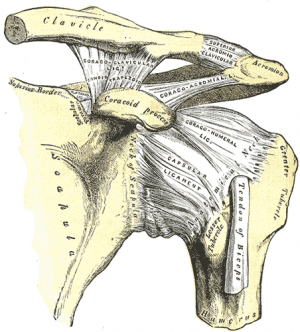
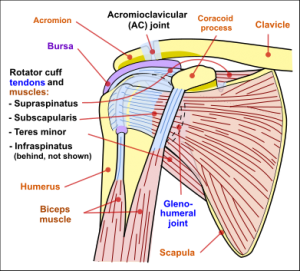
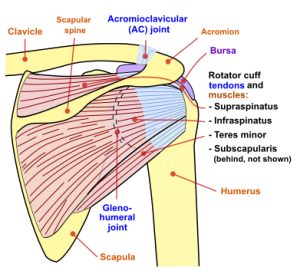
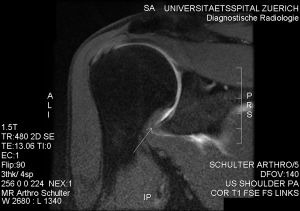
Adhesive capsulitis
Background
- Also known as "frozen shoulder syndrome"
- Inflammation of glenohumeral joint → joint capsule fibrosis, shoulder restriction
- Must rule-out posterior shoulder dislocation
- Associated with:
- Impingement Syndrome
- Postmenopause
- DM
- Thyroid disease
- Pulmonary neoplasm
- Autoimmune
Clinical Features
- Hallmark is limited active and passive range of motion
- Shoulder pain
- Diffuse, aching, poorly localized, accompanied by stiffness, worse at night
- Not typically reproducible by palpation
| Stage | Category | Timeline (months) | Findings |
|---|---|---|---|
| 1 | Acute | 2-3 | Acute synovial inflammation with limitation of shoulder movement due to pain |
| 2 | Freezing | 3-9 | Decreased shoulder motion due to capsular thickening/scarring; patient has chronic pain |
| 3 | Frozen | 9-15 | Less pain, but significantly decreased range of motion |
| 4 | Chronic | >15 | Minimal pain, progressive improvement in shoulder range of motion |
Evaluation
- Clinical diagnosis, consider X-ray to rule out fracture/dislocation
Differential Diagnosis
Shoulder and Upper Arm Diagnoses
Traumatic/Acute:
- Shoulder Dislocation
- Clavicle fracture
- Humerus fracture
- Scapula fracture
- Acromioclavicular joint injury
- Glenohumeral instability
- Rotator cuff tear
- Biceps tendon rupture
- Triceps tendon rupture
- Septic joint
Nontraumatic/Chronic:
- Rotator cuff tear
- Impingement syndrome
- Calcific tendinitis
- Adhesive capsulitis
- Biceps tendinitis
- Subacromial bursitis
- Cervical radiculopathy
Refered pain & non-orthopedic causes:
- Referred pain from
- Neck
- Diaphragm (e.g. gallbladder disease)
- Brachial plexus injury
- Axillary artery thrombosis
- Thoracic outlet syndrome
- Subclavian steal syndrome
- Pancoast tumor
- Myocardial infarction
- Pneumonia
- Pulmonary embolism
Management
- Avoid immobilization
- Physical therapy
- Analgesia
- Oral steroids
- Provide significant short-term benefit in terms of relieving pain and improving ROM
- Intra-articular steroids (20-40mg triamcinolone)
- Benefits last a few months, possibly up to 6 months[1]
- Joint distention
- Intra-articular distention with 25-40mL of saline + anesthetic is as effective as IA steroids[2]
Disposition
- Discharge, refer to primary care/ortho for physical therapy
See Also
External Links
References
- ↑ Sun Y, Zhang P, Liu S, et al. Intra-articular Steroid Injection for Frozen Shoulder: A Systematic Review and Meta-analysis of Randomized Controlled Trials With Trial Sequential Analysis. Am J Sports Med. 2017;45(9):2171-2179.
- ↑ Lin MT, Hsiao MY, Tu YK, Wang TG. Comparative Efficacy of Intra-Articular Steroid Injection and Distension in Patients With Frozen Shoulder: A Systematic Review and Network Meta-Analysis. Arch Phys Med Rehabil. 2018;99(7):1383-1394.e6.