Nonaccidental trauma
(Redirected from Abuse (Nonaccidental Trauma))
Background
- Newer term that encompasses child abuse
- Infant and children with disabilities are at higher risk
- In >80% of cases, the parent or primary guardian is the abuser
- Report suspicion
- Transparent, frank discussion with caregivers
- Social work or child protection agency involvement
- Protect the child first, admit if suspicious
- Social work may follow-up as outpatient for very low risk cases
Risk Factors
- Domestic violence
- Maternal depression
- Drug and alcohol abuse
- Premature birth
- Children with disabilities or children who require significant medical care
- Unrealistic expectations for the child
Red flags
- History given is inconsistent with the mechanism of injury
- Changes in caregivers report
- Significant delays in care
- Any injury to a young, pre-ambulatory infant
- Injuries to multiple organ systems
- Injuries in different stages of healing;
- Patterned injuries
- Injuries to non-bony or other unusual locations, (torso, ears, face, neck, or upper arms)
- Significant injuries that are unexplained
- Other evidence of child neglect.
Clinical Features
Bruises
- Bruises, ecchymosis, and soft-tissue injuries on the face, cheeks, buttocks, ears, torso, neck if the child is not cruising yet
- Bruises in clusters or patterned marks
- Bruising of any child less than or equal to 6 months of age (or non-ambulatory) warrants a full child abuse work-up
Oral injuries
- Torn frenulum in premobile children is highly associated with physical abuse
- Other reported oral injuries include laceration/bruising to the lips, mucosal lacerations, dental trauma, tongue injuries, and gingival lesions
Burns
- Most commonly immersion injuries of the extremities, buttocks, or perineum
- More likely symmetrical with clear upper margins
- Many will also have occult fractures; children <24mo should undergo a skeletal survey
Fractures
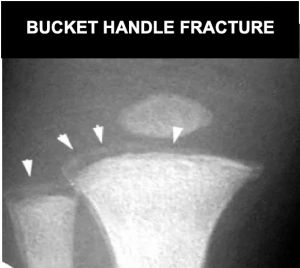
Bucket Handle Fracture (Courtesy of Michael Mojica[1])
- Fractures highly suspicious of abuse:
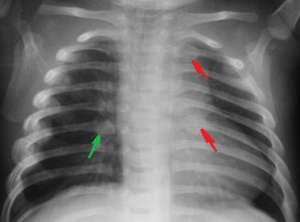
- Rib fracture, especially posterior
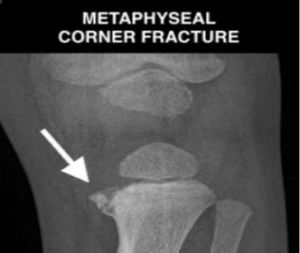
- Metaphyseal or Corner Fracture (Bucket Handle)
- Scapula fracture
- Spinous process fractures
- Sternum fracture
- Fracture not consistent with developmental stage (any fracture in non-ambulatory child)
- Fractures moderately suspicious of abuse:
- Long-bone transverse or spiral fracture of the diaphysis of the femur, humerus, tibia
- Multiple bilateral fractures
- Different stages of healing with multiple fractures
- Epiphyseal separations
- Vertebral body separation
- Complex skull fractures (i.e. depressed or cross suture lines)
- Pelvic fractures
Head Trauma
- Leading cause of death in abused children <2 years old
- Shaken baby syndrome - Retinal hemorrhages
- Present in up to 75% of cases and are virtually pathognomonic
- Described as “dot and blot” hemorrhages or flame or splinter hemorrhages
Abdominal Trauma
- Most from a direct blow or from being thrown
- Any abrasion or bruise on the abdominal area should prompt an evaluation for possible trauma
- Consider abuse in preschool aged children with any hollow viscus or pancreatic injury
Sexual Trauma
- Even among children who report vaginal or anal penetration, the rate of abnormal physical examination findings is only 5 to 15%
- Consult your local sexual assault response team or transfer to an appropriate facility as indicated.
- Females
- Preferred positioning for adequate examination: child lying supine with her hips externally rotated and knees flexed (frog-leg) or the prone knee-chest position.
- Examine hymen for lacerations, transections, and bruising.
- Prepubertal females do not require a speculum exam unless there is active bleeding.
- Vaginal discharge in a prepubertal female should prompt testing for sexually transmitted infections.
- The diameter of the hymenal orifice is not a marker for whether or not vaginal penetration occurred.
- Males
- Examine for lacerations, burns, bite marks, and bruises to the genital region. Penile and anal injuries are more common than scrotal injuries.
- Swab any anal or penile discharge for sexually transmitted infections.
Differential Diagnosis
- Bruising
- Mongolian spots (congenital dermal melanosis)
- Bleeding disorders
- Hemangiomas
- Phytophotodermatitis
- Malignancy
- Connective tissue disease
- Cultural healing practices (eg, coining and cupping)
- Osteogenesis imperfecta
- Vasculitis (Henoch-Schönlein purpura)
- Ink stains (e.g. caused by new clothing)
- Burns
- Hypersensitivity reaction
- Friction blisters
- Impetigo (may be confused with cigarette burns)
- Phytophotodermatitis
- Dermatitis herpetiformis
- Accidental laxative ingestion
- Healing practices (eg, coining, cupping, and moxibustion)
- Fractures
- Rickets
- Congenital syphilis (can cause periosteal elevation)
- Birth trauma
- CPR (rarely causes rib fractures and very rarely causes posterior rib fractures)
- Osteogenesis imperfecta
- Caffey disease
- Osteomyelitis
- Subdural hematoma
- Bleeding disorders
- Vascular malformations
- Glutaric aciduria type 153
- Benign extra-axial fluid
- Menkes disease
- Retinal hemorrhage
- Vasculitis
- Vascular obstruction
- Vaginal delivery (generally disappear by 4 weeks of age)
- CPR (retinal hemorrhages are rare after chest compressions and, if present, are usually in the presence of other risk factors for hemorrhage)
Crying Infant
- Occult infection
- GI
- Intussusception
- GERD
- Incarcerated hernia
- Milk protein intolerance
- Anal fissure
- Ophtho
- Occult trauma
- Hair tourniquet (on extremities, penis)
- Non-accidental trauma
- Diaper pin
- Insect bites
- Burns in mouth
- Misc
- Colic
- Scorpion envenomation
- SVT
- Testicular torsion
- Drug exposure/overdose (commonly methamphetamine or cocaine)
- Neonatal abstinence syndrome, drug withdrawal
Psychosocial and Related
- Drugs of abuse
- Elder abuse
- Human trafficking
- Homelessness
- Interpersonal Violence
- Mandatory reporting
- Nonaccidental trauma
- Sexual assault
Evaluation
- Skeletal survey for all children < 2 years of age, non-verbal, or severe developmental delay. Note: Follow-up skeletal survey should be performed within 10 to 14 days
- Skull AP and lateral view (left and right)
- Chest AP and lateral view
- Right and left oblique of the chest
- AP of the abdomen to include pelvis and hips
- AP and lateral spine to include cervical, thoracic, and lumbar vertebrae
- AP bilateral humerus
- AP bilateral forearms
- AP bilateral femurs
- AP bilateral tibia and fibula
- Posterior view of the hands
- Dorsoplantar view of the feet
- Head CT without contrast for any child < 1 year with suspicion of abuse or >1 year with concerning signs of head trauma
- Trauma labs: CBC, CMP, PT, PTT, lipase, and urinalysis (looking for blood; use bag specimen). Consider urine tox screen
- Consider CPK and platelet function studies if extensive bruising is present
- If trauma labs are abnormal (AST or ALT > 80, lipase > 100), obtain a CT of abdomen/pelvis with IV contrast
- Consider a dilated fundoscopic exam if under 2 years
- Photograph injuries
- Obtain a social work consult
Inpatient Workup[2]
- Ophtho consult for retinal hemorrhages
- CBC
- CMP, Mg, phos
- PT/INR/aPTT, fibrinogen
- PTH, iCa, 25-hydroxy-Vit D, 1,25-dihydroxy-Vit D
- vW panel (vW AT, ristocetin cofactors, factor VIII)
Management
- Treat injuries as indicated
- Keep alleged perpetrator separate from the patient if possible and/or keep patient supervised at all times
- Report abuse to the appropriate state child protection authority
Disposition
- Admit for medical treatment or if any question of child's safety
See Also
External Links
- Pediatric Emergency Playbook -- Vomiting in the Young Child: Nothing or Nightmare
- https://www.childhelp.org/wp-content/uploads/2019/02/CPS-Phone-Numbers-2.1.19.pdf
- Pediatric EM Morsels: Abuse