Diffuse abdominal pain
Background
- Diffuse (generalized) abdominal pain suggests a process affecting multiple quadrants or a non-localizing etiology
- Key EM concern: diffuse pain with peritoneal signs suggests perforation, mesenteric ischemia, or diffuse peritonitis — all surgical emergencies
- Diffuse pain may also represent early appendicitis (before localizing to RLQ), early small bowel obstruction, or extra-abdominal causes
- Consider metabolic and extra-abdominal sources (DKA, uremia, adrenal crisis)
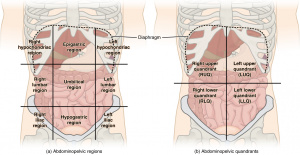
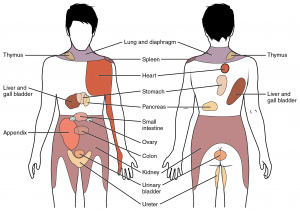
Classification by Abdominal pain location
| RUQ pain | Epigastric pain | LUQ pain |
| Flank pain | Diffuse abdominal pain | Flank pain |
| RLQ pain | Pelvic pain | LLQ pain |
Clinical Features
History
- Onset, character, duration, progression
- Associated symptoms: nausea/vomiting, diarrhea/constipation, fever, last bowel movement/flatus
- Prior abdominal surgeries (adhesive small bowel obstruction)
- Medications: NSAIDs, anticoagulants, immunosuppressants
- Medical history: diabetes (DKA), atrial fibrillation (mesenteric ischemia), vascular disease
- Social history: alcohol use, recent travel
Physical Exam
- Assess for peritoneal signs: rigidity, rebound tenderness, guarding, involuntary guarding
- Abdominal distension (obstruction, ileus, ascites)
- Bowel sounds: absent (ileus, late obstruction), high-pitched/tinkling (early obstruction)
- Hernial orifices (incarcerated hernia)
- Rectal exam: occult blood, rectal mass
- Skin: jaundice, rash (vasculitis), livedo reticularis
Red Flags
- Hemodynamic instability
- Rigid abdomen (peritonitis — surgical emergency)
- Diffuse pain out of proportion to exam (mesenteric ischemia — "pain out of proportion")
- Free air on imaging (perforation)
- Metabolic acidosis with diffuse pain (ischemia, DKA, toxic ingestion)
- Immunocompromised patient with abdominal pain (broad differential, atypical presentations)
Differential Diagnosis
Diffuse Abdominal pain
- Abdominal aortic aneurysm
- Acute gastroenteritis
- Aortoenteric fisulta
- Appendicitis (early)
- Bowel obstruction
- Bowel perforation
- Diabetic ketoacidosis
- Gastroparesis
- Hernia
- Hypercalcemia
- Inflammatory bowel disease
- Mesenteric ischemia
- Pancreatitis
- Peritonitis
- Sickle cell crisis
- Spontaneous bacterial peritonitis
- Volvulus
Extra-abdominal Sources of Abdominal pain
- MI
- Aortic Dissection
- PNA
- PE
- Testicular Torsion
- Herpes Zoster
- Muscle spasm
- Spinal pathology
- Strep Pharyngitis (peds)
- Mononucleosis
- DKA
- ETOH Ketoacidosis
- Uremia
- Sickle Cell Crisis
- SLE
- Vasculitis
- Glaucoma
- Hyperthyroidism
- Methanol Poisoning
- Heavy Metal toxicity
- Addison's disease
- Porphyria
- Paroxysmal nocturnal hemoglobinuria
- Black widow spider bite
Must Not Miss
- Mesenteric ischemia: elderly, atrial fibrillation, pain out of proportion to exam
- Perforated viscus: free air, peritonitis
- Small bowel obstruction: vomiting, distension, prior surgery
- Ruptured AAA: elderly, hypotensive, pulsatile abdominal mass
- Diabetic ketoacidosis: may present with severe abdominal pain as chief complaint
Evaluation
Laboratory
- CBC, BMP
- LFTs, lipase
- Urinalysis
- Urine pregnancy test (females of reproductive age)
- Lactate: elevated in mesenteric ischemia, sepsis, shock
- ECG: rule out MI in older patients (can present as epigastric/diffuse abdominal pain)
- Blood gas: metabolic acidosis (ischemia, DKA, toxic ingestion)
- Lipase: pancreatitis
- Blood cultures if febrile
- Stool guaiac
Imaging
- CT abdomen pelvis with IV contrast: most useful single test for diffuse abdominal pain (identifies obstruction, perforation, ischemia, abscess, appendicitis)
- Upright CXR or abdominal X-ray: free air under diaphragm (perforation), air-fluid levels (obstruction)
- POCUS: free fluid, AAA, hydronephrosis, gallbladder
- CT angiography: if mesenteric ischemia suspected
- KUB (abdominal X-ray): obstruction pattern, foreign body
Management
- IV access, fluid resuscitation
- Analgesia: appropriate pain control does NOT mask important findings and should not be withheld — opioids may actually improve physical exam by allowing patient to cooperate
- NPO if surgical abdomen suspected
- NG tube for decompression in obstruction with vomiting
- Emergent surgical consultation for: peritonitis, free air, suspected mesenteric ischemia, ruptured AAA, SBO with signs of strangulation
- Broad-spectrum IV antibiotics if perforation, peritonitis, or intra-abdominal sepsis suspected
- Treat metabolic cause (DKA, adrenal crisis) if identified
Disposition
- Admit: peritonitis, bowel obstruction, mesenteric ischemia, perforation, intra-abdominal abscess, pancreatitis requiring IV management, GI bleeding with hemodynamic changes
- Observation: undifferentiated abdominal pain with concerning features but negative initial workup — serial exams
- Discharge: benign etiology identified, pain resolving, tolerating oral intake, reliable follow-up in 24-48 hours
- Return precautions: worsening pain, vomiting, fever, inability to eat/drink, blood in stool