Ebola virus disease
Background
- An RNA based virus from the Filovirus Family with 5 species mainly originating from Africa.
- Outbreaks in Gabon, Africa occured in 1996 and in July, 2014[1]
- Viral hemorrhagic fever
- Unknown reservoir with most likely being bats
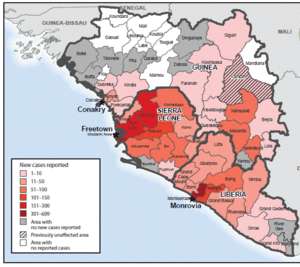
2014 Outbreak Country Details[2]
- Widespread Transmission
- Guinea
- Liberia
- Sierra Leone
- Localized Transmission^
- United States
- Mali
- Previously Affected*
- Nigeria
- Senegal
- Spain
^Persons traveling from these countries should NOT be considered to be at risk for exposure to Ebola.
2014 Domestic Outbreak Details
- September 30, 2014
- First case diagnosed in the United States in a man who had traveled to Dallas, Texas from Liberia (Died)
- October 10, 2014
- Healthcare worker at Texas Presbyterian Hospital who provided care for the index patient tested positive. (Recovered)
- October 15, 2014
- A second healthcare worker who provided care for the index patient tested positive (Recovered)
- October 23, 2014
- Medical aid worker who had returned to New York City from Guinea tested positive. (recovered)
- Current to date
- All other 177 contacts of the index case, all people on the plane with the second healthcare worker, all contacts of the NY case, everyone else who has come from West Africa = NO CASES
Communicable Transmission
- Via blood and body fluids (urine, saliva, semen, feces, vomit) in contact with mucous membranes or via instruments such as needles[3]
Clinical Features[4]
- Severe, often fatal (40-65%) hemorrhagic fever
- Incubation period: 2-21 days (most commonly ~11 days)
- Patients under the age of 21 years have alower case fatality rate than those over the age of 45 years (57% vs. 94%)[5]
- Common symptoms:
- fever (87.1%)
- fatigue (76.4%)
- Loss of appetite (64.5%)
- vomiting (67.6%)
- diarrhea (65.6%)
- headache (53.4%)
- abdominal pain (44.3%)
- Hemorrhagic symptoms (<43%)
Differential Diagnosis
Fever in traveler
- Normal causes of acute fever!
- Malaria
- Dengue
- Leptospirosis
- Typhoid fever
- Typhus
- Viral hemorrhagic fevers
- Chikungunya
- Yellow fever
- Rift valley fever
- Q fever
- Amebiasis
- Zika virus
Evaluation
For travelers returning from countries with active Ebola follow the CDC Algorithm for Evaluation of the Returned Traveler
Persons under Investigation (PUI)
- Obtain a travel history for all persons presenting with fever
- Consider Ebola in any person who presents within 21 days of:
- Traveling to an area with widespread transmission (see background section), OR
- Had contact with a person who had a confirmed Ebola case
Management[6]
Transmission Precautions
- Isolate the patient
- single patient room (with private bathroom), door closed
- Wear appropriate PPE
- Enhanced standard, contact, and droplet isolation precautions[7]
- gloves, gown (fluid resistant or impermeable), eye protection, and a facemask.
- Additional protective equipment might be required in certain situations: double gloving, disposable shoe covers, and leg coverings
- Have a second party monitor
- Restrict visitors
- Avoid entry of visitors into the patient's room
- Keep a logbook of all persons entering the patient's room
- Avoid aerosol-generating procedures
- If necessary, use respiratory protection (N95 or higher) and perform in airborne isolation room
- Implement environmental infection control measures
- Diligent environmental cleaning and disinfection
Contact Public Health
- Immediately report PUIs to local health authorities or CDC
- Los Angeles repots to Acute Communicable Disease Control Program (ACDC) at 213-240-7941 (nights/weekends: 213-974-1234)
- Special diagnostic testing requires consultation
Clinical Care
- Test and treat for other possible causes of Fever in Travelers while evaluating for Ebola
- A few days after infectious symptoms begin, ELISA IgM, PCR or virus isolation are possible. Later in the disease or during recovery, IgM or IgG can be tested.
- CDC has guidance for safe specimen handling
- Use point-of-care testing as much as possible
- Supportive care
Disposition
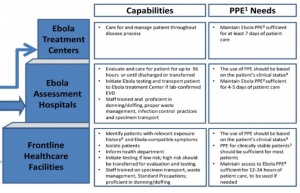
- Frontline Healthcare Facilities
- In consultation with public health authorities:
- Low risk: May initiate testing
- High risk: Transfer to Ebola Assessment Hospital or Ebola Treatment Center (if locally available)
- In consultation with public health authorities:
- Ebola Assessment Hospitals
- In consultation with public health authorities:
- Initiate initial testing
- If confirmed case, transfer to Ebola Treatment Center[8]
- In consultation with public health authorities:
- Ebola Treatment Center
- Admit, isolation, possible ICU for serologic results and clinical observation/supportive care.
See Also
External Links
- CDC Main Site: http://www.cdc.gov/vhf/ebola/index.html
- PPE video: http://www.medscape.com/viewarticle/833907?src=ppc_google_acq_bola_vid
References
- ↑ Ebola Virus Disease, West Africa http://www.afro.who.int/en/clusters-a-programmes/dpc/epidemic-a-pandemic-alert-and-response/outbreak-news/4233-ebola-virus-disease-west-africa-25-july-2014.html.
- ↑ CDC Website, accessed 12/10/2014
- ↑ Peters CJ. Chapter 197. Ebola and Marburg Viruses. Harrison’s Principles of Internal Medicine, 18e. 2012
- ↑ Ebola Virus Disease in West Africa — The First 9 Months of the Epidemic and Forward Projections. N Engl J Med 2014;371:1481-95
- ↑ Schieffelin JS, Shaffer JG, Goba A, et al. Clinical Illness and Outcomes in Patients with Ebola in Sierra Leone. N Engl J Med. 2014 Oct 29. PMID 25353969
- ↑ CDC website, accessed 12/10/14
- ↑ http://www.cdc.gov/vhf/ebola/hcp/infection-prevention-and-control-recommendations.html
- ↑ http://www.cdc.gov/vhf/ebola/hcp/current-treatment-centers.html