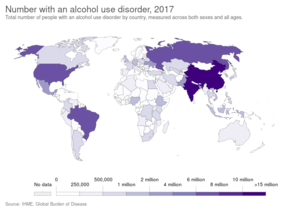
Alcohol use disorder
Background
- Chronic mental illness characterized by inability to limit alcohol ingestion, compulsive drinking, and a negative emotional state when not drinking.
- Previously separated into alcohol abuse and alcohol dependence, but as of DSM-5, the diagnoses were combined into alcohol use disorder, and subdivided into mild, moderate, or severe.
- It is estimated that about 6% of adults in the US suffer from alcohol use disorder.
Clinical Features
- Drinking more or for a longer period of time than intended.
- Feeling incapable of cutting back on the amount of alcohol consumed.
- Becoming sick for an extended period of time as a result of drinking too much.
- Inability to concentrate due to alcohol cravings.
- Inability to care for a family, hold down a job, or perform in school.
- Continuing to drink despite problems caused with friends or family.
- Decreased participation in activities which were once important.
- Finding oneself in dangerous or harmful situations as a direct result of drinking.
- Continuing to drink despite adding to another health problem, feeling depressed or anxious or blacking out.
- Drinking more as a result of a tolerance to alcohol.
- Experiencing withdrawal symptoms.
- Mild = 2-3 features
- Moderate = 4-5 features
- Severe = 6 or more features
Differential Diagnosis
- Ethanol toxicity
- Alcohol use disorder
- Alcohol withdrawal
- Electrolyte/acid-base disorder
Evaluation
- A history alone is sufficient to make the diagnosis of alcohol use disorder, however, if a patient presents to the ER, it is important to evaluate for the presence of:
- Acute alcohol intoxication,
- Alcohol withdrawal, and
- Co-ingestion with other drugs or toxic alcohols
- Check electrolytes, including magnesium and phosphorus[1]
- Long-term alcohol intake often has electrolyte abnormalities (including hypomagnesemia and hypokalemia)
- Low magnesium levels, typically below 0.8 mEq/L, can also cause hypocalcemia due to suppression of parathyroid hormone secretion and parathyroid hormone resistance
Management
Vitamin Prophylaxis for Chronic alcoholics
- At risk for thiamine deficiency, but no symptoms: thiamine 100mg PO q day
- Give multivitamin PO; patient at risk for other vitamin deficiencies
Banana bag
The majority of chronic alcoholics do NOT require a banana bag[2][3]
- Thiamine 100mg IV
- Folate 1mg IV (cheaper PO)
- Multivitamin 1 tab IV (cheaper PO)
- Magnesium sulfate 2mg IV
- Normal saline as needed for hydration
Medication Assisted Treatment
Naltrexone
Dosage
- Naltrexone 380 mg IM or 50 mg PO qday #30 tabs, no refills
- Contraindications:
- Any opioid use (including Buprenorphine):
- Must be off short-acting opioids for 1 week and methadone for 2 weeks
- Planned surgery/anesthesia in next 30 days (okay to use tablets, stop 1 day prior to surgery)
- Acute liver injury with AST or ALT >/= 250 or decompensated cirrhosis (Childs Pugh Class 3)
- Pregnancy
- Allergy
- Any opioid use (including Buprenorphine):
Evidence
- A Cochrane review assessed the efficacy of naltrexone in randomized control trials.[4]
- Helps to reduce the number of participants who relapse or return to heavy drinking in a short time frame following treatment (12 weeks).
- Reduces the time in days to first drink when compared to placebo or disulfiram.
- Reduces reported cravings and the total amount of alcohol consumed.
- Should be offered to patients with alcohol use disorder who are interested in reducing alcohol intake.
Gabapentin
Dosage
- Gabapentin 600 mg PO TID #90 tabs, no refills
- Counsel to decrease to 300 mg PO TID if dizzy, can increase after 1 week
- Renally dosed if CrCl<60
- ACOG approves of use in pregnancy
Evidence
- A metanalysis of several randomized control trials demonstrates that use of gabapentin for alcohol use disorder reduces the number of total heavy drinking days. [5]
- Addition of gabapentin to naltrexone further helped to reduce cravings in the first 6 weeks of AUD. [6]
Dilsulfiram
- Can be prescribed as alcohol avoidance therapy. This can be prescribed in the emergency department or referred to PCP/psychiatrist treating the patient's addiction.
Disposition
- Outpatient
- If the patient is not acutely intoxicated or at risk for alcohol withdrawal, they should be referred to a social worker or their PCP for resources to quit drinking and can usually be discharged safely.
See Also
External Links
References
- ↑ Baj J, Flieger W, Teresiński G, Buszewicz G, Sitarz R, Forma A, Karakuła K, Maciejewski R. Magnesium, Calcium, Potassium, Sodium, Phosphorus, Selenium, Zinc, and Chromium Levels in Alcohol Use Disorder: A Review. J Clin Med. 2020 Jun 18;9(6):1901. doi: 10.3390/jcm9061901. PMID: 32570709; PMCID: PMC7357092.
- ↑ Krishel, S, et al. Intravenous Vitamins for Alcoholics in the Emergency Department: A Review. The Journal of Emergency Medicine. 1998; 16(3):419–424.
- ↑ Li, SF, et al. Vitamin deficiencies in acutely intoxicated patients in the ED. The American Journal of Emergency Medicine. 2008; 26(7):792–795.
- ↑ Srisurapanont M, Jarusuraisin N. Opioid antagonists for alcohol dependence. Cochrane Database of Systematic Reviews. 2005;(1).
- ↑ Kranzler HR, Feinn R, Morris P, Hartwell EE. A meta-analysis of the efficacy of gabapentin for treating alcohol use disorder. Addiction. 2019;114(9):1547-1555.
- ↑ Anton RF, Myrick H, Wright TM, Latham PK, Baros AM, Waid LR, Randall PK. Gabapentin combined with naltrexone for the treatment of alcohol dependence. Am J Psychiatry. 2011 Jul;168(7):709-17. doi: 10.1176/appi.ajp.2011.10101436. Epub 2011 Mar 31. PMID: 21454917; PMCID: PMC3204582.