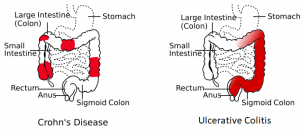
Ulcerative colitis
Background
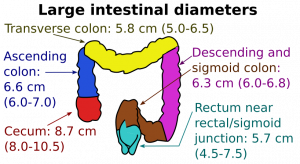
Average inner diameters and ranges of different sections of the large intestine.[1]
- Inflammation tends to be progressively more severe from proximal to distal colon
- Rectum is almost always involved
- Peak incidence occurs in second and third decades of life
Crohn's disease vs. ulcerative colitis
| Finding | Crohn's disease | Ulcerative colitis |
| Depth of inflammation | May be transmural, deep into tissues | Shallow, mucosal |
| Distribution of disease | Patchy areas of inflammation (skip lesions) | Continuous area of inflammation |
| Terminal ileum involvement | Commonly | Seldom |
| Colon involvement | Usually | Always |
| Rectum involvement | Seldom | Usually (95%) |
| Involvement around anus | Common | Seldom |
| Stenosis | Common | Seldom |
Clinical Features
- Abdominal cramps and diarrhea (often bloody)
Classification
- Mild
- <4 bowel movements per day
- No systemic symptoms
- Few extraintestinal manifestations
- Occasional constipation and rectal bleeding
- Moderate
- Colitis extends to splenic flexure
- Severe
- Frequent BM
- Anemia
- Fever
- Weight loss
- Frequent extraintestinal manifestations
- Pancolitis
Differential Diagnosis
Colitis
- Infectious colitis
- Ischemic colitis
- Ulcerative colitis
- CMV colitis
- Crohn's colitis
- Toxic colitis (antineoplastic agents)
- Pseudomembranous colitis
- Fibrosing colonopathy (Cystic fibrosis)
Evaluation
Work-up
- CBC
- Chemistry
- LFTs/lipase
- Consider:
- ESR/CRP
- Fecal calprotectin[2] (typically requested by GI)
- Type and screen (if significant bleeding)
- Imaging
- Consider CT based on clinical features and need to rule out more concerning processes
Diagnosis
- Positive atypical p-ANCA and negative ASCA is specific for ulcerative colitis
Management
- Rule-out complications:
- Hemorrhage
- Toxic megacolon
- Develops in advanced disease when all the layers of the colon become involved
- Presentation
- Severely ill
- Abdomen distended, tender, peritonitis
- Fever, tachycardia
- Leukocytosis (may be masked if patient taking steroids)
- Perforation results in high mortality
- Abdominal x-ray: long, continuous segment of air-filled colon >6cm in diameter
- Perirectal fistula
- Perirectal abscess
- Obstruction (due to stricture)
- Carcinoma
- Steroids
- Parenteral vs PO depending on severity
- PO: prednisone 40mg x 2wks, then decrease by 5mg per week
- Parenteral vs PO depending on severity
Medication Dosing
Prednisone 40mg daily x 2 weeks, then taper by 5mg/week PO
Disposition
- Admit for severe complication or severe flare requiring IV steroids
See Also
References
- ↑ Nguyen H, Loustaunau C, Facista A, Ramsey L, Hassounah N, Taylor H, et al. (July 2010). "Deficient Pms2, ERCC1, Ku86, CcOI in field defects during progression to colon cancer". Journal of Visualized Experiments (41). doi:10.3791/1931. PMC 3149991. PMID 20689513.
- ↑ van Rheenen PF, Van de Vijver E, Fidler V. Faecal calprotectin for screening of patients with suspected inflammatory bowel disease: diagnostic meta-analysis. BMJ. 2010;15(341):c3369.