Congestive heart failure
(Redirected from Congestive Heart Failure (CHF))
This page is for adult patients. For pediatric patients, see: congestive heart failure (peds)
Background
- Assume valvular problem in new-onset CHF
- Assume valve thrombosis in CHF with a prosthetic valve
- Do not give vasodilators in aortic stenosis, HOCM; yes in mitral regurgitation
Classification
- Systolic: poor contraction (↓EF) and decreased forward flow
- Diastolic: good contraction (normal EF) but stiff ventricles and poor filling
- Left-sided: LV failure, poor organ perfusion, dyspnea from backup in lung
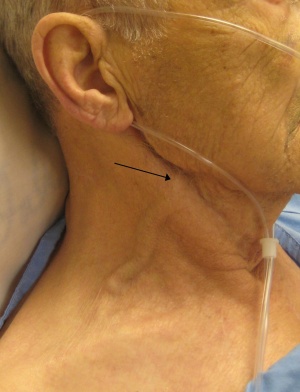
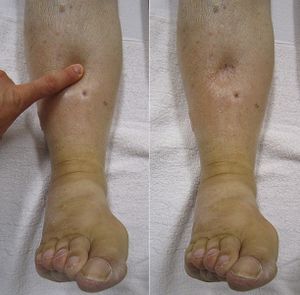
- Right-sided: peripheral edema, JVD, hepatomegaly
- Most common cause is left-sided failure
NYHA Classes
- No symptoms
- Symptoms with every day activity
- Severely limits activity or symptoms with minimal activity
- Symptoms at rest
Etiology
- Acute coronary syndrome (CAD)
- Hypertension
- Cardiomyopathy
- Valvular emergency
- High-output heart failure
- Peripartum cardiomyopathy
- Cardiac tamponade
- Dysrhythmias
Clinical Features
History & Physical Examination[1]
Different types of presentations:
- Hypotensive Heart Failure (cardiogenic shock)
- Least common, worst prognosis
- shortness of breath, pulmonary edema, narrow pulse pressure, signs of poor end-organ perfusion, altered mental status, cool peripheries, decreased urine output, increased HR, sBP < 90 mmHg
- Normotensive Heart Failure
- Develops over days to weeks
- Weight gain, peripheral edema, less shortness of breath, +/- rales
- Hypertensive Heart Failure
- Most common, presses rapidly
- sBP > 140 mmHg, preserved LV function, marked shortness of breath, minimal weight gain, rales, increased HR, pulmonary edema on CXR
- Acute (Flash) Pulmonary Edema
- Severe respiratory distress, relative hypertension, cool dipahoretic skin, +/- rales, JVD (94% specific, 39% sensitive), +/- peripheral edema, S3 (99% specific)
Differential Diagnosis
Congestive heart failure
- Cardiovascular
- Pulmonary
- Other
- Pure volume overload
- Renal failure
- Post-Transfusion
- Sepsis
- Anaphylaxis
- Pure volume overload
Causes of CHF Decompensation
- Medication noncompliance
- Dietary noncompliance
- Uncontrolled hypertension
- MI
- Valvular Dysfunction
- Arrhythmias
- Infection
- Inappropriate medications (e.g., negative inotropes)
- Fluid overload
- Missed dialysis
- Thyrotoxicosis
- Anemia
- Alcohol Withdrawal or alcohol intoxication
- Sympathomimetic excess
- Acute hypoxia or other respiratory problems
- Myocarditis
- Pulmonary embolism
- Excessive exertion or trauma
Elevated BNP
- CHF/ACS/Cardiogenic shock
- Pulmonary embolism
- Pulmonary hypertension
- Renal failure
- Left ventricular hypertrophy
- Sepsis[2]
- Subarachnoid hemorrhage
- Liver cirrhosis[3]
Evaluation
- CBC (rule out anemia)
- Chemistry
- ECG
- Digoxin level
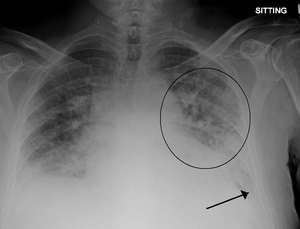
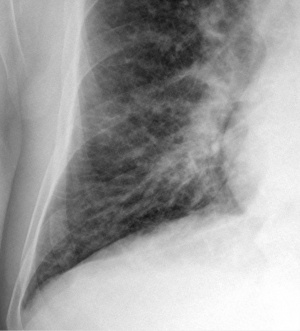
- CXR
- Cephalization
- Kerley B lines (thick and horizontal)
- Interstitial edema
- Pulmonary venous congestion
- Pleural effusion
- Alveolar edema
- Cardiomegaly
- Troponin/CK
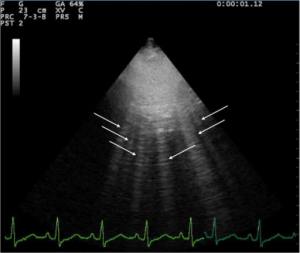
- Ultrasound
- Bedside to assess global function, B lines, assessment of IVC
- Formal TTE/TEE
Brain natriuretic peptide (BNP)[4]
- Measurement
- <100 pg/mL: Negative for acute CHF (Sn 90%, NPV 89%)
- 100-500 pg/mL: Indeterminate (Consider differential diagnosis and pre-test probability)
- >500 pg/mL: Positive for acute CHF (Sp 87%, PPV 90%)
- Combination of BNP with clinician judgment 94% sensitive 70% specific (compared to 49% sn and 96% spec clinical judgement alone) [5]
NT-proBNP[6][7][8]
- <300 pg/mL → CHF unlikely
- CHF likely in:
- >450 pg/mL in age < 50 years old
- >900 pg/mL in 50-75 years old
- >1800 pg/mL in > 75 years old
Lung ultrasound of pulmonary edema
- A lines and B lines
- A lines:
- Appear as horizontal lines
- Indicate dry interlobular septa.
- Predominance of A lines has 90% sensitivity, 67% specificity for pulmonary artery wedge pressure <= 13mm Hg
- A line predominance suggests that intravenous fluids may be safely given without concern for pulmonary edema
- B lines ("comets"):
- White lines from the pleura to the bottom of the screen
- Highly sensitive for pulmonary edema, but can be present at low wedge pressures
- A lines:
Management
Acute Pulmonary Edema and Hypertensive Heart Failure
See Pulmonary Edema or Sympathetic crashing acute pulmonary edema (SCAPE)
Hypotensive Heart Failure
Inotropic Agents
- Dobutamine generally first line
- Milrinone if patient on beta-blockers
- Consider in severe LV dysfunction and low output syndrome
- Diminished peripheral perfusion and end organ damage
- Vasodilatory treatment inadequate response or limited by symptomatic hypotension
- Must have obvious evidence of elevated filling pressures
- JVD, noncollapsing IVC, etc
- Inotropes are not indicated in setting of preserved systolic function
Heart Failure Without Pulmonary Edema
UNLOAD+
- Upright Position
- Nitrates
- Do not use with sildenafil, severe AS, or if right-sided MI
- Start sublingual nitroglycerin 0.4mg delivered over 4 min = 0.10mg/min
- If no improvement IV nitroglycerin drip, start 0.3-0.5mcg/kg/min, but may increase to 3-5mcg/kg/min
- Keep BP >95
- Consider nitroprusside 0.3 mcg/kg/min if hypertension or nitroglycerin ineffective
- Lasix
- Hold if no symptoms of fluid overload
- Give nitrates first
- Give double home dose, or up to 2.5x dose.
- If lasix 40mg po QD, then lasix 40-100mg IV
- Oxygen
- ACEI
- Afterload reduction
- Enalaprilat at 0.004mg/kg as IVB or 1mg drip over 2hr
- Avoid in pregnancy, hyperK+, angioedema
- Digoxin
- Decompensated HF
- Digoxin and Amiodarone are the only medications indicated for use in decompensated HF for rate control if needed[9]
- Evidence suggests that treating rate in acutely ill patients including CHF leads to worse outcomes[10]
- Compensated HF (not acutely symptomatic from failure)
- May benefit from a fib rate control, but calcium-channel blockers and beta-blockers first line, goal of < 85 bpm per RACE II trial
- Diltiazem low and slow at 5mg/hr
- AVOID in severe heart failure, preexcitation syndrome
- AVOID in significant hypotension
- Metoprolol 2.5 - 5.0mg over 2 min, then q5 as needed to max of 15mg
- Esmolol 0.5mg/kg bolus over 1 min, then 50 mcg/kg/min, may increase q30 min by 50 mcg/kg/min
- Decompensated HF
Medications to Avoid
- Anti-dysrhythmics other than digoxin and amiodarone
- Calcium-channel blockers - worsen HF
- NSAIDs - sodium retention, worsen toxicity of diuretics and ACE-I
- Thiazolidinediones - worsen HF
- Morphine - chart reviews show increased morbidity in ADHF patients[11][12]
Disposition
Admission Criteria
CCORT - Emergent Heart Failure Mortality Risk Grade Calculator
- 7 day mortality risk score calculator for patients presenting to the ED with decompensated HF
- https://ehmrg.ices.on.ca
AHCPR '00
- ACS
- Pulmonary edema/respiratory distress
- O2 sat < 90% on room air
- Severe complicating illness
- CHF refractory to outpatient therapy
- Anasarca
- Symptomatic hypotension or syncope
- Arrhythmia (e.g. new a. fib)
- Inadequate outpatient support
CHF Drug Target Doses
- ACE inhibitor
- Lisinopril 5mg QD start; 20mg QD goal
- Captopril 25mg tid start; 100mg tid goal
- Benazepril 10mg QD start; 40mg QD goal
- ARB
- Beta-blocker
- Carvedilol 3.125mg BID start; 25mg BID goal (50mg BID goal if weight > 85 kg)
- Metoprolol ER 12.5mg QD start; 190mg QD goal
- Others
- Hydralazine/isosorbid dinitrate 10-20mg (1 tab) tid start; 100-80mg (5 tabs) goal for black patients with NYHA III-IV already on BB and ACEi
- Spironolactone 25mg QD start; 50mg QD goal for indications:
- LVEF < 30% with NYHA II
- LVEF < 35% with NYHA III-IV
- LVEF < 40% post-MI, goal ACE-I, symptomatic CHF, or DM
See Also
External Links
- MDCalc - Emergency Heart Failure Mortality Risk Grade (EHMRG)
- emDocs - ED Management of Heart Failure: Pearls and Pitfalls
References
- ↑ Peacock W. Chapter 57: Congestive Heart Failure and Acute Pulmonary Edema. In: Tintinalli J. Tintinalli's Emergency Medicine. A comprehensive study guide. 7th ed. 2011: 405-415.
- ↑ Nikolaos I. Nikolaou, Constantin Goritsas, Maria Dede, Nikolaos P. Paissios, Michalis Papavasileiou, Amalia T. Rombola, Angeliki Ferti, Brain natriuretic peptide increases in septic patients without severe sepsis or shock, European Journal of Internal Medicine, Volume 18, Issue 7, 2007, Pages 535-541, ISSN 0953-6205, https://doi.org/10.1016/j.ejim.2007.01.006.
- ↑ Radvan M, Svoboda P, Radvanová J, Stumar J, Scheer P. Brain natriuretic peptide in decompensation of liver cirrhosis in non-cardiac patients. Hepatogastroenterology. 2009;56(89):181-185.
- ↑ Maisel AS, Krishnaswamy P, Nowak RM, et al. Rapid measurement of B-type natriuretic peptide in the emergency diagnosis of heart failure. N Engl J Med. 2002;347(3):161-167. doi:10.1056/NEJMoa020233.
- ↑ McCullough et al. B-Type natriuretic peptide and clinical judgment in emergency diagnosis of heart failure: analysis from breathing not properly (BNP) multinational study. Circulation. 2002:DOI: 10.1161/01.CIR.0000025242.79963.4
- ↑ Januzzi JL, van Kimmenade R, Lainchbury J, et al. NT-proBNP testing for diagnosis and short-term prognosis in acute destabilized heart failure: an international pooled analysis of 1256 patients: the International Collaborative of NT-proBNP Study. Eur Heart J. 2006 Feb. 27(3):330-7.
- ↑ Kragelund C, Gronning B, Kober L, Hildebrandt P, Steffensen R. N-terminal pro-B-type natriuretic peptide and long-term mortality in stable coronary heart disease. N Engl J Med. 2005 Feb 17. 352(7):666-75.
- ↑ Moe GW, Howlett J, Januzzi JL, Zowall H,. N-terminal pro-B-type natriuretic peptide testing improves the management of patients with suspected acute heart failure: primary results of the Canadian prospective randomized multicenter IMPROVE-CHF study. Circulation. 2007 Jun 19. 115(24):3103-10.
- ↑ January CT, et al. 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: Executive summary a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol. 2014; 64(21):2246-2280.
- ↑ Scheuermeyer FX, et al. Emergency department patients with atrial fibrillation or flutter and an acute underlying medical illness may not benefit from attempts to control rate or rhythm. Ann Emerg Med. 2015; 65(5):511-522.e2.
- ↑ Peacock WF, Hollander JE, Diercks DB, Lopatin M, Fonarow G, Emerman CL. Morphine and outcomes in acute decompensated heart failure: an ADHERE analysis. Emerg Med J. 2008 Apr;25(4):205-9.
- ↑ Ellingsrud C, Agewall S. Morphine in the treatment of acute pulmonary oedema--Why? Int J Cardiol. 2016 Jan 1;202:870-3.