Renal abscess
Background
- Rare clinical entity which can lead to delayed diagnosis
- Usually a complication of a UTI or pyelonephritis
- Most commonly due to E. Coli, Klebsiella, Proteus
- Less often can be due to hematogenous spread from other sources of infection
- Most commonly due to Staph aureus
Risk Factors
- Inadequately treated or delayed treatment of UTI or pyelonephritis
- Diabetes
- Renal calculi
- Ureteral obstruction
- Any underlying urinary tract abnormality
- Immunosuppression
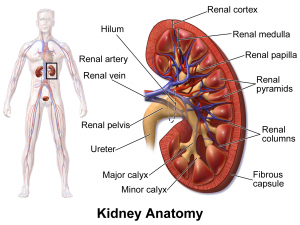
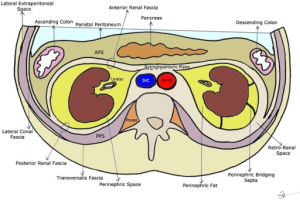
Perinephric vs renal abscess
| Perinephric | Renal | |
| Necrotic Area | Perinephric fat between the renal cortex and Gerota's fascia | Renal parenchyma |
| Cause | Pyelonephritis (majority) | Pyelonephritis (vast majority) |
| Risk of morbidity | Higher | Lower |
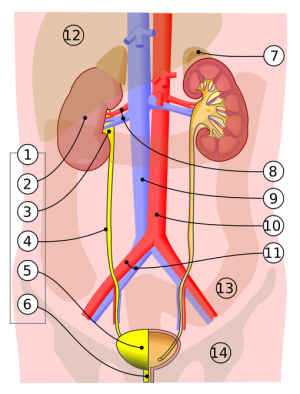
Genitourinary infection
"UTI" frequently refers specifically to acute cystitis, but may also be used as a general term for all urinary infections; use location-specific diagnosis.
- Renal/perirenal
- Ureteral
- Infected urolithiasis
- Bladder
- Acute cystitis ("UTI")
- Chronic cystitis
- Urethra/periurethra
Clinical Features
- Costovertebral, flank, lumbar, lower chest, or back pain
- Usually unilateral
- Fever, especially if prolonged or after antibiotic initiation
- Nausea, vomiting
- UTI or pyelonephritis symptoms not improving with antibiotics
Complications
- Need for open surgical management or nephrectomy
- Renal failure
- Sepsis, bacteremia
- Emphysematous kidney
- Cortical abscesses can rupture and form perinephric abscesses
Differential Diagnosis
Evaluation
.
- Labs
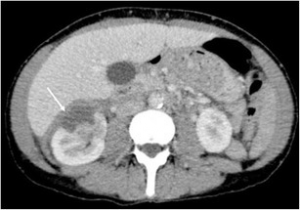
- Imaging
- Renal ultrasound
- Well-defined hypoechoic lesion with thick walls and usually with internal debris
- CT
- Renal ultrasound
Management
- Antibiotics
- Broad spectrum if unclear source
- If urinary source cover typical urinary pathogens
- Ceftriaxone 1g IV
- Piperacillin-Tazobactam 4.5 g IV
- If hematogenous spread considered, cover for MSSA and MRSA
- Vancomycin 15-20mg/kg IV
- If urinary source cover typical urinary pathogens
- Broad spectrum if unclear source
- Percutaneous drainage
- Open surgical management if patient fails antibiotics/percutaneous drainage
Disposition
- Admission for IV antibiotics and drainage
- Especially if elderly or elevated BUN or creatinine
References
- Dembry LM, Andriole VT. “Renal and Perirenal Abscesses” Infectious Disease Clinics North America: 11, 3, (Sept 1997).
- Getting GK, Shaikh N. “Renal Abscess” Journal of EM: 31, 1 (2006): 99-100.
- Judith E, Stapczynski J. Stephan. "Urinary Tract Infections” Tintinalli's Emergency Medicine: A Comprehensive Study Guide. 7th ed. New York: McGraw-Hill, 2011. 632.
- Yen DHT, et al. “Renal Abscess: Early Diagnosis and Treatment” Am J EM: 17, 2 (March 1999).
- Shu T, Green JM, Orihuela E. “Renal and Perirenal Abscesses in Patients with Otherwise Anatomically Normal Urinary Tracts” Journal of Urology: 172 (July 2004): 148-150.
- http://www.ncbi.nlm.nih.gov/pubmed/16798166