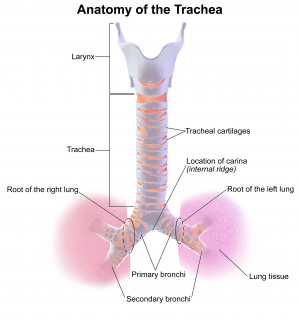
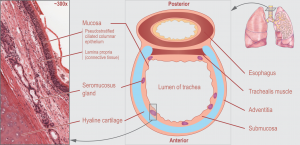
Bacterial tracheitis
Background
- Bacterial infection of tracheal epithelium
- Often secondary infection after viral illness
- S. Aureus most common, also strep species, H. Influenza and anaerobes
- Peak age is 3-5 years old
- Occurs throughout childhood and adulthood
Clinical Features
- Severely ill child, starts out as viral prodrome
- Followed by inspiratory and expiratory stridor, respiratory distress, and copious purulent secretions
- Difficult to differentiate from croup and epiglottitis
- May have been treated with racemic epinephrine and steroids for croup, with no clinical improvement
Differential Diagnosis
Pediatric stridor
<6 Months Old
- Laryngotracheomalacia
- Accounts for 60%
- Usually exacerbated by viral URI
- Diagnosed with flexible fiberoptic laryngoscopy
- Vocal cord paralysis
- Stridor associated with feeding problems, hoarse voice, weak and/or changing cry
- May have cyanosis or apnea if bilateral (less common)
- Subglottic stenosis
- Congenital vs secondary to prolonged intubation in premies
- Airway hemangioma
- Usually regresses by age 5
- Associated with skin hemangiomas in beard distribution
- Vascular ring/sling
>6 Months Old
- Croup
- viral laryngotracheobronchitis
- 6 mo - 3 yr, peaks at 2 yrs
- Most severe on 3rd-4th day of illness
- Steeple sign not reliable- diagnose clinically
- Epiglottitis
- H flu type B
- Have higher suspicion in unvaccinated children
- Rapid onset sore throat, fever, drooling
- Difficult airway- call anesthesia/ ENT early
- H flu type B
- Bacterial tracheitis
- Rare but causes life-threatening obstruction
- Symptoms of croup + toxic-appearing = bacterial tracheitis
- Foreign body (sudden onset)
- Marked variation in quality or pattern of stridor
- Retropharyngeal abscess
- Fever, neck pain, dysphagia, muffled voice, drooling, neck stiffness/torticollis/extension
Evaluation
- Clinical diagnosis
- Gram stain with predominance of one organism, differentiating from colonization
- XR neck may show subglottic narrowing with ragged tracheal epithelium
- CXR may show concomitant pneumonia
- Emergent bronchoscopy is diagnostic and therapeutic
Management
- Intubation, emergent, usually necessary
- Bronchoscopy to confirm diagnosis, rule out supraglottic pathology
- Antibiotics[1]
- Third generation cephalosporin (cefotaxime or ceftriaxone)
- PLUS MRSA coverage, options below depending on prevalence of CA-MRSA
- Clindamycin 40mg/kg/d IV divided q8hr OR
- Vancomycin 45mg/kg/d IV divided q8hr
Disposition
- Admit to ICU
- Often require prolonged intubation (4-5 days)
Complications
- Toxic shock syndrome
- Septic shock
- Renal failure
- Postintubation pulmonary edema
- ARDS
- Residual subglottic stenosis
See Also
External Links
References
- ↑ Bacterial Tracheitis - Treatment and Management. Medscape. http://emedicine.medscape.com/article/961647-treatment