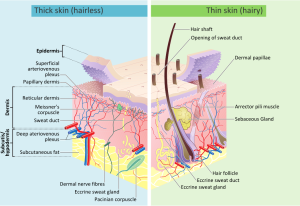
Hand-foot-and-mouth disease
Background
- Caused by coxsackie virus
- Most frequently in children, but can occur in all age groups
- Similar to Herpangina, but with additional hand/foot lesions
Clinical Features
- Brief prodrome with low fever, anorexia, sore mouth
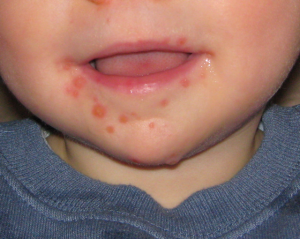
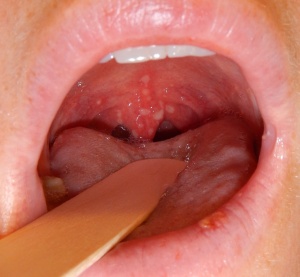
- Oral lesions appear 1-2d later
- Vesicles on erythematous base, will then ulcerate
- Painful
- Found on buccal mucosa, tongue, soft palate and gingiva
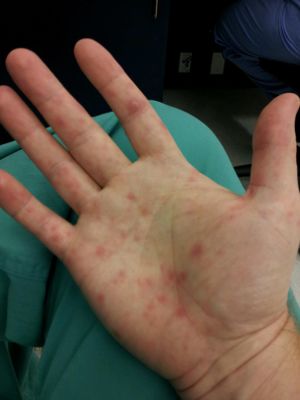
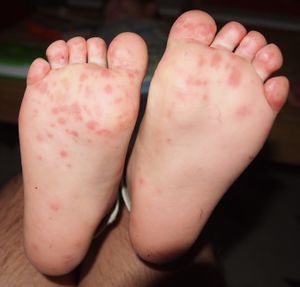
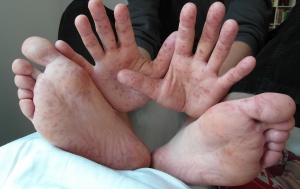
- Hand and sole of foot lesions
- Red papules that change to gray vesicles
- Resolves after 7–10 days
Differential Diagnosis
Pediatric Rash
- Atopic dermatitis
- Bed bugs
- Contact dermatitis
- Drug rash
- Erythema infectiosum (Fifth disease)
- Hand-foot-and-mouth disease
- Henoch-schonlein purpura (HSP)
- Herpangina
- Herpes simplex virus (HSV)
- Infectious mononucleosis
- Meningitis
- Measles
- Molluscum contagiosum
- Roseola infantum
- Rubella (German measles)
- Scabies
- Scarlet fever
- Smallpox
- Varicella (Chickenpox)
Vesiculobullous rashes
Febrile
- Diffuse distribution
- Varicella (chickenpox)
- Smallpox
- Monkeypox
- Disseminated gonococcal disease
- DIC
- Purpural fulminans
- Localized distribution
Afebrile
- Diffuse distribution
- Bullous pemphigoid
- Drug-Induced bullous disorders
- Pemphigus vulgaris
- Phytophotodermatitis
- Erythema multiforme major
- Bullous impetigo
- Localized distribution
- Contact dermatitis
- Herpes zoster (shingles)
- Dyshidrotic eczema
- Burn
- Dermatitis herpetiformis
- Erythema multiforme minor
- Poison Oak, Ivy, Sumac dermatitis
- Bullosis diabeticorum
- Bullous impetigo
- Folliculitis
Hand and finger infections
- Bed bugs
- Closed fist infection (Fight Bite)
- Hand cellulitis
- Hand deep space infection
- Hand-foot-and-mouth disease
- Herpetic whitlow
- Felon
- Flexor tenosynovitis
- Paronychia
- Scabies
- Sporotrichosis
Look-Alikes
Evaluation
- Clinical diagnosis, based on history and physical examination
- If unsure, see Pediatric Fever
Management
- No specific therapy for most; self-limited
- NSAIDS and cool liquids for pain
- Encourage good hand hygiene to prevent spread
- Some recommend Magic Mouthwash/oral lidocaine if not tolerating PO intake, although evidence suggests no better than placebo[1]
- In infants, do NOT use oral lidocaine due to risk of lidocaine toxicity and FDA black box warning[2][3]
Disposition
- Discharge
- Admit for dehydration or development of complications[4]
Complications
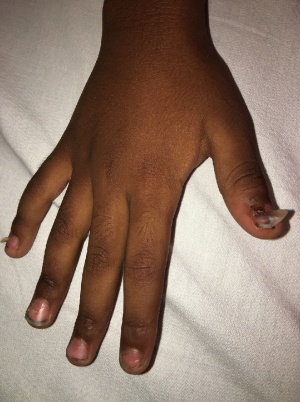
- Some children get a desquamation of the nails around 2 weeks afterwards (self resolves)
- Meningitis and encephalitis are uncommon, yet still possible complications[5]
See Also
External Links
https://pedemmorsels.com/severe-hand-foot-mouth-disease/
References
- ↑ Hopper S. et al. Topical lidocaine to improve oral intake in children with painful infectious mouth ulcers: a blinded, randomized, placebo-controlled trial. Ann Emerg Med. 2014 Mar;63(3):292-9
- ↑ FDA recommends not using lidocaine to treat teething pain. http://www.fda.gov/Drugs/DrugSafety/ucm402240.htm
- ↑ Curtis LA, Dolan TS, Seibert HE. Are one or two dangerous? Lidocaine and topical anesthetic exposures in children. J Emerg Med 2009;37:32-39
- ↑ https://www.aafp.org/afp/2019/1001/p408.html
- ↑ Bonfante G and Rosenau AM. Rashes in Infants and Children: in Tintinalli JE, Stapczynski S, et al (eds): Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, ed 7. McGraw-Hill, 2011. Ch (134).