Psychogenic nonepileptic seizure
Background
- Psychogenic nonepileptic seizure (PNES) characterized disturbances of motor, sensory, autonomic, cognitive, and/or emotional functions that can mimic epileptic seizures.
- In contrast to epileptic seizures, PNES are not associated with abnormally excessive neuronal activity but are instead derived from psychologic causes.
- The term pseudoseizures and hysterical seizures are historical terms that are now discouraged.
- Accurate diagnosis is best achieved via a detailed history, physical examination, selected testing, and neurology and/or psychiatry evaluation.
- Epidemiology
- Estimated incidence rate ranges from 1.5 to 5 per 100,000 persons per year.
- Estimate prevalence 2 to 33 per 100,000 persons.
- More common in women
- Etiology
- There may be a history of sexual abuse, eating disorders, depression, substance abuse, anxiety disorders or personality disorders, and the episode may be preceded by a stressful event
- Dissociative disorders and conversion disorders are felt to be the underlying cause to most episodes of PNES.
- Some patients may have both psychogenic nonepileptic seizures and true epileptiform seizures
Clinical Features
- Symptoms specific to PNES:
- Duration > 2 minutes
- Pelvic thrusting
- Side to side head rocking
- Crying/shrieking
- Voluntary eye movements away from the examiner/forceful closing of the eyes
- Stuttering/stammering
- ABSENT postictal confusion
- ABSENT physical injury
- Symptoms similar to an epileptic seizure:
- Drooling
- Rapid eye movements
- Tongue biting
- Loss of bladder/bowel control
- Grunting
- Loss of consciousness
- Altered mental status
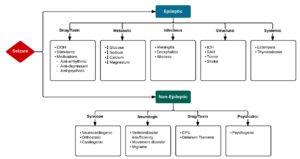
Differential Diagnosis
Seizure
- Epileptic seizure
- First-time seizure
- Seizure with known seizure disorder
- Status epilepticus
- Temporal lobe epilepsy
- Non-compliance with anti-epileptic medications
- Hyponatremia
- INH toxicity
- Non-epileptic seizure
- Meningitis
- Encephalitis
- Brain abscess
- Intracranial hemorrhage
- Alcohol withdrawal
- Benzodiazepine withdrawal
- Barbiturate withdrawal
- Baclofen withdrawal
- Metabolic abnormalities: hyponatremia, hypernatremia, hypocalcemia, hypomagnesemia, hypoglycemia, hyperglycemia, hepatic failure, uremia
- Eclampsia
- Neurocysticercosis
- Posterior reversible encephalopathy syndrome
- Impact seizure (head trauma)
- Acute hydrocephalus
- Arteriovenous malformation
- Seizure with VP shunt
- Toxic ingestion (amphetamines, anticholinergics, cocaine, INH, organophosphates, TCA, salicylates, lithium, phenothiazines, bupropion, camphor, clozapine, cyclosporine, fluoroquinolones, imipenem, lead, lidocaine, metronidazole, synthetic cannabinoids, theophylline, Starfruit)
- Psychogenic nonepileptic seizure (pseudoseizure)
- Intracranial mass
- Syncope
- Hyperventilation syndrome
- Migraine headache
- Movement disorders
- Narcolepsy/cataplexy
- Post-hypoxic myoclonus (Status myoclonicus)
Evaluation
- May be a clinical diagnosis
- Consider standard seizure workup
- Always check glucose
- Lactic acid may be able to differentiate from true generalized tonic-clonic seizure[1]
- Consider obtaining a drug screen (and a pregnancy test in women)
- If unsure, an urgent neuro consult with EEG can determine the diagnosis
Management
- Avoid invasive medical procedures
- Some patients will improve after they are told the diagnosis in a compassionate, non-judgmental fashion.
- If new diagnosis or diagnostic uncertainty consider admission for neurology consult and video EEG.
- Psychiatric intervention is the main treatment modality (e.g. outpatient cognitive behavioral therapy).
- The purpose of psychiatric consultation is to identify underlying psychiatric conditions that can help direct treatment.
- In case of significant emotional stress, administer a mild tranquilizing agent (e.g. lorazepam 1-2mg IM/IV; hydroxyzine 50-100mg IM)
Disposition
- If symptoms improve consider discharge with close neurology and psychiatry follow-up to rule out epilepsy and identify and treat the underlying psychiatric origin of symptoms.
- If symptoms cannot be controlled or patient/family are not accepting of diagnosis. Consider admission for observation and further evaluation.
Prognosis
- 25-38 percent of patients achieve "seizure" freedom
- Children have a better prognosis than adults, with 70-80% achieving remission
See Also
External Links
References
- ↑ Ebru Apaydın Doğan, Ali Ünal, Aslıhan Ünal, Çağla Erdoğan, Clinical utility of serum lactate levels for differential diagnosis of generalized tonic–clonic seizures from psychogenic nonepileptic seizures and syncope, Epilepsy & Behavior, Volume 75, 2017, Pages 13-17, ISSN 1525-5050, https://doi.org/10.1016/j.yebeh.2017.07.003. (http://www.sciencedirect.com/science/article/pii/S1525505017304821)
- Chen DK. Psychogenic Non-epileptic Seizure. Uptodate. Updated May 18, 2018. Accessed June 1, 2018. https://www.uptodate.com/contents/psychogenic-nonepileptic-seizures?search=psychogenic%20nonepileptic%20seizures&source=search_result&selectedTitle=1~31&usage_type=default&display_rank=1