WLAVA:Enhanced Screening Tent
Last Updated: 7/23/20
MISSION OF EST
- The mission of the tent is to rapidly triage ambulatory patients presenting to WLA VA MC that failed primary COVID-19 screen when attempting to enter the medical center or who presented directly to EST.
- This is not a clinic that provides a comprehensive evaluation but we can facilitate coordination of urgent telehealth visits.
- We want to avoid having low acuity (otherwise well) symptomatic patients wandering Building 500.
- Try to complete the visit for patient out in the EST. For example
- If came to GLA for a medication refill, call Pharmacy and have an EST runner go pick up the meds.
- If came for a specialist appointment, page the on call team to help them coordinate a telehealth visit or come and evaluate the patient out in the EST.
- Try to complete the visit for patient out in the EST. For example
EST PROVIDER DISPOSITION TOOL
EMPLOYEE SYMPTOM SELF-REFERRAL TOOL
EST PROVIDER ORIENTATION CHECKLIST
EST Provider Schedule
EST Provider Schedule (VA Intranet Only)
EST TELEHEALTH (No EST Provider Scheduled)
WLAVA:Enhanced_Screening_Tent_Telehealth
TENT SKYPE LINK (Remote Accessible)
- Have EST provider log into WOW in Room 3 at beginning of every shift.
- Load Skype chatroom using this link.
- Call ED attending to join chatroom via same link (using Skype for business on phone, ipad, or laptop).
EST PHONE EXTENSIONS
- 310-478-3711
- EST Main x53333 (310-268-3333)
- RN Tent screener 1 x41034
- RN Tent screener 2 x41035
- EST Provider x41075
DIRECT ADMISSIONS OR ADMISSIONS FROM EST
- Stable patients can be admitted from the EST if there is no need for an acute medical intervention.
- Call MOD VA pager 99511
- GMED admissions: UCLA pager p89082
- MICU admissions: UCLA pager p89081
Direct Admission Scenarios
- Provider making admission disposition is in charge of coordinating with OTS and MOD to notify the admission team and give sign out.
- Stable COVID19 patient coming from home should go directly to inpatient bed, but can go to tent if there is no open bed available upon patient arrival.
- Stable COVID19 patient that is being admitted from outpatient clinic, should wait in private room in clinic until they are assigned a bed. If the clinic ends and patient not assigned a bed, then patient is sent to tent as a holding area.
- Stable COVID19 patient seen in the EST that requires admission, EST provider will call MOD to coordinate admission process.
DIRECT ADMISSIONS TO 214-DOM (UNDOMICILED VETERANS)
- Think of this as a homeless shelter for PUIs with pending COVID test or COVID+. Patients do not need to have substance use issues.
- COVID DOM Checklist (File:COVID-19 B214 ADM-ED.INPT.PACT 04.10.2020.pdf)
- Call ED SW x 40976 for help coordinating with 214-DOM
- Consult social worker
- Make sure patient ruled out for TB with cxr or quant ifn within the past 12 months.
- pCXR an be done in the tent if needed.
- Have it read by ED provider if unable to read own CXR)
- pCXR an be done in the tent if needed.
- Fill out CERS <ATTENDING ATTESTATION-INDEPENDENCE/ELIGIBILITY-CERS PROGRAM>
- Social worker will contact DOM for bed between 8am -10pm. If overnight, will need to be observed
Patient & Staff Safety
- All persons inside of the tent must be wearing at least a Level 1 surgical mask (may not enter tent without a surgical mask).
- We want to minimize the time that patients spend inside the EST so that we minimize their exposure to persons that may have COVID-19.
- Staff safety is a priority and we must help/remind each other maintain proper precautions when involved in direct patient care.
- Also important to ensure that staff break area is clean (do not bring soiled PPE to break area).
How To Keep Yourself Protected
- The virus (SARS-CoV-2) cannot jump on you or go through your intact skin. If you keep a distance and do not touch your eyes, nose, or mouth (mucosa) you will be safe.
- The EST Team has built in multiple lines of defense to keep you safe:
- The 1st line of defense is ensuring that patients are wearing surgical mask appropriately.
- The 2nd line of defense is good/frequent hand washing AND maintaining a safe distance (at least 3 feet) from the patient.
- The 3rd line of defense is wearing a surgical mask and face shield.
- The 4th line of defense is wearing gloves.
- The purpose of gown, bouffant, and shoe covers is to keep your clothes from becoming contaminated. We suggest bringing an extra pair of clothes to change into prior to getting into car (or using disposable scrubs provided by EST Team).
Staff PPE for All Suspected COVID-19 Patients Seen in EST
- Standard
- Droplet
- Contact precautions (with eye protection)
- Eye protection (face shield or goggles)
Close Contact Definition
- Being within approximately 6 feet (3 feet if person is wearing a mask) of a confirmed COVID-19 case for a prolonged period (5 minutes)
- Having unprotected direct contact with infectious secretions of a COVID-19 case.
- NOTE: Examples of Brief Interactions include:
- Briefly entering the patient room without having direct contact with the patient or their secretions/excretions.
- NOTE: Examples of Brief Interactions include:
NOT Close Contact Definition
- Brief conversation at a triage desk with a patient who was not wearing a face mask.
- These encounters are NOT close contacts, except when an aerosol-generating procedure is or has been recently performed.
Aerosol-generating procedures
- Endotracheal intubation or extubation
- Cardiopulmonary resuscitation
- Non-invasive positive pressure ventilation (BiPAP)
- Bronchoscopy
- Open oropharyngeal or nasopharyngeal suctioning (closed circuit suctioning is considered non-aerosol generating)
- Nebulizer therapy. Use of metered dose inhalers with spacers is strongly preferred for patients being tested for or diagnosed with COVID-19.
- NOTE: The number of healthcare workers present during the procedure should be limited to only those essential for patient care and procedure support. Visitors should not be present for the procedure.
COVID-19 Specimen Collection (Nasopharyngeal Swabs)
- Standard/Contact/Droplet precautions are recommended.
- The number of persons present during the procedure should be limited to only those essential for patient care and procedure support. Visitors should not be present for specimen collection.
Patient Transport to the Hospital/ED
- If transport personnel must prepare the patient for transport (e.g., transfer them to the wheelchair or gurney), transport personnel should wear all recommended PPE (surgical mask and face shield at least).
- Patients should wear a face mask to contain secretions during transport. If patients cannot tolerate a face mask or one is not available, they should use tissues to cover their mouth and nose.
Doffing PPE UCLA Video
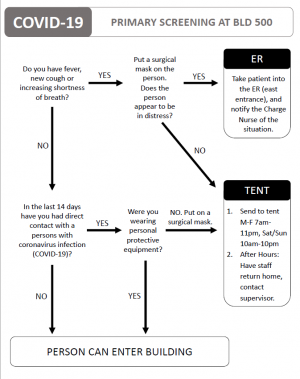
Primary Screen
- Occurs at the entrance to Building 500.
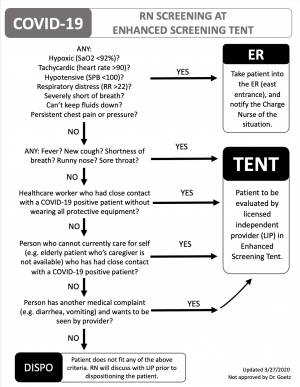
Secondary Screen
- Last Updated: 3/27/20
- Occurs in the first stage tent, completed by RN.
You Will Always Be Supported
- Providers working the tent always have the option to phone a friend:
- ID is on call 24/7 for discussions regarding COVID-19 testing.
- Please review the GLA ID COVID-19 Testing Algorithm prior to discussion with ID
- UCLA Pager 89324 (Call 310-206-8477)
- ED is on call 24/7 for help with disposition of patients if you think you need an ED consult prior to disposition.
- Please have go to Telehealth WOW for ED consult
- x53169 or 310-268-3169
- ED provider would be added as a co-signer on your EST note, if ED provider agrees with disposition decision.
- If ED provider does not agree with your disposition, then send to ED for further evaluation.
- ID is on call 24/7 for discussions regarding COVID-19 testing.
TENT SKYPE MEETING LINK (Remote Accessible)
Minimize Close Contact With Patient
- Staff safety is our primary priority.
- We are a triaging tent, not a comprehensive primary care or urgent care clinic.
- Our job is to ensure that patients are stable enough to wait a few days for a telehealth appointment.
Focus On What Will Change Patient Management
- We are here to rapidly triage and reassure patients/employees.
- We are NOT here to provide a definitive diagnosis.
- The majority of patients can be triaged at a distance using the "eyeball" test (i.e., sick versus non-sick).
- If you are about to touch the patient, always STOP to think "is what I am about to do going to change my management?"
- We encourage empiric treatment/management in the EST.
- For example:
- Patients reported mild dyspnea but they are speaking in full sentences, are afebrile, are not tachypneic, and have unremarkable oxygen saturation on room air.
- The lung auscultation exam is unlikely to change your management, so why expose yourself?
- This patient is likely stable to wait a few days for a formal telehealth evaluation after recommending empiric treatment in EST.
- If you are worried that the patient is wheezing, treat them empirically and discharge them with albuterol.
- If you are worried that the patient has a pneumonia (unlikely if they are afebrile and have unremarkable respiratory vitals) you have the option to treat empirically with antibiotics (dispensed in the tent).
- Patients reported mild dyspnea but they are speaking in full sentences, are afebrile, are not tachypneic, and have unremarkable oxygen saturation on room air.
Help Coordinate Urgent Telehealth F/U
- For assigned patients we use the ED PACT Tool to notify their PCP.
- For unassigned patients we will place a Primary Care Consult AND add lead for the clinic as a cosigner.
Testing for COVID-19
- Please use EST Provider Disposition Tool to check most up-to-date information.
- You always have the option of discussing a case with ID (UCLA Pager 89324) to decide on COVID-19 testing.
- If patient is adamant about testing, despite discussing why testing might not be helpful, go ahead and test the patient.
WLA VA ID COVID-19 Testing Algorithm
- Last Updated 6/26/20
- Reference file (for printing):
File:6.c.i.5_20200624_GLAVA_Algorithm_Triage_OutpatientBldg500.1.pdf
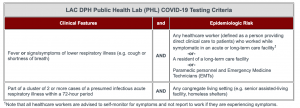
LADPH PUI Criteria
Employee Health (EH) Mission
- We are testing symptomatic employees (and a select few asymptomatic) with a history of exposure to COVID19 for COVID19 if they are involved in direct patient care as it will guide our return to work instructions.
- Please provide all employees with EH handout at discharge.
- If employee was tested for COVID-19 in EST they must be instructed to not go back to work until they are cleared by EH.
- If employee was not tested for COVID-19, they must speak to EH and their supervisor to discuss sick leave and return to work timeline.
- Employee Health (x53522).
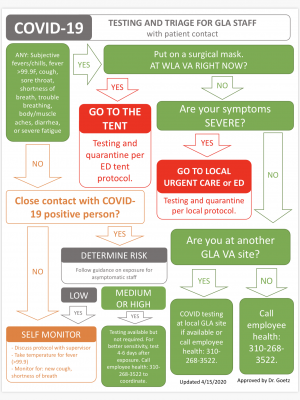
Employee COVID-19 Triage Algorithm
Last Updated: 4/16/20
Employee Exposure Risk Determination Algorithm
Last Updated: 4/17/20
- Reviewing the exposure risk algorithm shows that this simple intervention keeps exposure risk low to medium.
- Second layer of defense is ensuring that you wear a face mask (NOT N95).
EMPLOYEE RETURN TO WORK GUIDANCE
Last Updated: 7/23/20
- Return to work for persons with mild to moderate illness who are not severely immunocompromised:
- At least 24 hours have passed since resolution of fever, if any (without the use of antipyretics) and
- There has been improvement in respiratory symptoms (e.g., cough, shortness of breath) and
- 10 days have passed since the onset of symptoms or time of diagnosis (whichever period is longer)
- All criteria must be satisfied prior to return to work.
- Return to work for persons with severe to critical illness (required O2 or admission) or who are severely immunocompromised:
- At least 24 hours have passed since resolution of fever, if any (without the use of antipyretics) and
- There has been improvement in respiratory symptoms (e.g., cough, shortness of breath) and
- 20 days have passed since the onset of symptoms or time of diagnosis (whichever period is longer)
- All criteria must be satisfied prior to return to work.
- Notes:
- After returning to work, persons with direct patient care responsibilities should always wear a facemask for source control while in the healthcare facility until all symptoms are completely resolved or at baseline. A facemask instead of a cloth face covering should be used by these HCP for source control during this time period while in the facility.
- Reference file:
Suggested Management Algorithm for Patients Presenting to EST
- Use EST Provider Disposition Tool to guide your management of patients presenting to EST.
Clinical Syndromes Associated with Mild COVID-19
- Patients with uncomplicated upper respiratory infection may have non-specific symptoms such as fever, cough, sore throat, nasal congestion, malaise, headache, GI symptoms (n/v/diarrhea), or muscle pain. These patients do not have signs of dehydration (tachycardia, orthostasis), sepsis (2 or more SIRS criteria), or significant dyspnea.
Further Triage of Patients with Dyspnea
- Assessing dyspnea in EST patients:
- Ask the patient to describe the problem with their breathing in their own words, and assess the ease and comfort of their speech. Ask open-ended questions and listen to whether the patient can complete their sentences.
- Ask the following questions:
- Are you so breathless that you are unable to speak more than a few words?
- Are you breathing harder or faster than usual when doing nothing at all?
- Are you so ill that you’ve stopped doing all of your usual daily activities?
- Focus on change. A clear story of deterioration is more important than whether the patient currently feels short of breath. Ask questions like:
- Is your breathing faster, slower or the same as normal?
- What could you do yesterday that you can’t do today?
- What makes you breathless now that didn’t make you breathless yesterday?
- Interpret the breathlessness in the context of the wider history and physical signs. Does the patient have normal vital signs and normal appearance OR do they have abnormal respiratory vital signs and look breathless?
- Ask the following questions:
- Ask the patient to describe the problem with their breathing in their own words, and assess the ease and comfort of their speech. Ask open-ended questions and listen to whether the patient can complete their sentences.
Detailed Provider Orientation
EST Handouts
- Employee Health EST Return to Work Guidance Handout
- Pending COVID-19 LADPH Discharge Instructions for Home Isolation
- LADPH Home Quaratine Guidance for Close Contacts to COVID-19
- LADPH Home Cleaning Instructions
- LADPH Group Living Home Cleaning Instructions
- Provider Work Note
EST Provider Orientation Videos
EST Provider Orientation Videos
Other WLA VA Pages
- WLAVA: COVID19 ED Operational Updates
- WLA VA PPE Main Information Page
- WLAVA: COVID-19 ED Airway Main
- EST Provider Orientation
- WLAVA:Enhanced Screening Tent Telehealth