Mucormycosis
Background
- Opportunistic invasive fungal infection, typically affecting immunocompromised patients (especially uncontrolled diabetics)[1]
- Caused by saprophytic fungi (Mucorales)
- Found in soil, bread mold, decaying fruits[2]
- Fungal spores are dispersed in air → route of entry is inhalation[1]
- Infection typically begins in nose and paranasal sinuses
- Can also affect pulmonary, GI and CNS systems
- Mucorales fungi have vascular proclivity, and can cause thrombosis → tissue and bone necrosis
- Prognosis is poor, with 17-51% mortality[3], higher in cerebral involvement[4]
Clinical Types
- 6 clinical types, based on location of infection[1][2]
- Rhino-orbital-cerebral (most common form)
- Pulmonary
- Gastrointestinal
- Cutaneous
- Disseminated
- Miscellaneous
Clinical Features
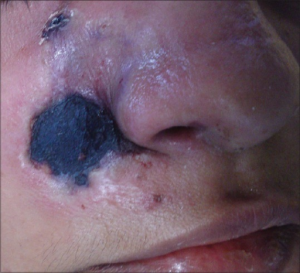
- Rhinocerebral form initially mimics acute bacterial sinusitis (pain/swelling of cheeks and periorbital region)[2]
- A much more rapid, extensive expansion of the fungus to the surrounding anatomy is classic
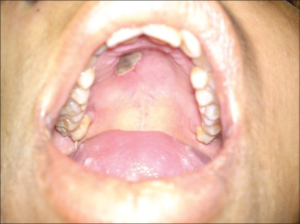
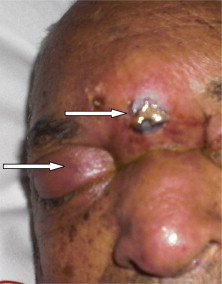
- Can spread to orbits, oropharynx, nasopharynx, brain, nearby vasculature leading to → vision changes, nasopharyngeal and oropharyngeal ulceration or eschars, facial edema/pain, cranial nerve deficits, headache
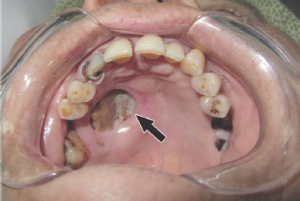
- Black palatal discoloration indicates palatal necrosis
Differential Diagnosis
Rhinorrhea
- Upper respiratory infection, influenza
- Sinusitis
- Juvenile nasopharyngeal angiofibroma
- Nasal polyp
- Nasal mass
- Nasal foreign body
- CSF leak (e.g. basilar skull fracture)
- Toxic inhalation (e.g. selenium toxicity, neurotoxic shellfish poisoning)
Headache
Common
Killers
- Meningitis/encephalitis
- Myocardial ischemia
- Retropharyngeal abscess
- Intracranial Hemorrhage (ICH)
- SAH / sentinel bleed
- Acute obstructive hydrocephalus
- Space occupying lesions
- CVA
- Carbon monoxide poisoning
- Basilar artery dissection
- Preeclampsia
- Cerebral venous thrombosis
- Hypertensive emergency
- Depression
Maimers
- Giant cell arteritis of temporal artery (temporal arteritis)
- Idiopathic intracranial hypertension (Pseudotumor Cerebri)
- Acute Glaucoma
- Acute sinusitis
- Cavernous sinus thrombosis or cerebral sinus thrombosis
- Carotid artery dissection
Others
- Mild traumatic brain injury
- Trigeminal neuralgia
- TMJ pain
- Post-lumbar puncture headache
- Dehydration
- Analgesia abuse
- Various ocular and dental problems
- Herpes zoster ophthalmicus
- Herpes zoster oticus
- Cryptococcosis
- Febrile headache (e.g. pyelonephritis, nonspecific viral infection)
- Ophthalmoplegic migraine
- Superior Vena Cava Syndrome
Aseptic Meningitis
- Viral
- Tuberculosis
- Lyme disease
- Syphilis
- Leptospirosis
- Fungal (AIDS, transplant, chemotherapy, chronic steroid use)
- Noninfectious
Evaluation
- CT scan of sinuses with IV contrast can assist with diagnosis, often preferred over MRI as initial study as it is more readily available and more sensitive than MRI for bony erosions[5]
- PCR-based techniques on invasively-obtained histologic samples demonstrating fungal elements is confirmatory[6]
Management
- Emergent ENT consult for OR debridement (definitive treatment)
- Start Amphotericin B 1mg/kg IV[2] OR
- Liposomal Amphotericin B 5-10mg/kg[3]
- Aggressive resuscitation, airway management, and supportive care while in ED.
- Hyperbaric oxygen therapy[4] and iron chelation (iron is required for fungal growth) may also help.[2]
- Do not use deferoxamine (can worsen disease caused by certain fungal genera) - deferiprone is preferred
See Also
External Links
References
- ↑ 1.0 1.1 1.2 Selvamani M, Donoghue M, Bharani S, Madhushankari GS. Mucormycosis causing maxillary osteomyelitis. Journal of Natural Science, Biology, and Medicine. 2015;6(2):456-459. doi:10.4103/0976-9668.160039.
- ↑ 2.0 2.1 2.2 2.3 2.4 Motaleb HYA, Mohamed MS, Mobarak FA. A Fatal Outcome of Rhino-orbito-cerebral Mucormycosis Following Tooth Extraction: A Case Report. Journal of International Oral Health : JIOH. 2015;7(Suppl 1):68-71.
- ↑ 3.0 3.1 Bellazreg F, Hattab Z, Meksi S, et al. Outcome of mucormycosis after treatment: report of five cases. New Microbes and New Infections. 2015;6:49-52. doi:10.1016/j.nmni.2014.12.002.
- ↑ 4.0 4.1 Mohamed MS, Abdel-Motaleb HY, Mobarak FA. Management of rhino-orbital mucormycosis. Saudi Medical Journal. 2015;36(7):865-868. doi:10.15537/smj.2015.7.11859.
- ↑ Aribandi M, McCoy VA, Bazan C 3rd. Imaging features of invasive and noninvasive fungal sinusitis: a review. Radiographics. 2007 Sep-Oct;27(5):1283-96. doi: 10.1148/rg.275065189. PMID: 17848691.
- ↑ Walsh TJ, Gamaletsou MN, McGinnis MR, Hayden RT, Kontoyiannis DP. Early clinical and laboratory diagnosis of invasive pulmonary, extrapulmonary, and disseminated mucormycosis (zygomycosis). Clin Infect Dis. 2012 Feb;54 Suppl 1:S55-60. doi: 10.1093/cid/cir868. PMID: 22247446.