Mesenteric ischemia
Background
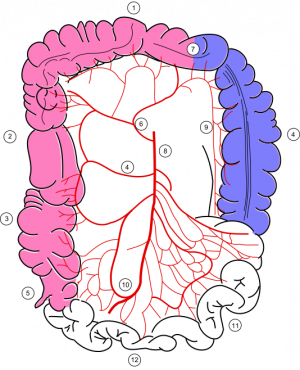
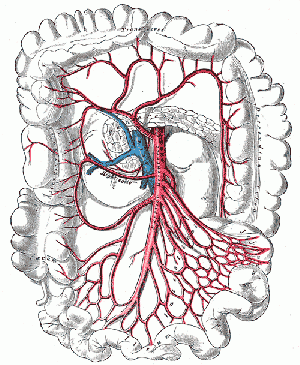
Colonic blood supply. Pink - supply from superior mesenteric artery (SMA) and its branches: middle colic, right colic, ileocolic arteries. Blue - supply from inferior mesenteric artery (IMA) and its branches: left colic, sigmoid, superior rectal artery. 7 is for so-called Cannon-Böhm point (the border between the areas of SMA and IMA supplies), which lies at the splenic flexure.
- Most commonly superior mesenteric artery (SMA), thus typically involves small bowel (especially jejunum) and right colon
- Left colon uncommonly involved due to collateral flow
- Mean age = 70 years old (>70% of cases occur in women)
Pathophysiology
4 distinct entities:
- Mesenteric arterial embolism (ex. Afib)
- Mesenteric arterial thrombosis (ex. Vasculopath)
- Nonocclusive mesenteric ischemia (ex. Hypovolemia from diuretics)
- Mesenteric venous thrombosis (ex. hypercoagulable state)
Intestinal Ischemic Disorder Types
- Ischemic colitis
- Accounts for 80-85% of intestinal ischemia
- Due to non-occlusive disease with decreased blood flow to the colon.
- Causes decreased perfusion leading to sub-mucosal or mucosal ischemia only.
- Typical to the "watershed areas" of the colon (Splenic flexure or Sigmoid)
- Acute mesenteric ischemia
- Due to complete occlusion of mesenteric vessels
- Complete transmural ischemia
- Mesenteric venous thrombosis
- Chronic mesenteric ischemia ("intestinal angina")
Risk Factors
| Type | Risk Factor |
|---|---|
| Arterial Embolism |
|
| Arterial Thrombosis |
|
| Venous Thrombosis |
|
| Nonocculsive |
|
Clinical Features
- Pain out of proportion to exam
- Abdomen often soft, without guarding.
- Pain often left sided around watershed areas of colon (splenic flexure and recto-sigmoid junction)
- Severe, generalized, colicky
- Bloody stools
Differential Diagnosis
Colitis
- Infectious colitis
- Ischemic colitis
- Ulcerative colitis
- CMV colitis
- Crohn's colitis
- Toxic colitis (antineoplastic agents)
- Pseudomembranous colitis
- Fibrosing colonopathy (Cystic fibrosis)
Diffuse Abdominal pain
- Abdominal aortic aneurysm
- Acute gastroenteritis
- Aortoenteric fisulta
- Appendicitis (early)
- Bowel obstruction
- Bowel perforation
- Diabetic ketoacidosis
- Gastroparesis
- Hernia
- Hypercalcemia
- Inflammatory bowel disease
- Mesenteric ischemia
- Pancreatitis
- Peritonitis
- Sickle cell crisis
- Spontaneous bacterial peritonitis
- Volvulus
Evaluation
Workup
- Labs
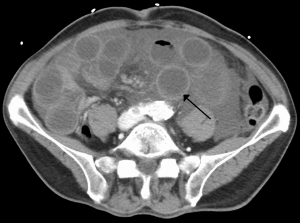
- CTA abdomen/pelvis (Bowel wall edema is the most common finding on CT)
- Mesenteric angiography considered gold standard (if available, typically as a secondary study)
Diagnosis
- Typically diagnosed on CT
- Labs may show the following (although do not rule need for CT):
- Lactate (higher later)
- WBC (often >15K)
- Chemistry (metabolic acidosis)
- Hyperphosphatemia
Management
General
- Aggressive IVF resuscitation, continued after revascularization due to capillary leak
- Correct electrolyte imbalances prior to IV contrast or surgical exploration[1]
- Analgesia (usually Opioids
- IV antibiotics - broad spectrum antibiotics to prevent sepsis [2]
- Second-generation cephalosporin plus metronidazole[3], OR
- Levofloxacin 500 mg IV q24 hours PLUS Metronidazole 15 mg/kg IV LOAD over 1 hour, for severely ill, maintenance 500 mg IV q6 hours,[4] OR
- Piperacillin/tazobactam 3.375 mg IV q6 hours
- Anticoagulation with heparin is usually appropriate in all patients with mesenteric ischemia, with exception of those with typical contraindications
- Some experts will recommend delaying heparin for 48 hours due to risk for intraluminal bleeding in bowels[5]
Acute arterial embolus
- Papaverine infusion (30-60m g/h IV) OR
- Surgical embolectomy OR
- Mesenteric artery bypass surgery OR
- Retrograde open mesenteric stenting OR
- tPA intra-arterial thrombolysis with IR
- PLUS/MINUS surgical resection of necrotic bowel after any of above interventions
- PLUS/MINUS 24-48 hour second-look surgery
Nonocclusive mesenteric ischemia
- Transcatheter vasodilation via:
- PGE1, alprostadil
- PGI2, epoprostenol
- Papaverine, most commonly used, though use in caution with angina, recent stroke, MI, glaucoma
Mesenteric venous thrombosis
- Heparin/warfarin either alone or in combination with surgery
- Up to 5% of patients require intervention beyond anticoagulation alone[6]
- Immediate heparinization should be started even when surgical intervention is indicated
- Decreases progression of thrombosis and improves survival
- PLUS/MINUS tPA intra-arterial thrombolysis with IR
- PLUS/MINUS laparotomy for evidence of bowel necrosis, peritonitis, stricture, severe GI bleeding
Chronic mesenteric ischemia
- Angioplasty with or without stent placement or surgical revascularization
Disposition
- Admit with consultation of one or more of the following:
- IR
- Vascular
- Surgery
See Also
External Links
References
- ↑ Wyers MC. Acute mesenteric ischemia: diagnostic approach and surgical treatment. Semin Vasc Surg. 2010 Mar;23(1):9-20.
- ↑ Acute mesenteric ischemia. Curr Gastroenterol Rep 2008;10:341
- ↑ Klar E, Rahmanian PB, Bücker A, Hauenstein K, Jauch KW, Luther B. Acute mesenteric ischemia: a vascular emergency. Dtsch Arztebl Int. 2012 Apr;109(14):249-56 full-text, commentary can be found in Dtsch Arztebl Int 2012 Oct;109(42):709 full-text, Dtsch Arztebl Int 2012 Oct;109(42):710.
- ↑ Berland T, Oldenburg WA. Acute mesenteric ischemia. Curr Gastroenterol Rep. 2008 Jun;10(3):341-6.
- ↑ Brandt LJ, Boley SJ. AGA technical review on intestinal ischemia. American Gastrointestinal Association. Gastroenterology. 2000 May;118(5):954-68.
- ↑ Clair DG, Beach JM. Mesenteric Ischemia. N Engl J Med. 2016 Mar 10;374(10):959-68.