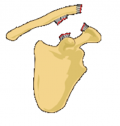
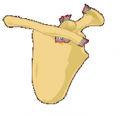
Acromioclavicular joint injury
(Redirected from Acromioclavicular injuries)
Background
- Occurs via direct trauma to the adducted shoulder
- Accounts for 40% of all shoulder injuries and 10% of all injuries in collision sports (football, hockey, etc.)[1]
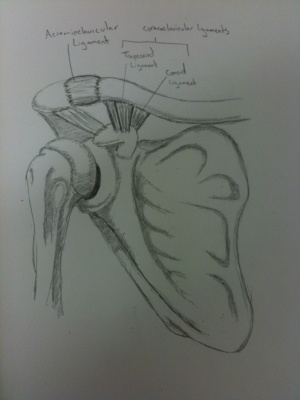
- Acromioclavicular (AC) and coracoclavicular (CC) ligaments may be affected
- Routine use of stress radiographs is controversial (low yield)
Clinical Features
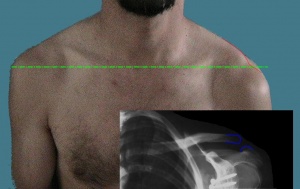
- Tenderness directly over AC joint (with possible deformity)
- AC compression test
- Passively flex arm so It is parallel with ground; then passively adduct across body
- Pain suggests AC joint injury
- Passively flex arm so It is parallel with ground; then passively adduct across body
- Ability to touch contralateral shoulder with injured arm suggests lack of shoulder dislocation
Differential Diagnosis
Shoulder and Upper Arm Diagnoses
Traumatic/Acute:
- Shoulder Dislocation
- Clavicle fracture
- Humerus fracture
- Scapula fracture
- Acromioclavicular joint injury
- Glenohumeral instability
- Rotator cuff tear
- Biceps tendon rupture
- Triceps tendon rupture
- Septic joint
Nontraumatic/Chronic:
- Rotator cuff tear
- Impingement syndrome
- Calcific tendinitis
- Adhesive capsulitis
- Biceps tendinitis
- Subacromial bursitis
- Cervical radiculopathy
Refered pain & non-orthopedic causes:
- Referred pain from
- Neck
- Diaphragm (e.g. gallbladder disease)
- Brachial plexus injury
- Axillary artery thrombosis
- Thoracic outlet syndrome
- Subclavian steal syndrome
- Pancoast tumor
- Myocardial infarction
- Pneumonia
- Pulmonary embolism
Evaluation
Workup
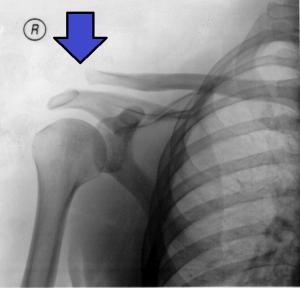
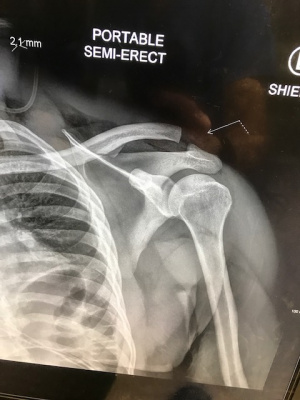
- AP shoulder (highly consider comparison view)
- AC joint
- Normal width of AC joint in adults is 1-3mm
- By age 60 width is often less than 1mm
- Children and adolescents have a slightly wider joint space
- CC joint
- Normal distance is 11-13mm
- Comparison to opposite CC joint space is more important
- Increase in CC distance of 25-50% indicates complete CC ligament disruption
- Zanca view (AP with 10-15 degree cephalic tilt)
- Consider if AP view is ambiguous, concern for type II injury or distal clavicle injury
- Axillary view
- Obtain if coracoid tenderness is present to rule-out associated coracoid fracture
- Helps to confirm ant-post position of clavicle in injury types III-IV
- AC joint
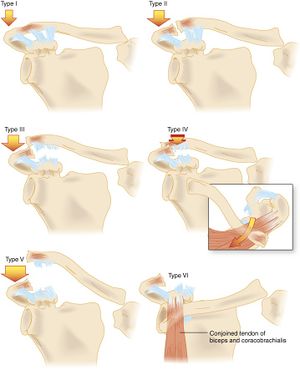
Diagnosis
| Classification | Anatomic Injury | Exam | X-ray | Image |
| Type I |
|
|
|
|
| Type II |
|
|
|
|
| Type III |
|
|
|
|
| Type IV |
|
|
|
|
| Type V |
|
|
|
|
| Type VI |
|
|
Management
Type I
- Rest, ice, sling
- ROM and strengthening exercises as soon as tolerated
- Return to sport or work is limited only by pain
Type II
- Rest, ice, sling x 3-7 days
- ROM and strenghtnening exercises as soon as tolerated
- Return to sport or work once full ROM and strength are regained
Type III
- Rest, ice, sling x2-3 weeks
- ROM and strengthening exercises as soon as tolerated
- Return to sport or work 6-12 weeks following injury
- Ortho consultation within 1 week
Types IV-VI
- Require orthopedic evaluation; emergent if neurovascular compromise exists
- Generally operative
Disposition
- Admission Criteria
- Neurovascular compromise
- Open or unstable fractures
- Admission for operative repair may be needed for Types IV, V, and VI
- Discharge Criteria
- Type I/Type II may be discharged with orthopedic follow-up
- Type III may be discharged with urgent orthopedic follow-up
See Also
References
- ↑ Sirin E, Aydin N, Mert Topkar O. Acromioclavicular joint injuries: diagnosis, classification and ligamentoplasty procedures. EFORT Open Rev. 2018;3(7):426-433. Published 2018 Jul 17. doi:10.1302/2058-5241.3.170027