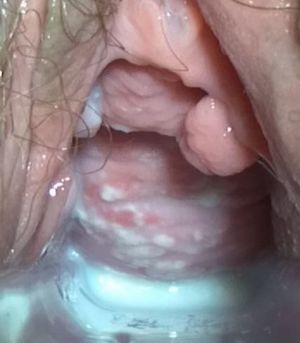
Candida vulvovaginitis
Revision as of 15:32, 27 October 2016 by Neil.m.young (talk | contribs) (Text replacement - "* " to "*")
Background
- Local fungal infection caused by the Candida genus
- Most commonly seen in females in high estrogen states: pregnancy, oral contraceptive use, obesity, diabetes mellitus
- Not considered an STI although it can be transmitted by sexual intercourse
- May occur in premarnarcheal girls (rare)
Types
- Uncomplicated
- Sporadic infectionn
- mild-moderate symptoms
- due to Candida albicans
- immunocompetent
- Complicated
Clinical Features[1]
- Vulvar pruritus - most common and specific symptom
- Vaginal discharge - varies from little to copious and from watery to cottage-cheese like
- Malodorous smell is unusual (if present favors diagnosis of Bacterial vaginosis)
- intense vulvovaginal pruritus or burning
- dyspareunia
- dysuria
Differential Diagnosis
Vulvovaginitis
- Bacterial vaginosis
- Candida vaginitis
- Trichomonas vaginalis
- Contact vulvovaginitis
- Bubble baths and soaps
- Deodorants, powders, and douches
- Clothing
- Atrophic vaginitis due to lack of estrogen (AKA Vulvovaginal atrophy)
- Lichen sclerosus
- Tinea cruris
- Chlamydia/Gonorrhea infection
- Pinworms
- Vaginal foreign body
- Toilet paper
- Other
- Genitourinary syndrome of menopause
- Foreign body
- Allergic reaction
- Normal physiologic discharge
Evaluation
Work-up
- Wet mount - shows hyphae and yeast buds
- Candida does not cause WBCs on wet mount → if present, consider co-infection with other vaginitides or STI
- If recurrent, consider checking blood glucose for occult DM
Diagnosis
- although other candida infections are clinically diagnosed, laboratory methods should be pursued to confirm diagnosis of candida vulvovaginitis
- cotton cheese curd-like non-odorous vaginal discharge on pelvic exam
- vaginal pH < 4.5
- vaginal wet mount
Management
- Do not treat if asymptomatic
- Sexual partners should not be treated unless the patient has frequent recurrences
- Antifungal[2]
- 1st line: Oral Fluconazole
- Pregnant: Topical imidazole (clotrimazole, miconazole)
Antifungals
Uncomplicated
There is little resistance to azole medications; treatment often dictated by patient preference.
- Fluconazole 150mg PO once[2]
- Intravaginal therapy
- Clotrimazole 1% cream applied vaginally for 7 days OR 2% applied vaginally for 3 days
- Miconazole 2% cream applied vaginally for 7 days OR 4% cream x 3 days
- Butoconazole 2% applied vaginally x 3 days
- Tioconazole 6.5% applied vaginally x 1
Complicated
Severe or immunosuppressed
- Fluconazole 150mg PO q72h x 3 doses
Non-albicans species
- For example, C. glabrata, C. krusei and other atypical Candida spp.
- Boric acid vaginal suppository intravaginal qday x ≥14 days
- Can be fatal if taken orally
- If empirically treated and later is found to have non-albicans Candida spp., no change in therapy is needed if patient is improving (otherwise switch to boric acid.
Recurrent (≥ 4 infections in a year)
- Treat as for uncomplicated (see above)
- Once therapy completed, prescribe long-term treatment
- Fluconazole 150mg PO qweek x 6 months OR
- Intravaginal medication, such as clotrimazole 500mg PV qweek or 200mg PV twice a week
Pregnant Patients
- Intravaginal clotrimazole or miconazole are the only recommended treatments
- Duration is 7 days
- PO fluconazole associated with congenital malformations and spontaneous abortions[3]
Disposition
- Outpatient
See Also
References
- ↑ Kauffmann CA. Overview of Candida Infections. UptoDate. 2016.
- ↑ 2.0 2.1 Pappas PG, Kauffman CA, Andes DR, et al. Clinical Practice Guideline for the Management of Candidiasis: 2016 Update by the Infectious Diseases Society of America. Clin Infect Dis 2016; 62:e1.
- ↑ Molgaard-Nielsen D et al. Association Between Use of Oral Fluconazole During Pregnancy and Risk of Spontaneous Abortion and Stillbirth. JAMA. 2016;315(1):58-67.