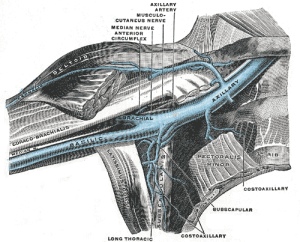
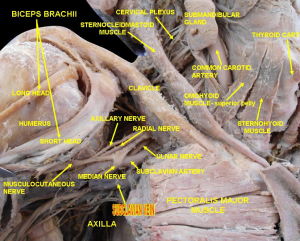
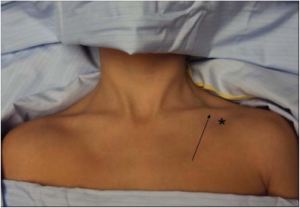
Central line: subclavian
Indications
- Central venous pressure monitoring
- Administration of multiple medications and drips
- High volume/flow resuscitation[citation needed]
- Emergency venous access
- Inability to obtain peripheral venous access
- Repetitive blood sampling
- Administering hyperalimentation, vasopressors, caustic agents, or other concentrated fluids
- Insertion of transvenous cardiac pacemakers
- Hemodialysis or plasmapheresis
- Insertion of pulmonary artery catheters
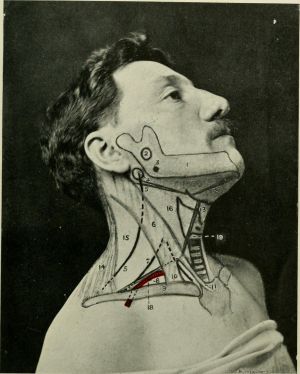
Anatomy of lateral neck: 1. The inferior maxilla. 2. The inferior alveolar nerve. 3. The tonsil. 4. The transverse process of the atlas. 5. The spinal accessory nerve. 6. The sterno-mastoioid muscle. 7. The upper limit of the brachial plexus. 8. The third part of the subclavian artery. 9. clavicle. 10. The clavicular head of thesterno-mastoid muscle.)
Contraindications
Absolute[1]
- Infection over the placement site
- Anatomic obstruction (thrombosis of target vein, other anatomic variance)
- Site-specific
- Subclavian - trauma/fracture to ipsilateral clavicle or proximal ribs
Relative
- Coagulopathy (see below)
- Distortion of landmarks by trauma or congenital anomalies
- Prior vessel injury or procedures
- Morbid obesity
- Uncooperative/combative patient
Central line if coagulopathic
- Preferentially use a compressible site such as the femoral location (avoid the IJ and subclavian if possible, though IJ preferred over subclavian)
- No benefit to giving FFP unless artery is punctured[2]
- However, consider giving FFP if patient has hemophilia[3]
Equipment Needed
- CVC kit typically contains:
- Chlorhexidine
- Sterile drape
- 1% lidocaine without epinephrine
- 5 mL syringe (for lidocaine)
- 22-ga and 25-ga needles (for lidocaine)
- 5-10 mL syringe (for venipuncture)
- 18-ga needle (for venipuncture)
- Guidewire
- Scalpel with 11-blade
- Dilator
- Triple-lumen catheter (or introducer catheter/Cordis)
- Catheter clamp
- Silk suture
- Sterile gown, cap, mask, gloves
- Biopatch
- Tegaderm
- Sterile saline flush
- Sterile caps for lumen ports
Procedure (Infraclavicular approach)
- Obtain informed consent when possible
- Supine position, arm adducted
- Don cap, mask, sterile gown and gloves
- Chlorhexidine prep the skin. Right sided approach preferred
- Place sterile drape over target area
- Anesthetize insertion site, including periosteum of clavicle
- Prepare catheter by flushing each lumen with sterile saline
- Prepare the guide wire by sliding the plastic sleeve slightly forward to straighten the curved wire tip
- Locate insertion site at junction of middle and medial thirds of the clavicle.
- Orient the bevel of the needle inferomedially to direct the wire inferiorly
- Insert needle with syringe toward the suprasternal notch, while applying negative pressure on the syringe
- Advance needle until it hits clavicle, then walk the needle down until it is able to pass posterior to the clavicle. (Other recommended approach is to insert needle slightly more lateral which can avoid "walking the needle" down the clavicle)
- When the needle enters the lumen, blood will be aspirated freely
- Stabilize the needle hub, carefully remove the syringe from the needle
- Confirm blood flow is non-pulsatile. Cap needle hub with thumb to avoid air embolism
- Insert the guidewire in through the needle hub, never letting go of the wire. If resistance is met, remove the wire and aspirate with syringe to confirm placement still in the vessel
- Remove the needle, keeping the wire in the vessel
- Make a small incision to facilitate dilator passage through the skin
- Thread the dilator over the wire, and advance several centimeters into the vessel, then remove, while keeping the wire in the vessel
- Advance the catheter over the wire, until the wire protrudes from a distal port (For introducer catheters, the dilator and larger single-lumen catheter are inserted as a dilator-sheath unit, assembled prior)
- Grasp the wire where it emerged from the port and advance the catheter into the vessel
- Remove the wire
- Place end cap on port
- Withdraw blood then flush each port/lumen with saline
- Suture the catheter in place
- Place Biopatch
- Cover with Tegaderm
Complications
- Arterial puncture and hematoma
- Pneumothorax
- Hemothorax
- Vessel injury
- Air embolism
- Cardiac dysrhythmia
- Nerve injury
- Infection
- Thrombosis
- Catheter misplacement
- Bleeding
See Also
Vascular access types
- Central venous catheterization
- Rapid infusion catheter
- Intraosseous access
- Venous cutdown
- Umbilical vein catheterization
- Ultrasound assisted peripheral line placement
- External jugular vein cannulation
- The "Easy IJ"
- Midlines
External Links
- Merk Manual - How To Do Infraclavicular Subclavian
- Merk Manual - How To Do Infraclavicular Subclavian (Ultrasound-Guided)
Videos
{{#widget:YouTube|id=IerJcgPb0N4}}
References
- Roberts & Hedges 6e, pp 397-431
- ↑ Graham, A.S., et al. Central Venous Catheterization. N Engl J Med 2007;356:e21
- ↑ Fisher NC, Mutimer DJ. Central venous cannulation in patients with liver disease and coagulopathy—a prospective audit. Intens Care Med 1999; 25:5
- ↑ Morado M.et al. Complications of central venous catheters in patients with haemophilia and inhibitors. Haemophilia 2001; 7:551–556