Harbor:Admission and consultation guidelines
Admission and Consultation Rules
The following guidelines for specific medical disorders are intended to expedite care of ED patients. They have been reviewed and agreed upon by all Departments and Divisions that provide consultation to the Adult ED.
The detailed guidelines can be found in HUMC Policies 312 File:HUMC Policy 312.pdf and 370 File:HUMC Policy 370.pdf (Official Feb 2020). Any new agreements are so annotated below.
Admission Decisions
- The ED Attending will determine the need for admission for all ED patients (AED, RME, PED) with input from consulting services
- The ED Attending will determine appropriateness for OBS/CORE with input from UR
- The ED attending has admitting privileges to all inpatient services; for cases with no specific guidelines, the ED Attending will use their best professional judgment in determining the admitting service
- The ED Attending should document the rationale for admission, admitting service, and required level of care
- A collaborative discussion should be had with the admitting service
- After discussion with the admitting service, the ED provider will place the admission order which transfers care to the admitting service (unless there is a medical emergency)
- If an admitting service attending feels the patient would be best cared for on another inpatient service, the admitting attending should speak to the attending of that service and a final decision should be accomplished and reported back to the ED attending within 30 minutes; if this does not occur, escalate to the associate/CMO who will make the decision
- If there is disagreement about a admitting service, the ADMITTING ATTENDING NEEDS TO CALL THE ALTERNATE/MORE APPROPRIATE ADMITTING SERVICE ATTENDING
- If an admitting service attending feels the patient would be best cared for on another inpatient service, the admitting attending should speak to the attending of that service and a final decision should be accomplished and reported back to the ED attending within 30 minutes; if this does not occur, escalate to the associate/CMO who will make the decision
- If the admitting service has not evaluated the patient and placed orders within 2 hours of the admission, the ED should place abbreviated admission orders ("holding orders" - activity, vitals, oxygen, IV)
- Patients <18 will be admitted to Pediatrics; ages 18-20 will be admitted to Pediatrics at the discretion and capacity of the Peds service
Consults
- Always check Medhub for the most current schedule
- If no one is listed, please call ED AOD to escalate to Drs. Gutierrez & Harrington
- Consult via Orchid as soon as you know the service is needed to expedite patient throughput
- Service transition time is generally 7am (from night team to the following day team)
- Agreed by:
- Hand Call @ 7am (6/5/23): Plastics (Dr. Do), Ortho (Dr. Gold)
- Face Call @ 7am (6/12/23): Plastics (Dr. Do), OMFS (Dr. Crum), ENT (Dr. Kedeshian), Dr. de Virgilio (Surgery Chair)
- Agreed by:
Complicating Medical Conditions (CMC)
- One or more active acute medical conditions that the non-IM/FM service does not usually manage AND is likely to require ongoing management or active monitoring during the hospitalization; the decision of what constitutes a CMC is made by the ED Attending
- Any discussion for most appropriate admitting service given a CMC will occur at the attending level (inpatient service & ED); elevation to division chief/department chair, then associate/CMO (Dr. Stein/Dr. Mahajan); chief residents cannot replace an attending for this discussion
- Service specific, so it might vary by services
- Consideration: Simply having stable co-morbidities that require continuation of home medications and therapies does NOT constitute a reason to deviate from the admission guidelines
- Consideration: Significant co-morbidities that separately would require admission to a medicine service, consider admitting that patient to medicine with the surgical or specialty service on consult
- If there is disagreement about a CMC, the ADMITTING ATTENDING NEEDS TO CALL THE ED ATTENDING
- Service specific, so it might vary by services
- Residents cannot overrule admission decisions made by the ED attending
- Residents cannot discharge a patient from the ED who has been admitted to their service without an explicit discussion and agreement from their attending
- If an admitting service attending feels the patient would best be cared for on another inpatient service, the admitting attending should speak with the attending of that service. A final decision between the two inpatient service attendings about which admitting service is most appropriate should be accomplished within 30 minutes and reported back to the ED attending.
- Assisting services for specific CMCs
- Primary surgical admission requiring ICU care will be admitted to the trauma/surgical ICU
- C-team can be consulted for CHF as a complicating medical condition
- Nephrology can be consulted to assist with HTN as a complicating medical condition
- Geriatrics may be consulted 24/7 and is available to assist in the care of patients greater than 65 years old (will go as low as 60 for ortho patients)
- Endocrine: may be consulted to assist with blood sugar management
- Nephrology: may be consulted to assist with blood pressure control; if the patient needs cardiac clearance as well, cardiology can perform this function and help manage hypertension
- Pre-operative Clearance: If >65, consult geriatrics; otherwise, third-call can assist in providing this service
Aortic Aneurysms
- Aortic Aneurysms & Dissections
- Thoracic (Type A or B) - admit to trauma surgery (or CTS if immediately available)
- Abdominal Aneurysm
- Expanding or ruptured to trauma (or vascular if immediately available)
- Stable aneurysms can be admitted to other services based on reason for admission
- Abdominal Dissection - trauma (or vascular if immediately available)
BOA
Mother & Baby workflow File:BOA Mother-Baby Workflow 7 14 20 (1).pdf
Brain Death
- Admit to the service who would have cared for the primary illness or injury
- Trauma - trauma patient
- Neurology - intracranial hemorrhage, stroke
- IM/FM - medical/cardiac cause
- Peds/PICU - all peds
- Admitting service should notify organ donation agency
Breast abscess/mastitis
- Breast Abscess Pathway
- Abscess
- ED aspirating (POCUS if needed)
- If you need a formal US after hours to confirm abscess, order "US Chest (R or L)" STAT [radiology only reads "Chest US", BDC only reads "Breast US"]
- Needle aspiration, send wound culture
- Standard care is needle aspiration 2x prior to I&D
- Discharge with PO antibiotics
- Keflex, dicloxacillin if lactating, bactrim or doxycycline if concern for MRSA
- Follow-up:
- DHS: ED Request for Specialty Appointment: Surgery-Breast for the following Tuesday (in 7-14 days)
- OOP: PCP in 7 days
- ED aspirating (POCUS if needed)
- If sending to BDC for needle aspiration
- 7a-3:30p (DHS or OOP) call BDC at x68178 to add case (fellow p3386, alt# x67406)
- Place ORDER for: "US Breast (R or L) STAT" and "US Drainage Abscess or Cyst" and note location of suspected abscess (X o'clock, X cm from nipple)
- Patient will return to the ED from BDC post-procedure
- BDC will arrange f/up with Breast Surgery Clinic if DHS, patient to f/up with PCP if OOP
- Start PO Antibiotics
- Keflex, dicloxacillin if lactating, bactrim or doxycycline if concern for MRSA
- Afterhours DHS Patients:
- Place FUTURE ORDER for: "US Breast (R or L) URGENT" and "US Drainage Abscess or Cyst" and note location of suspected abscess (X o'clock, X cm from nipple)
- Message Har-BDC message pool for appt
- BDC will arrange f/up with Breast Surgery Clinic if DHS, PCP if OOP
- Start PO Antibiotics
- Keflex, dicloxacillin if lactating, bactrim or doxycycline if concern for MRSA
- BDC will schedule follow-up for DHS patients or instruct OOP patients to f/up with PCP
- Afterhours OOP Patients: can consult surgery for the I&D; will need to f/up with PCP for outpatient drainage
- 7a-3:30p (DHS or OOP) call BDC at x68178 to add case (fellow p3386, alt# x67406)
- Needs I&D (failed needle aspiration(s) or overlying skin is unhealthy)
- I&D can be done by either ED or Breast Surgery (consult Trauma afterhours)
- Follow-up:
- DHS: ED Request for Specialty Appointment: Surgery-Breast for the following Tuesday (in 7-14 days)
- OOP: PCP in 7 days
- Septic Patient
- Initiate IV antibiotics
- For mastitis/cellulitis requiring IV antibiotics, admit to IM/FM
- For patients needing operative intervention, admit to Breast Surgery (covered by trauma from 7p to 7a)
- Abscess
- Schedule into BDC if:
- Palpable mass persists after 14-21 days, ultrasound and needle biopsy should be performed of solid components by radiology department
- Recurrent mastitis/abscess, or chronic granulomatous mastitis
- DHS expected practice and agreed upon by Radiology, Acute Care Surgery, Breast Surgery, EM: 2021 DHS Best Practice - Mastitis-Breast Abscess
Breast mass/malignancy
- DHS Empaneled/DHS Eligible Breast mass concerning for malignancy (THIS PATHWAY IS THE FASTEST WAY TO EXPEDITE A WORKUP)
- OOP - direct patient to their in-plan PCP for coordination of care
- OPTION 1 - NO BIOPSY-PROVEN DIAGNOSIS - Breast Diagnostic Center for imaging
- OPTION 1a - Suspicious for malignancy with NO obvious METASTASES
- Order Bilateral Mammogram and Unilateral US - future visit within 2 weeks
- "MG Mammogram Diagnostic" order set: "Mammogram Digital Diagnostic Bilateral URGENT" and "US Breast (R or L) URGENT"; Order detail must include chief complaint, relevant med/fam hx, location of mass (X o'clock, X cm from nipple)
- Message Har-BDC message pool and PCP (send to Reg 6 if no PCP)
- BDC will perform imaging, biopsy, and arrange f/up with Breast Surgery Clinic
- Order Bilateral Mammogram and Unilateral US - future visit within 2 weeks
- OPTON 1b - Suspicious for malignancy WITH obvious METASTASES (excludes local axillary lymph node spread)
- Order Bilateral Mammogram and Unilateral US - future visit within 1 week
- "Mammogram Digital Diagnostic Bilateral URGENT" and "US Breast (R or L) URGENT"; Order detail must include chief complaint, relevant med/fam hx, location of mass (X o'clock, X cm from nipple)
- Message Har-BDC message pool, PCP (send to Reg 6 if no PCP)
- Page oncology to expedite outpatient workup
- ED Request for Specialty Appointment: Oncology-New in the timeframe recommend by Oncology consultant
- BDC will perform the imaging, biopsy, and the patient will f/up with Oncology Clinic (NOT Breast Surgery)
- Order Bilateral Mammogram and Unilateral US - future visit within 1 week
- OPTION 2 - Newly diagnosed breast cancer WITH A BIOPSY-PROVEN DIAGNOSIS
- OPTION 2a - BIOPSY CONFIRMED WITHOUT obvious METASTATIC disease (excluding local axillary lymph node spread
- Pt MUST obtain records (CD images, path slides, reports)
- If the patient does not have BOTH imaging and path results, they must go to Breast Diagnostic Center first
- ED Request for Specialty Appointment: Surgery-Breast Oncology in 7-14 days
- Pt MUST obtain records (CD images, path slides, reports)
- OPTION 2b - BIOPSY CONFIRMED WITH obvious METASTATIC disease
- Page oncology to expedite outpatient workup
- ED Request for Specialty Appointment: Oncology-New in the timeframe recommend by Oncology consultant
- BDC will perform the imaging, biopsy, and the patient will f/up with Oncology Clinic (NOT Breast Surgery)
- Page oncology to expedite outpatient workup
- Random Scenarios
- If unsure if a mass or abscess, schedule into BDC and order the imaging
- Mastalgia, breast lesion needing excision for non-malignant lesion, need for cancer surveillance after losing insurance elsewhere - NERF/message PCP for e-consult
Burns
- Transfer to burn center AFTER Trauma service consultation if meets ABA burn center referral criteria
- Partial thickness burns greater than 10% total body surface area (TBSA)
- Burns that involve the face, hands, feet, genitalia, perineum, or major joints
- Third degree burns in any age group
- Electrical burns, including lightning injury
- Chemical burns
- Inhalation injury
- Burn injury in patients with preexisting medical disorders that could complicate management, prolong recovery, or affect mortality
- Any patient with burns and concomitant trauma (such as fractures) in which the burn injury poses the greatest risk of morbidity or mortality. In such cases, if the trauma poses the greater immediate risk, the patient may be initially stabilized in a trauma center before being transferred to a burn unit. Physician judgment will be necessary in such situations and should be in concert with the regional medical control plan and triage protocols
- Burned children in hospitals without qualified personnel or equipment for the care of children
- Burn injury in patients who will require special social, emotional, or rehabilitative intervention.
- LAG cannot refuse transfers
Cardiology
REVIEW
- Cardiology consults and admissions:
- For quick questions during business hours, CORE fellow p1035 (follow up, CORE vs Cteam admission, etc.)
- For Admits, contact Third call p6534
- For anything else (potential STEMI, not sure what a patient has, not sure what the rhythm is, discharge coordination when CORE isn’t here, etc.) --> Fellow consult pager - p6493
- Any issues reaching on-call fellow, 1) check MedHub and call the on-call fellow, or 2) call the CCU, or 3) consider contacting attending
- Starting 10/4: CORE NP taking CORE admits until 8p Mon - Thurs
CHF
- If estimated <2 midnight stay, place in Cardiology Observation Rapid Evaluation area (CORE) CORE
- Admit any patients with anasarca (including abdominal or scrotal edema)
- If estimated >2 midnight stay:
- Admit to IM/FM (tele/PCU) if all of the following are met:
- Low suspicion for ACS (as determined by ED attending)
- HR < 110
- BP > 110
- Creatinine <2.0 (unless ESRD on HD)
- No BiPAP required at any time in the ED
- Admit to Cardiology (C-team) if the above criteria are not met or the patient needs ICU care
- Admit to IM/FM (tele/PCU) if all of the following are met:
Cellulitis, Abscess, NSTI
- Cellulitis
- IM/FM
- EXCEPTION: Hand Call (plastic surgery or ortho) - upper extremity cellulitis (hand to AC, or proximal to AC if primarily below) or deep space hand
- Soft tissue abscess
- Trauma - all except face, neck, mouth, or distal arms; even if drained in the ED
- Spine call - epidural abscess
- NSTI - trauma surgery
- Maxillofacial cellulitis or abscess
- Optho - periorbital/orbital
- OMFS - odontogenic infection or facial cellulitis secondary to dental
- "Tooth Call" pager: 800-233-7231 x32831 (per ENT 10-2-16)
- ENT - dental infection with facial cellulitis AND neck extension WITH risk of rapid loss of airway, deep space neck infection, or sinus infection
- Face call - all other maxillofacial infections
Dialysis fistula/graft problem (e.g. bleeding or thrombosed)
- Trauma (or vascular if immediately available) if needs immediate operative intervention (uncontrolled bleeding)
- Require IR
- If unable to perform outpatient, admit to IM/FM
- IM/FM (with vascular and nephrology) if requires more than IR
- Less than 30 days post-op - trauma consult in the ED
Decubitus Ulcers
- Trauma/ACS - admit when patients require hospitalization primarily for surgical debridement of decubitus ulcers
- IM/FM - admit when patients require hospitalization primarily for management of medical problems but also have decubitus ulcers
- 11/1/2022 - Drs. Thomas, Putnam, Schickedanz, Goolsby
Deep venous thrombosis
- DVT
- Vascular Surgery (through Trauma Surgery afterhours) for phlegmasia or subsequent compartment syndrome
- Phlegmasia alba dolens painful swollen white leg from early arterial compromise
- Phlegmasia cerulea dolens = painful swollen cyanotic leg, bullae and necrosis from later arterial compromise
- Heparin 80-100U/kg followed by infusion of 15-18U/kg/hr
- Consider IR for thrombectomy:
- Acute symptom onset of 14 days or less in the target limb.
- Presence of proximal DVT (inferior vena cava, iliac vein, common femoral vein, deep femoral vein, and femoral vein) that was objectively diagnosed with CT and/or US scan
- Symptomatic DVT (pain, neurological deficit) or impairment of the tissue perfusion (phlegmasia) and less than 14 days' duration
- Symptomatic DVT defined as meeting at least one of the following clinical indicators:
- rVCSS Pain Score ≥2
- New edema of calf or thigh (CEAP ≥3)
- Limited mobility or bed bound due to pain / swelling
- Symptomatic DVT defined as meeting at least one of the following clinical indicators:
- Acute symptom onset of 14 days or less in the target limb.
- If needs admission, IM/FM
- <30-day post-op, admit to surgical service who performed the operation
- OB/Gyn - pregnant, <6-weeks post-partum, due to gyn malignancy
- Vascular Surgery (through Trauma Surgery afterhours) for phlegmasia or subsequent compartment syndrome
Delirium/Dementia
- Acute delirium
- IM/FM
- Dementia
- Dr. Kronfeld, Director of Inpt Neuro, 7/2022
- Typically, concern for gradual onset dementia does not warrant admission solely for workup
- Discharge with neuro clinic follow-up if neurology recommends outpatient evaluation of the patient
- May need to consider Placement Pathway (consult SW, PT/OT, UR, and involve ED AOD ASAP)
- If rapidly progressive dementia, consider UDS, psych consult, LP, and inpatient admission/MRI
- Typically, concern for gradual onset dementia does not warrant admission solely for workup
- If admission is warranted:
- Neuro - new onset or previously undiagnosed
- IM/FM - new onset with one or more complicating medical condition
- Dr. Kronfeld, Director of Inpt Neuro, 7/2022
Diabetic Foot Infections
- Effective 10-4-2023: all diabetic foot infections will go to IM/FM with limb salvage consultation (Dr. Thomas, IM Chair; Dr. Miller, Limb Salvage)
- Hold antibiotics until surgery evaluation unless the patient is septic or has rapidly progressing infection
- Consult Limb Salvage (or Trauma/ACS after-hours) if being admitted for another primary medical condition but also has a diabetic foot infection (Confirmed with Dr. Putnam 7-15-2021)
Disposition Problems
- Patients with placement needs, see Harbor:Placement_patients for more detailed tips
- Consult SW early, many resources only available during business hours
- Offer family option of Harbor:Home_Health for PT/OT, home safety evals if can wait couple business days
- If unable to safely discharge, then need to admit (DHS) or transfer (if OOP) for placement, via Interqual request
- Admit to IM/FM for DHS patients that need long-term placement unless otherwise directed by UR
- If unable to transfer to patient's OOP network or unable to authorization to admit to IM/FM then:
- Ensure UR Director is aware via UR nurse.
- Let Harbor:DEM_Admin_on_Duty_(AOD) know, as may need higher level discussion
- EXCEPTIONS:
- Patient develops a complication from a medical or surgical problem and is already followed by that particular service in the outpatient setting should be admitted to that service
- Problem is solely surgical without complicating medical condition, admit to that surgical service (eg, cannot care for self due to fracture, admit to ortho)
GI Bleeding
- IM/FM: all patients with GI bleeding who require admission, including post-endoscopy
- GI should evaluate immediately if patient hemodynamically unstable or requiring massive transfusion; admit to MICU with Trauma / ACS consultation.
- Admit to Surgery only if established surgical patient that has GI bleeding potentially related to a surgical procedure
(Chair IM, Chief Trauma 5-8-20)
Gyn
- DRAFT
- D&C's
- Indications for vacuum aspiration: r/o ectopic, incomplete miscarriage (no FHTs), active miscarriage
- Gyn Clinic:
- Patients who can be reasonably managed on an outpt basis should have D&C in gyn clinic
- Patients requesting termination of pregnancy can be seen at ROC clinic on Wednesdays
- ED D&C indications:
- Patients experiencing symptoms that would generally necessitate taking to the OR solely for a D&C but are stable
- Patients who have extenuating barriers to clinic follow-up
- OB can perform paracervical block in the ED (no procedural sedation)
- Patients generally need to be monitored for 30 min post D&C
- Gyn to provide pictorial for appropriate amount of post-procedural bleeding and will re-eval pt if there is concern from the ED provider or RN
- NB/JL - need written policy ... same population as clinic; do in clinic during clinic hours; standard work in clinic; no sedation
- OR:
- Any patient with massive hemorrhage, hemodynamic instability, or expected prolonged recovery period
- Gyn Clinic:
- Indications for vacuum aspiration: r/o ectopic, incomplete miscarriage (no FHTs), active miscarriage
- D&C's
Hand Injuries & Infections
- Fractures of hand and forearm: Ortho
- EXCEPTION - isolated distal phalanx fractures: Hand call (plastics & ortho)
- Trauma patient need clearance by Trauma Surgery prior to admission
- Soft tissue injuries or infection up to elbow WITHOUT fracture: Hand call (plastics & ortho)
- Replant injuries will always be ORTHO as a fracture is involved
Hip Fractures
Click here for ED Pathway: Harbor Hip Fracture Pathway
- Suggested pre-op workup (UCSF Guideline):
- XR hip, pelvis, femur
- CBC, Chem 10, INR, Vitamin D, T&S
- CXR & EKG if history of heart or lung problems
Hypertension
- Patients with hypertension as a COMPLICATING MEDICAL CONDITION will be admitted to Internal Medicine/Family Medicine only if the hypertension is the primary reason for admission; otherwise, Nephrology may be consulted to assist with management.
Intracranial mass lesions
- Non-hemorrhagic intracranial masses
- Neuro with NS consult: new solitary lesion without hemorrhage
- IM/FM with NS consult: non-hemorrhagic mass WITH complicating medical condition OR likely metastatic disease
- Patients with known mass will be admitted to the service that manages them on outpt basis (eg, IM with oncology for glioma, Neuro for MS)
- Neurosurgery: hemorrhagic OR non-hemorrhagic mass that require emergent surgical intervention or ICP monitor will be admitted to Neurosurgery, regardless of the presence of a Complicating Medical Condition.
- ED will call NS with the specific question, "Is it surgical or does it need an ICP monitor?” If no, then admit to neuro (ED does not need to wait for the full consult, just the answer to the pointed question).
- Trauma: Trauma surgery has right of refusal for admitting any patients with a traumatic mechanism.
- 6/2023: Drs. Dhall (NS), Kronfeld (Neuro), Putnam (Trauma), & Chappell (ED)
Lower back pain
- Admit IM/FM pain control with no neuro deficits
- Could consider NS consult
- Neurosurgery: LBP with acute weakness, bowel/bladder incontinence, or requiring surgical intervention
Malignant Hyperthermia
- Call OR front desk x65200 to get the Malignant Hyperthermia Cart
Maxillofacial trauma
- Trauma: any maxillofacial traumatic injuries requiring admission
- Face Call: isolated non-traumatic maxillofacial diagnoses requiring surgical intervention
- Optho: isolated glob injury (eg, globe rupture)
Meningitis
- IM/FM
- Neuro can be consulted for diagnostic and management assistance
Neurosurgery
- Consult NS on any patient presenting within 30 days of surgery regardless of reason for visit (Dr. Dhall, NS Chair, 4/1/22)
NSTEMI
- C-team: if appears to be secondary to ACS or CHF
- IM/FM: if appears to be secondary to non-cardiovascular cause (eg, sepsis)
- Trauma: if appears to be secondary to a traumatic injury (eg, cardiac contusion after a motor vehicle accident) and NOT the etiology of the trauma (eg, cardiac syncope leading to a motor vehicle accident)
- Determination of the most likely cause of the NSTEMI will be made by the ED Attending
Optic Neuritis
- Admit to Neurology if requiring inpatient admission and alternate ophthalmologic condition is not suspected
Dr. Kronfeld (Director Inpatient Neuro) 2/9/2022
Osteomyelitis requiring admission
- Hand Call: hand and forearm
- Ortho: all other extremity osteo, especially if underlying hardware
- NS: osteo of the spine WITH acute weakness, numbness, or bowel/bladder incontinence
- IM/FM: all other osteo locations (including spine without neuro deficit)
Painless Jaundice
- Consider Expedited Work-up Clinic if stable for outpatient evaluation
- Message PCP if DHS empaneled
- CCC for EWC if the patient does not have a PCP
- IM/FM if requiring admission
Pancreatitis
- Trauma/ACS: if gallstones present on ultrasound
- Bedside US requires: gallbaldder wall thickness, comment on pericholecystic fluid, comment on gallstones, and diameter of the common bile duct or common hepatic duct
- If all 4 items are not present, formal US should be obtained
- Pancreatitis without gallstones, admit to IM/FM
Pathologic Fractures
- HUCLA can take care of small benign bone tumors (like UBC's or ABC's) with fracture, fracture through a known primary, or fracture through a met of known primary.
- We don't have orthopaedic oncology at Harbor.
- Transfer to USC if unclear whether new primary (not a met) because the fixation method and approach changes based on the primary
- If unclear, escalate to the HUMC Ortho Attending 24/7
Dr. Badkoobehi 12/14/2022
PEDIATRICS
Placement Patients
Pregnant Patients
- Consult OB for all pregnant patient requiring admission
- OB will admit all pregnant patients unless the patient has a medical or surgical condition that requires or is likely to require active management beyond the scope of practice of the Obstetrics and Gynecology service
- If the ED and OB attendings disagree with the admission service, the final decision is made by the OB attending
Pulmonary Embolus
- For all Confirmed PE or DVT with findings suggestive of PE (Clot in transit or right heart thrombi on TTE/TEE) but unable to obtain CTPA, risk stratify patient for PE Response Team Activation using ED PERT Activation Algorithm 2026.
- Risk Stratification
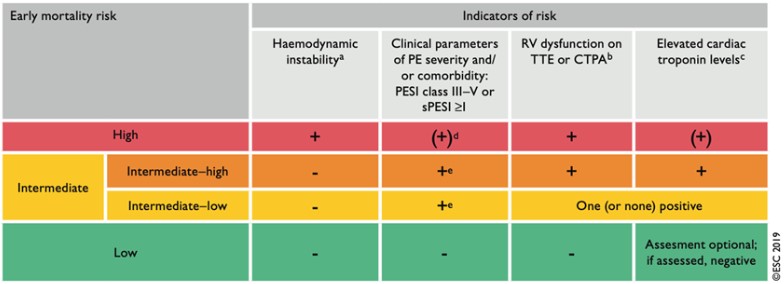
- Harbor UCLA's PERT Program currently uses the European Society of Cardiology (ESC) 2019 Guidelines for risk stratification to help determine treatment options and level of care:
- Definition of hemodynamic instability for risk stratification
- Cardiac arrest and need for cardiopulmonary resuscitation.
- Obstructive shock defined as a systolic blood pressure (BP) < 90 mmHg or vasopressors required to achieve a bp > 90 mmHg despite adequate filling status and end-organ hypoperfusion (altered mental status; cold clammy skin; oliguria/anuria; increased serum lactate)
- Persistent hypotension with a systolic BP < 90 mmHg or systolic BP drop > 40 mmHg, lasting longer than 15 minutes and not caused by new-onset arrhythmia, hypovolemia, or sepsis
- sPESI
- While you’re waiting for PERT you can…
- Begin anticoagulation if no absolute contraindication (see reference below)
- Strongly consider obtaining a head CT for patients who have underlying malignancy prior to starting anticoagulation
- Ensure the following labs are drawn and studies are ordered
- CBC w/diff, CMP, PTT/INR/Anti-Xa, troponin, BNP, lactate
- Bilateral lower extremity ultrasounds (consider upper extremity if patient has a chronic central line in place or symptomatic arms)
- TTE with PERT protocol
- Ensure at least x2 large bore PIVs; if central line is required for pressors then avoid non-compressible sites (e.g. subclavian vein)
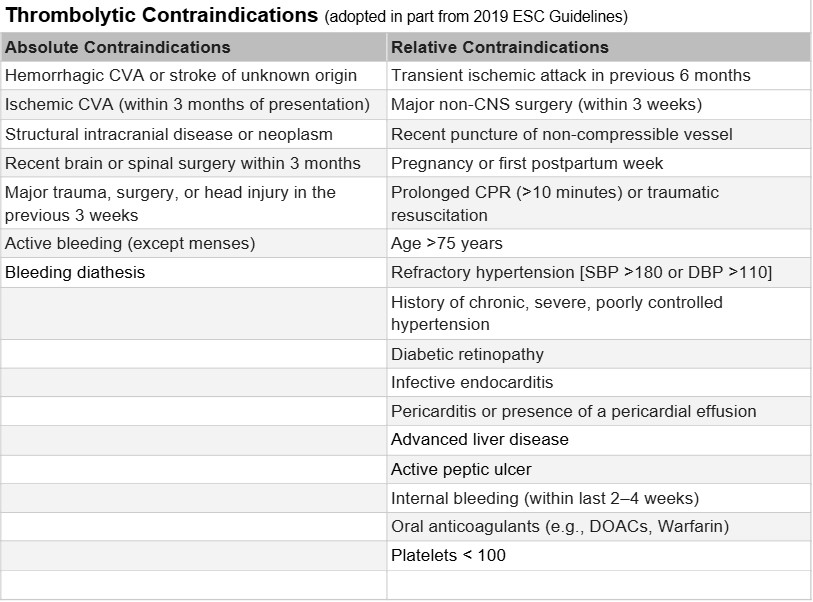
- Assess for thrombolysis contraindications (see table below)
- Anticoagulation Guidelines
- Unfractionated Heparin (UFH)
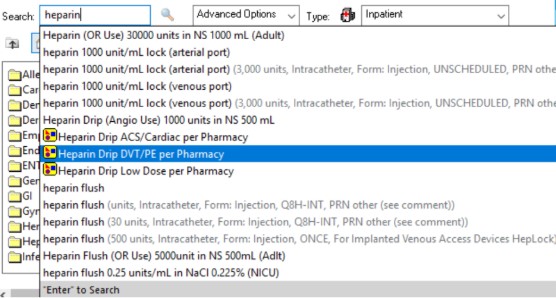
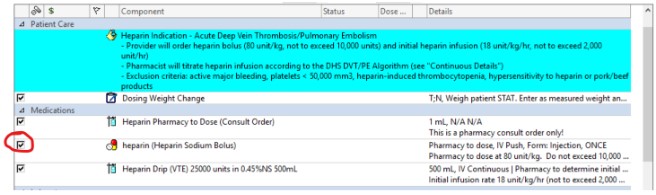
- Utilize Heparin Drip DVT/PE per Pharmacy subphase order set
- Note, this order set automatically includes a bolus of heparin. If this is not desired such as in patients who are at increased risk of bleeding, please unclick the checked off box
- Low Molecular Weight Heparin (LMWH): Enoxaparin 1 mg/kg q12h (avoid if CrCl < 30mL/min)
- DOACs (Low Risk Only):
- Rivaroxaban: 15 mg PO BID x 21 days -> 20 mg daily (avoid if CrCl < 30mL/min)
- Apixaban: 10 mg PO BID x 7 days -> 5 mg BID
- Note when able, Apixaban is favored over Rivaroxaban given decreased bleeding risk
- Unfractionated Heparin (UFH)
- Thrombolytic Contraindications
- Frequently Asked Questions
- PERT is not responding. What should I do?
- PERT should respond within 15 minutes. Repage x 1 and escalate to Pulmonary Consultation attending on call if no response (see MedHub for attending name and contact number).
- I consulted PERT. Do I need to reach out to IR, Cardiology, or Surgery for my patient to be considered for catheter-based or surgical intervention?
- No; PERT will coordinate and consult all the other members of the PERT program as needed on a case-by-case basis.
- I have a high-risk PE patient who is unstable and/or in extremis. Do I need to wait for PERT prior to giving thrombolytics?
- If the patient can be stabilized with vasopressors, holding off on the administration of thrombolytics until PERT is able to able to provide input to the patient’s care is preferred.
- If you feel you cannot wait for this response, then perform a quick assessment for contraindications for thrombolytic administration prior to starting the administration.
- My patient has a DVT. Do I activate PERT?
- No. If you later find a PE in your workup, then please follow the algorithm and determine if PERT consult is appropriate.
- For symptomatic DVTs, both IR and Vascular Surgery can help with the assessment and additional management strategies.
- I am unable to get a CTPA but am worried about a PE. Do I activate PERT?
- No. The PERT program is intended to assist in the care of patients with a confirmed PE in the intermediate- or high-risk range that might benefit from more advanced therapy beyond anticoagulation alone.
- If you need assistance with assessing the patient and would like additional help, please contact the Pulmonary Consultation service (pager 310-501-5194).
- A patient with a prior PE returns to the ED. Should I activate PERT?
- The answer is it depends...
- If they are coming in with a new PE event and have features consistent with an intermediate- or high-risk features, activate PERT.
- If they are coming in with a concern for anticoagulant failure in the setting of the original PE management, bleeding, or other concerns, PERT should not be activated. Consultation of medical subspecialty service including Hematology or Pulmonary can be obtained depending on the concern.
- The answer is it depends...
- I have a question about anticoagulation, but the patient does not have an acute PE. Who do I consult?
- Hematology/Oncology would be the consultation team to start with if there are questions specifically directed at anticoagulation choices alone.
- PERT is not responding. What should I do?
Drs. Vintch/Chappell/Grohmann 2-2026
Pyelonephritis
- Men and non-pregnant women, admit to IM/FM
- Urology: pyelonephritis associated with nephrolithiasis, urinary stents, obstructive uropathy, or nephrostomies
- If they have a Complicating Medical Condition, they will be admitted to Internal Medicine/Family Medicine with consultation by Urology
- OB/Gyn: pregnant women with pyelonephritis
- If they have a Complicating Medical Condition, they will be admitted to Internal Medicine/Family Medicine with consultation by OB/Gyn
Re-implant (Replant)
ROSC
- C-team: presumed cardiac etiology of cardiac arrest
- MICU: presumed non-cardiac etiology of cardiac arrest
- The presumed etiology will be determined by the ED Attending physician. Initiate TTM, consider CT head, with post ROSC care
Septic Arthritis
- Orthopedics unless the patient has systemic sepsis or complicating medical conditions
- IM/FM with ortho consult if CMC or sepsis
Spinal Injuries
- Trauma/ACS: All cervical, thoracic, or lumbar injuries
Stroke
- Neurology: All strokes (ischemic or hemorrhagic) EXCEPT:
- Trauma/ACS: traumatic ICH (if cleared by Trauma Surgery, admit to Neurosurgery)
- Non-traumatic ICH:
- Simultaneously consult NEURO and NEUROSURGERY
- Admit to Neurosurgery if the require emergent operative neurosurgical intervention or ICP monitor
- ED will call NS with the specific question, "Is it surgical or does it need an ICP monitor?” If no, then admit to neuro (ED does not need to wait for the full consult, just the answer to the pointed question).
- Neurology admit with NS consult: non-aneurysmal SAH or non-massive ICH (including post-tPA hemorrhage)
- Admit to Neurosurgery if the require emergent operative neurosurgical intervention or ICP monitor
- Simultaneously consult NEURO and NEUROSURGERY
- IM/FM with neurology if complicating medical condition
- 6/2023: Drs. Dhall (NS), Kronfeld (Neuro), Putnam (Trauma), & Chappell (ED)
Surgical Specialty Consults
- ALL surgical admissions (acute care or trauma) go to the "Surgery - Trauma" service
- For surgical subspecialty consults:
- Page Trauma/ACS
- During daytime hours, you can directly page the specialty service if you need a more rapid decision, especially if already known to specialty service
Thyroid Masses
- Refer to endocrinology
Trauma patients
- Trauma/ACS: will admit all multi-system trauma including fractures and must clear any TTA1 or TTA2 patients prior to admission to other services
- Hip Fractures: see Hip Fractures guideline
- Ortho: isolated traumatic fractures once cleared by trauma
Vaginal Bleeding
- Gyn: symptomatic anemia from vaginal bleeding requiring extended stay OR greater than 2U pRBC transfusion
See Also
References