WLAVA:COVID19 ED Operational Updates: Difference between revisions
Mceledon83 (talk | contribs) |
Mceledon83 (talk | contribs) |
||
| Line 18: | Line 18: | ||
==WLA ED Workflow== | ==WLA ED Workflow== | ||
*'''Please have a low threshold to place isolation orders early on patients in whom you suspect COVID-19''' | *'''Please have a low threshold to place isolation orders early on patients in whom you suspect COVID-19''' | ||
* | *''WLA ED COVID19 Suggested Workflow'' ([[File:WLAVA COVID - ED Flow - v03-20-20v.2.pdf|WLAVA COVID ED Flow 03.20.20]]) | ||
==ED Attending Shift Responsibilities== | ==ED Attending Shift Responsibilities== | ||
Revision as of 20:36, 31 March 2020
- Website Last Updated 3/31/20
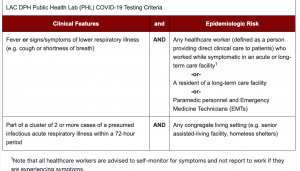
WLA VA ID COVID-19 Testing Algorithm
LAC DPH COVID19 Resources
Definition of COVID19 Person Under Investigation (PUI) updated 3.24.20
- Note that all healthcare workers are advised to self-monitor for symptoms and not report to work if they are experiencing symptoms.
LAC DPH COVID19 Physician Checklist
LAC DPH Home Isolation Handout
WLA ED Workflow
- Please have a low threshold to place isolation orders early on patients in whom you suspect COVID-19
- WLA ED COVID19 Suggested Workflow (File:WLAVA COVID - ED Flow - v03-20-20v.2.pdf)
ED Attending Shift Responsibilities
- Extra weekday night and weekend shift coverage has been added to flex to tent and cover airway.
- Airways:
- Anesthesia covers all airways including ED COVID airways from 7a-7p.
- From 7p-7a ED covers all crash airways including COVID ones. A third overnight attending has been added so that two attendings may respond to airways while one remains in the ED.
- 4p-12a fast track attending serves as airway buddy during weekdays.
- Anesthesia can be called for impending airways if 2 hours notice can be given.
- Enhanced Screening Tent:
- EST open M-F 7a-11p and Sa-Su 10a-10p
- EST Schedule (WLA Intranet Only)
- Weekday 4p-mn FT (covers 4p-11p) and weekend FT (covers 10a-5p)
- Weekend main ED 7p-7a attending (covers from 5p-10p)
- please check in with the EST nurses at the start of your shift and leave them your name (so they can reach you by Vocera).
- Please pick up the VA iPad assigned for EST Telehealth so you can see patients using FaceTime (so you don’t have to walk back-and-forth).
- We are still working out if the ED MSA or the ED Charge Nurse will be in charge of EST VA iPad sign in/sign out. This will hopefully be resolved tomorrow.
- See the following WikEM pages for details on the EST mission and protocols:
- EST open M-F 7a-11p and Sa-Su 10a-10p
Whom To Notify of PUIs
- Call GLA ID: UCLA consult p89321.
- Notify LA County Dept of Public Health if directed by ID:
- 213-240-7941 (weekdays 8:30a-5p)
- 213-974-1234 and ask for physician on call (after-hours).
- If admitted, please notify Jonie, Neil, Manny, and Lisa by text if you have a PUI patient.
Misc Numbers:
- Infectious diseases fellow (x40270/40271)
- Microbiology Department (x41259)
PPE Documentation
- Please make sure to document the PPE used in your chart as it will allow us to track your exposure category and will help us guide work restrictions.
Ordering COVID-19
- Influenza/COVID-19 is the new order (no RP2 testing).
- Must call ID for COVID-19 testing approval.
- In-house testing available with TAT 1-4 days.
- We are only collecting one nasopharyngeal swabs per patient.
- Current COVID-19 ordering protocol:
- Patient presents with possible need for COVID testing (perhaps a healthcare worker)
- Tent/ED provider order Flu/COVID-19 in CPRS (this is when ID should be called)
- Nurse swabs NP x 1, send to lab.
- If Flu results negative, the patient may need COVID testing.
- Micro contacts ID if Flu is negative (not a consistent process, so please confirm for now)
- The COVID-19 test is done if ID approves
- Lab processing is not automatic at VA, until all the kinks get ironed out with ordering COVID-19, please continue to follow the Flu results on these patients
- At least double check to see if COVID-19 was added by lab (ID will f/u COVID-19 results) to ensure the testing you want is occurring.
AVOID AEROSOLIZING Procedures (if Possible)
- Do not use NEBS - use MDI/SPACER (we have some in stock- if not in FT- check main ED)
- NO to High flow NC (generally - if done place a surgical mask on patient)
- NO to BIPAP
- Intubate early & in a negative pressure room
- AVOID any bagging
COVID-19 Admission Guidelines
- Please have low threshold to admit patients to higher level of care or discuss cases with MOD.
- Draft of COVID-19/PUI Triage Guidelines:
- Draft of COVID-19/PUI Triage Guidelines:
- Most COVID Admissions will go to MICU Team
- If they are critical, they go to the ICU under MICU. If they are meta-stable, then go to the new 5SD "COVID" Unit, but still under MICU team
- The 5SD "COVID" unit is a newly converted unit with 10 negative pressure rooms.
- New Isolation Note
- Specific to COVID19 - indicate if ICU level of care and high risk for aerosolizing procedures vs usual care.
COVID-19 Direct Admission Guidelines
- Same as our previous direct admission policy.
- Patients in clinic can be admitted directly if stable and clinic is still open.
- Provider that made admission disposition decision must call MOD/OTS for coordination.
- If patient coming from home, provider can still call MOD/OTS. Holding area will be Tent if there is not immediate inpatient bed available.
CODE Situation for COVID-19 Cases
- DO NOT be a hero and RUSH IN
- PPE: N95, Face Shield, bouffant, gloves x2 and gown x2
- Place a surgical mask on patient while getting airway set up, chest compressions ok
- Do not BAG patient
- Limit # of staff
- Staff safety is #1 PRIORITY
Official GLA PPE Recommendations
Last Updated 3.21.20
PPE for Suspected COVID-19 Patients: Critically Ill or Aerosolizing Procedures
- Airborne
- Droplet
- Contact precautions (with eye protection)
- Negative pressure room (if available)
- Critically ill (i.e., receiving ICU-level care)
- Eye protection (face shield or goggles)
PPE for All Other Suspected COVID-19 Patients
- Standard
- Droplet
- Contact precautions (with eye protection)
- Eye protection (face shield or goggles)
Radiology COVID-19 and PPE
- Very low threshold for placing facemask on patients with respiratory symptoms or symptoms potentially concerning for COVID.
- All patients with respiratory symptoms are supposed to have this anyway, but we may have to enforce further
- In the current climate, portable CXRs generally preferred (especially for respiratory symptoms)
- Very low threshold for staff wearing face masks whenever interacting directly with patients including when obtaining XRs
- Make sure patients are wearing face mask properly if they are sent down to imaging (Remind transport to check face mask).
- We can do portable CXRs in Fast Track if either the patient is in a bed (Room D only) or the patient is very compliant and able to sit still in our exam chairs without risking dropping the cassette.
Updates on GLA ED Supply of PPE
- Please do not mark PAPR hoods with your name. We are going to be using them indiscriminately based on your size.
- We secured a limited supply of Inner Hoods with neck covering for use with PAPR.
inner
- We secured a limited supply of special PAPRS with Hood with neck covering.
- There is only one in the airway cart and one in the Med Room.
- Bunny Suit - comes in 3 sizes (located in Med Room).
- Zahir had a great idea about buying protective goggles for our nurses/ICTs. The idea is to buy onefor yourself and one for a nurse/ICT. No pressure, $13.00 on Amazon.
Reusing PPE
- PAPR hoods - Used PAPR hoods are now community property amongst ED staff since they are being cleaned by SPS (will be labeled ER).
- Cleaning Eye Protection:
- Perform hand hygiene
- Put on gloves
- Use an alcohol wipe across the entire INNER surface
- Use a hospital disinfectant (SaniWipe AF3) to wipe the entire OUTER surface
- Allow to air dry
- Place in brown paper bag till next use
- Remove gloves and perform hand hygiene
- GLA Infection Control Reference file:
File:APPROVED 20200330.1030.Interim GLA guidance for Eye Protection Cleaning.pdf
GLA Main Contact For Official PPE Purchasing (Not Donations)
- Terry Wolgamott
GLA Contacts for PPE Donations
- If you know someone who is interested in donating masks, or other items, to our medical center please have them contact our Voluntary Service dept.
- Alexia Lunningham, Chief of Voluntary Service: Alexia.Lunningham@va.gov or 310-286-3994
- Shirley Bearden, Voluntary Service Specialist: Shirley.Bearden@va.gov or 310-268-3194
Close Contact Definition
- Being within approximately 6 feet (2 meters) of a confirmed COVID-19 case for a prolonged period (5 minutes)
- Having unprotected direct contact with infectious secretions of a COVID-19 case.
- NOTE: Examples of Brief Interactions include:
- Briefly entering the patient room without having direct contact with the patient or their secretions/excretions.
- NOTE: Examples of Brief Interactions include:
NOT Close Contact Definition
- Brief conversation at a triage desk with a patient who was not wearing a face mask.
- These encounters are NOT close contacts, except when an aerosol-generating procedure is or has been recently performed.
Patient Placement
- Patients with suspected or confirmed COVID-19 disease will be cared for in single rooms with the door closed.
- Airborne isolation rooms (negative pressure rooms) will be used for patients with suspected or confirmed COVID-19 disease who
- Are receiving ICU-level care OR
- Undergoing procedures that are likely to generate a high concentration of respiratory aerosols.
- NOTE: If negative pressure rooms are unavailable for a patient receiving ICU care, patients will be placed in a standard room with staff using N95 with eye protection/PAPRs, gowns and gloves. If hospitalization is not medically needed, home care is preferable if the individual’s situation allows.
Aerosol-generating procedures
- Endotracheal intubation or extubation
- Cardiopulmonary resuscitation
- Non-invasive positive pressure ventilation (BiPAP)
- Bronchoscopy
- Open oropharyngeal or nasopharyngeal suctioning (closed circuit suctioning is considered non-aerosol generating)
- Nebulizer therapy. Use of metered dose inhalers with spacers is strongly preferred for patients being tested for or diagnosed with COVID-19.
- NOTE: The number of healthcare workers present during the procedure should be limited to only those essential for patient care and procedure support. Visitors should not be present for the procedure.
COVID-19 Specimen Collection (Nasopharyngeal Swabs)
- Standard/Contact/Droplet precautions are recommended.
- The number of persons present during the procedure should be limited to only those essential for patient care and procedure support. Visitors should not be present for specimen collection.
- Specimen collection can be performed in a normal examination room with the door closed.
Patient Transport in the Hospital
- If transport personnel must prepare the patient for transport (e.g., transfer them to the wheelchair or gurney), transport personnel should wear all recommended PPE.
- Patients should wear a face mask to contain secretions during transport. If patients cannot tolerate a face mask or one is not available, they should use tissues to cover their mouth and nose.
- The transporter should wear a face mask.
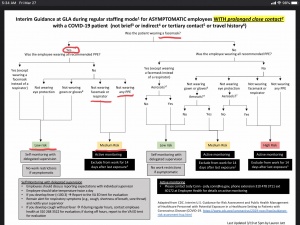
GLA Provider Exposure Risk Algorithm
- Please protect yourself from inadvertent exposure by making sure patients that have any hint of being a potential PUI (i.e., epidemiological risk factors, URI sx, any respiratory sx, etc.) are wearing a face mask (can use conical or level 1/yellow mask).
- Reviewing the exposure risk algorithm shows that this simple intervention keeps exposure risk low to medium.
- Second layer of defense is ensuring that you wear a face mask (NOT N95).
- File:20200319.1700.Interim GLA guidance for healthcare monitoring.pdf
General PPE Training
- PPE training 3/17 to 4/17 @ 8:30a - 4:00p Bldg 500, Rm 6043 (no reservation required)
SIM Lab Training
- Email Cindy Koh or Carol Lee.
FIT Testing
- To clarify, you need to be FIT tested yearly at each facility you work because the brand and type of mask may be different. Your face may change shape with age/weight/pregnancy etc...
- FIT Testing Sessions:
- Fit testing for Full face mask (WW2 gas mask looking thing) Wedneday April 1 12p-2p rm 3232.
- Please complete online form prior to training:
- URL: http://respiratormedicalevaluation.com
- Organization Code: vala
N95 Mask at GLA
- Stored in Med Room (badge access only)
- GLA N95 Brand/Model:
- We primarily carry: 3M 1870+
- We have a stock of small masks: 3M 1860S
GLA Donning & Doffing Checklist
Last Updated 3.20.20 N95
- N95 Donning & Doffing (File:PPE Donning.Doffing Checklist ER 2020 N95 - final 3.20.pdf)
- N95 D&D Flowchart (File:GLA VA ED Physician Flowsheet.N95&ok.pdf)
PAPR
- PAPR Donning & Doffing (File:PPE Donning Checklist ER 2020 airway PAPR - 3.26_jh.pdf)
- PAPR D&D Flowchart (File:GLA VA ED Physician Flowsheet.PAPR.pdf)
GLA Showers
- No Lockers - Bring your own towel/clothes
Airway Cart x 2 & COVID-19 Attending (3rd Overnight 11a-7p) Restocking Responsibilities
- Reference document:
- New Airway carts are located across from MD station/Rm 6-7. These have PAPR, PPE, and airway equipment including viral filters.
- Code is 1212
- In an airway emergency - grab cart, Glidescope Go and a bag of disposable meds in the MED ROOM, and PAPR hood if reused.
- PAPR, belt, tube, and hood are REUSABLE only the plastic cover over breathing tube is disposable.
- Clean PAPR hoods thoroughly with sani-wipes when doffing to decease pathogens.
- PAPRs and the Paprs hoods will be cleaned by SPS so after you are done using it, place in a biohazard bag and leave it in the dirty Utility room of the actual Unit where you intubated.
- Contact SPS M-F 41811, Weekends 310-987-8710 or 323-497-4585. They will pick up, clean and deliver back to ED.
3rd Overnight 11p-7a (COVID-19) Attending Duties:
- Airway management for crash COVID patients.
- At the beginning of the shift, please go through the airway cart and make sure everything is stocked in the right numbers. A list will be provided in the cart.
- Help other attendings with ED patient load.
- If you cannot find an item, email Derrick, Miguel, Lisa and Jonie.
Mock Code Drills
- If you are having a slow shift, please consider running a few mock code drills so that we can ensure our nursing staff is well prepared. Our nursing staff is a little rusty when it comes to critical care, so it isbetter we iron out any issues in preparation for the future.
- Hospitalists are doing daily weekday drills (M-F) at 11AM in 3rd floor conference room (there will be no overhead announcements).
- Reference Documents:
Your Health (and Ours)
- If you develop a fever and/or resp symptoms- notify Neil/Jonie immediately. We know how hard y'all want to work - but it's important to stay healthy and keep away from others to avoid further spread of disease to coworkers and patients and additional need for quarantine.
CDC Return to Work Guidance
- Guidance on what to do if you think you were exposed to COVID-19 and are asymptomatic:
- We are using the CDC updated recommendations on public health management of healthcare personnel (HCP) with potential exposure in a healthcare setting to patients with COVID-19 (see below). This updated guidance allows for asymptomatic HCP who have been exposed to a COVID-19 patient to continue to work AFTER consultation with their occupational health program (see table below for details on exposure risk).
- We are counting on your self-referral.
Miscellaneous Admin
Detaining PUI or COVID19 Confirmed Patients
- It seems that without any specific quarantine order (rare that we will have an official order on our patients)- we cannot detain patients against their will unless we do not think they have capacity- which is a separate issue.
Medical Student & Resident Rules Regarding PUI Pt Care
- Medical students SHOULD NOT participate in any care for COVID — so they don’t spread in their community.
- Residents ok to see PUI patient, but no intubations (includes anesthesia residents).
- Official GLA Housestaff Policy on Residents Caring for COVID-19 Patients:
Coding COVID19 Encounters
- For suspected COVID19 cases: Z20.828
- For confirmed COVID19 cases: B97.29
Dexter Moved Out
- Use ‘UM Review’ label on EDIS to communicate with him.
- If you are interested in not having to change your admission orders 50 times.
- Here are ways to contact me if you have questions:
- VA cell: 626 314 9774
- VA Pager *11 p73284
- Here are ways to contact me if you have questions:
GLA Sites
- Links to GLA COVID19 documents and resources (https://dvagov.sharepoint.com/sites/VHAGLAMed/ed/default.aspx)
- VA screening scripts and resources (https://dvagov.sharepoint.com/sites/VACOVHAPublicHealth/HCI/SitePages/Home.aspx)
Emergency Alerting and Accountability System (EAAS)
- If you wish to receive alerts from the VA EAAS (https://alerts7.athoc.com/SelfService/VAEAAS)
- Any issue please contact Lonnie Miller at x40863
Other WLA VA Pages