaxis
- Angioedema
- Aspiration
- Acute respiratory distress syndrome (ARDS)
- Asthma
- Cor pulmonale
- Epiglottitis
- Inhalation exposure
- Noncardiogenic pulmonary edema
- Pneumonia
- Pneumocystis Pneumonia (PCP)
- Pulmonary embolism
- Pulmonary hypertension
- Tension pneumothorax
- Idiopathic pulmonary fibrosis acute exacerbation
- Cystic fibrosis exacerbation
- Cardiac
- Other Associated with Normal/↑ Respiratory Effort
- Other Associated with ↓ Respiratory Effort
Non-Emergent
- ALS
- Ascites
- Uncorrected ASD
- Congenital heart disease
- COPD exacerbation
- Deconditioning
- Fever
- Hyperventilation
- Interstitial lung disease
- Neoplasm
- Obesity
- Obstructive sleep apnea
- Panic attack
- Pleural effusion
- Polymyositis
- Porphyria
- Pregnancy
- Rib fracture
- Spontaneous pneumothorax
- Thyroid Disease
- URI
- Vocal cord dysfunction
Evaluation
Workup
- Labs
- Imaging
- CXR
- EKG
- consider CT if stable to evaluate for perforation/mediastinitis
Diagnosis
- Based on urine test
Management
Patients who present in extremis after an ingestion will not survive regardless of management and should be treated palliatively. Large >50mL ingestions of paraquat are universally fatal. Aggressive resuscitation is futile.
Resuscitation
- Airway: consider early aggressive intubation for any respiratory distress or large (>100mL) ingestions
- Breathing: CXR, O2
- Avoid aggressive oxygen therapy unless severe hypoxia due to increased free radical production
- Circulation: may develop early shock and require aggressive inotropic support
Decontamination
- Paraquat is absorbed transdermally. Unprotected first responders and healthcare workers are at risk
- Remove clothing and wash patient's skin if spillage or obvious skin involvement present
- Consider activated charcoal or Fuller's Earth if within 1-2 hrs of ingestion
- Consider NG tube for administration of activated charcoal
- Must weigh risks as NGT placement can exacerbate caustic injury
Supportive Care
- IV fluids: patients often 2-3L fluid down
- Pain control
Antidotes/Additional Therapies
- Some centers administer glucocorticoids (typically dexamethasone 6mg-10mg IV q6h)
- Consider NAC, vitamin C, other free radical scavengers in consultation with toxicologist or poison control
- No role for extracorporeal elimination (hemodialysis/Hemoperfusion, CRRT)
Disposition
- If small/trivial exposure and patient asymptomatic at 6 hours, unlikely to manifest a significant toxicity
- Any symptomatic exposure requires admission for close hemodynamic monitoring and supportive care
See Also
External Links
References
- ↑ Gawaramanna I, Buckley N. Medical management of paraquat ingestion. Br J Clin Pharmacol. 2011;72(5):745–757