Neutropenic enterocolitis
(Redirected from Neutropenic enterocolitis (typhlitis))
Background
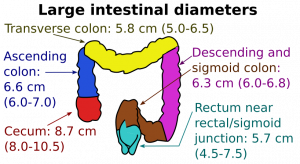
Average inner diameters and ranges of different sections of the large intestine.[1]
- Also known as "typhlitis"
- Necrosis of bowel wall secondary to polymicrobial invasion
- Involves terminal ileum and colon
- May progress to full-thickness infarction/perforation
Clinical Features
- Typically presents 10-14d after cytotoxic therapy
- Fever
- RLQ pain
- Nausea/vomiting
Differential Diagnosis
Oncologic Emergencies
Related to Local Tumor Effects
- Malignant airway obstruction
- Bone metastases and pathologic fractures
- Malignant spinal cord compression
- Malignant Pericardial Effusion and Tamponade
- Superior vena cava syndrome
Related to Biochemical Derangement
- Hypercalcemia of malignancy
- Hyponatremia due to SIADH
- Adrenal insufficiency
- Tumor lysis syndrome
- Carcinoid syndrome
Related to Hematologic Derangement
Related to Therapy
- Chemotherapy-induced nausea and vomiting
- Cytokine release syndrome
- Chemotherapeutic drug extravasation
- Differentiation syndrome (retinoic acid syndrome) in APML
- Stem cell transplant complications
- Catheter-related complications
- Tunnel infection
- Exit site infection
- CVC obstruction (intraluminal or catheter tip thrombosis)
- Catheter-related venous thrombosis
- Fracture of catheter lumen
- Oncologic therapy related adverse events
RLQ Pain
- GI
- Appendicitis
- Perforated appendicitis
- Peritonitis
- Crohn's disease (terminal ileitis)
- Diverticulitis (cecal, Asian patients)
- Inguinal hernia
- Mesenteric ischemia
- Ischemic colitis
- Meckel's diverticulum
- Neutropenic enterocolitis (typhlitis)
- Appendicitis
- GU
- Other
Evaluation
Workup[2]
- CBC with neutropenia, thrombocytopenia
- Blood cultures positive in ~25-85%, frequently bowel organisms
- CT A/P: cecal distention, wall thickening, pneumatosis intestinalis, intestinal perforation, fat stranding
- Avoid endoscopic evaluation due to risk of perforation, hemorrhage, bacterial translocation, worsening sepsis
Management
- Bowel rest
- NG tube to suction
- IVF
- TPN
- Consider G-CSF, particularly neutropenia < 100/ml and severe disease[3]
- Broad spectrum antimicrobials, in particular against gut microbiota to include[4]:
- Metronidazole plus cefepime
- Piperacillin-tazobactam
- Amphotericin B when patient remains febrile, neutropenic for greater than 5 days despite broad spectrum antibiotics
- Surgical consult (possible need for right hemicolectomy)[5]
Disposition
- Admit
See Also
References
- ↑ Nguyen H, Loustaunau C, Facista A, Ramsey L, Hassounah N, Taylor H, et al. (July 2010). "Deficient Pms2, ERCC1, Ku86, CcOI in field defects during progression to colon cancer". Journal of Visualized Experiments (41). doi:10.3791/1931. PMC 3149991. PMID 20689513.
- ↑ Machado NO. Neutropenic enterocolitis: A continuing medical and surgical challenge. N Am J Med Sci. 2010 Jul; 2(7): 293–300.
- ↑ Greil R, Psenak O, Roila F. ESMO Guidelines Working Group. Hematopoietic growth factors: ESMO recommendations for the applications. Ann Oncol. 2008;19(suppl 2:ii):116–1118.
- ↑ Gorschluter M, Mey U, Strehl J, Zinske C, Schepke M, Schmid F, Wolf IG, Sauerbruch T, Glasmacher A, et al. Neutropenic enterocolitis in adults: systematic analysis of evidence quality. Eur J Haematol. 2005;75(1):1–13.
- ↑ Williams N, Scott AD. Neutropaenic enterocolitis : a continuing surgical challenge. Br J Surg. 1997;84(9):1200–1205.


