Stridor (peds)
This page is for pediatric patients. For adult patients, see: stridor
Background
- Stridor refers to harsh upper airway sounds caused by turbulent airflow through a narrowed airway[1]
- Classically inspiratory, indicating extrathoracic obstruction
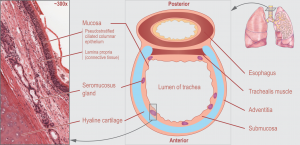
- Pediatric airways are particularly vulnerable due to anatomical differences:
- Smaller absolute airway diameter — 1mm of circumferential edema reduces cross-sectional area by ~60% in an infant vs. ~20% in an adult
- More compliant airway cartilage
- Relatively larger tongue and occiput
- Croup is the most common cause of acute stridor in children ages 6 months to 6 years[2]
- A minimal amount of edema or inflammation can result in significant obstruction and rapid decompensation
Clinical Features
Phase of Respiration
- Inspiratory stridor: extrathoracic obstruction (supraglottic/glottic)
- Pressuretrach < Pressureatm
- Croup, epiglottitis, foreign body, anaphylaxis, laryngomalacia
- Expiratory stridor (vs. wheezing): intrathoracic obstruction
- Pressuretrach < Pressurepleura
- Asthma, bronchiolitis, foreign body, vascular ring
- Biphasic stridor: fixed obstruction (subglottic stenosis, hemangioma, foreign body lodged at glottis)
By Age
- Neonates: laryngomalacia (most common cause of chronic stridor in infants), subglottic stenosis, vocal cord paralysis, congenital hemangioma, vascular ring
- Infants (6 months - 2 years): croup, foreign body, laryngomalacia, subglottic hemangioma
- Toddlers/Preschool (2-6 years): croup (most common), foreign body, epiglottitis, bacterial tracheitis
- School-age and older: epiglottitis, peritonsillar abscess, retropharyngeal abscess, foreign body
Red Flags (Impending Respiratory Failure)
- Drooling, inability to swallow
- Tripod positioning, refusal to lie down
- Toxic appearance, high fever (epiglottitis, bacterial tracheitis, retropharyngeal abscess)
- Cyanosis, altered mental status, decreasing stridor with worsening respiratory distress (exhaustion)
- No cough + drooling + high fever = think epiglottitis (do NOT examine throat or agitate child)
- Sudden onset without prodrome = think foreign body aspiration
Differential Diagnosis
Pediatric stridor
<6 Months Old
- Laryngotracheomalacia
- Accounts for 60%
- Usually exacerbated by viral URI
- Diagnosed with flexible fiberoptic laryngoscopy
- Vocal cord paralysis
- Stridor associated with feeding problems, hoarse voice, weak and/or changing cry
- May have cyanosis or apnea if bilateral (less common)
- Subglottic stenosis
- Congenital vs secondary to prolonged intubation in premies
- Airway hemangioma
- Usually regresses by age 5
- Associated with skin hemangiomas in beard distribution
- Vascular ring/sling
>6 Months Old
- Croup
- viral laryngotracheobronchitis
- 6 mo - 3 yr, peaks at 2 yrs
- Most severe on 3rd-4th day of illness
- Steeple sign not reliable- diagnose clinically
- Epiglottitis
- H flu type B
- Have higher suspicion in unvaccinated children
- Rapid onset sore throat, fever, drooling
- Difficult airway- call anesthesia/ ENT early
- H flu type B
- Bacterial tracheitis
- Rare but causes life-threatening obstruction
- Symptoms of croup + toxic-appearing = bacterial tracheitis
- Foreign body (sudden onset)
- Marked variation in quality or pattern of stridor
- Retropharyngeal abscess
- Fever, neck pain, dysphagia, muffled voice, drooling, neck stiffness/torticollis/extension
Evaluation
Immediate
- Assess airway stability — allow child to remain in position of comfort (parent's lap)
- Do NOT agitate the child if epiglottitis is suspected
- Pulse oximetry (may be normal until late)
- Observe work of breathing, air entry, level of consciousness
Stable Patient
- AP and lateral neck X-rays:
- Steeple sign (subglottic narrowing) = croup
- Thumbprint sign (swollen epiglottis) = epiglottitis
- Prevertebral soft tissue widening = retropharyngeal abscess
- Radiopaque foreign body
- CT neck with contrast if deep space infection, abscess, or mass suspected
- Direct visualization (nasopharyngoscopy / fiberoptic laryngoscopy) if available and safe
Unstable Patient
- Defer imaging — proceed directly to airway management
- Prepare for difficult airway — have smaller ETT sizes available, call for backup (anesthesia, ENT)
- See Intubation (peds) and Difficult Airway Algorithm
Laboratory
- Not routinely helpful in acute setting
- CBC, blood cultures if bacterial cause suspected (bacterial tracheitis, epiglottitis)
- Avoid phlebotomy in a distressed child with epiglottitis (agitation worsens obstruction)
Management
Croup (Most Common)
- Dexamethasone 0.6 mg/kg PO/IM (single dose, max 10mg) — cornerstone of treatment, effective even in mild croup
- Racemic epinephrine (2.25%) 0.5 mL nebulized in 3 mL NS for moderate-severe croup
- Or L-epinephrine (1:1000) 0.5 mL/kg nebulized (max 5 mL)
- Observe for 2-3 hours after racemic epinephrine (rebound possible)
- Humidified air/mist therapy: no proven benefit but commonly used
- Heliox for severe croup not responding to above
Epiglottitis
- Keep child calm, in parent's lap, in position of comfort
- Do NOT examine throat, do NOT lay child down, do NOT insert tongue depressor
- Call anesthesia and ENT immediately
- Controlled intubation in the operating room (preferred)
- If impending arrest: attempt intubation with experienced provider, prepare for surgical airway
- IV antibiotics after airway secured: ceftriaxone + vancomycin
Bacterial Tracheitis
- Intubation often required (thick tracheal secretions)
- IV antibiotics: ceftriaxone + vancomycin (or nafcillin)
- Frequent suctioning
Foreign Body
- If complete obstruction: BLS choking algorithm (back blows for infants, Heimlich for older children)
- If partial obstruction with stable airway: bronchoscopy for removal (do not attempt blind finger sweep)
- If unstable: attempt direct laryngoscopy for removal
Retropharyngeal/Peritonsillar Abscess
- IV antibiotics (ampicillin-sulbactam or clindamycin)
- ENT consultation for surgical drainage
- See Retropharyngeal abscess, Peritonsillar abscess
Anaphylaxis
- IM epinephrine (0.01 mg/kg, max 0.3-0.5 mg)
- See Anaphylaxis
Disposition
Admit / PICU
- Epiglottitis (PICU with secured airway)
- Bacterial tracheitis
- Severe croup not responding to treatment
- Required >1 dose of racemic epinephrine and still symptomatic
- Deep space neck infections
- Foreign body requiring bronchoscopy
- Respiratory failure or impending failure
Discharge
- Mild croup responding to dexamethasone with no stridor at rest after 2-3 hours observation
- Single dose of racemic epinephrine with resolution of symptoms after 2-3 hour observation period
- Reliable caregivers with access to return to ED
- Return precautions: worsening stridor, drooling, difficulty breathing, color change, inability to drink fluids, fever