WLAVA:COVID19 ED Operational Updates
♦♦♦LAST UPDATED 9/27/20♦♦♦
- Please refer to Weekly ED Digest/Newsletter for weekly updates
AEROSOL GENERATING PROCEDURES (AGP) REMINDER
- Coughing/sneezing inside of a private room by a COVID+ or suspected COVID patient is not considered and AGP and therefore does not require terminal clean
- These are the AGPs:
- CPR
- Intubation / Extubation
- Bronchoscopy
- Nebulizer therapy
- Sputum Induction
- Open oro-tracheal suctioning
ACCEPTING TRANSFERS
- ED-to-ED (including LBVA for NSG) – don’t accept calls unless they are coming from our transfer center (M-F 7a-5p; x31448) or OTS (after hours; VA pager 99510 or x53568)
- Confirm who you are talking to prior to taking the call
- if it is not the transfer center or OTS, redirect to transfer center/OTS depending on time of day
- Confirm bed availability
- If patient requires specialist, consult that service prior to accepting the transfer
- Whenever you are unable to reach the resident on call, please use the GLA on-call Sharepoint intranet site to check for up to date contact information and call schedule.
- If you are unable to reach the resident after this, escalate to the Attending -> Service Chief -> Department Chief
- Confirm who you are talking to prior to taking the call
- SNF or clinics – maintain open-door policy for any patient transfers
- Feel free to share your thoughts on their clinical judgment or assist them in their decision making, if warranted, but please keep it professional
- Email (encrypted email pls) vhaglaemchiefs@va.gov with any issues
COVID-19 TRIAGE SCREEN
- Nurses are not reliably providing a warm handoff on patients that screen positive to their triage questions.
- Per Tuesday, RNs will only notify the provider if there is a high suspicion for COVID-19.
- Since this likely to be variable, it is best for us to review this section to make sure they didn’t leave any “landmines” for us.
- If the triage screen is positive the following should occur
- If we agree with the suspicion for COVID-19, we should start enhanced droplet isolation precautions - notify nurse and enter iso note
- If we disagree, document that we reviewed the triage RN COVID-19 screen, why you disagree/don’t need enhanced droplet precautions (i.e., patient has chronic rhinorrhea, was previously COVID+ but now asymptomatic and it has been more than 10-20 days from diagnosis/initial Sx, etc).
COVID+ Screens
- Please try to encourage the charge nurse to room the following patients immediately (if possible)
- Active Resp Symptoms
- Fever with Unclear Etiology
- Noncompliant with mask wear
- Also please remember to review the nursing triage screen and either place the patient in isolation or if the screen is positive, document why you did not place the patient on isolation.
ACCEPTING EST PATIENTS
- Most patients being transferred from the EST to the ED should be going to the ED and roomed directly instead of going to triage. The Main ED doctor will be receiving these calls. Most of these patients are level 3 and are PUIs and we want to keep them contained.
- If the patient is truly a level 4-5, they can be sent to triage but make sure that the FT attending is aware by writing a "ED Transfer Contact Note" to make clear that a handoff has occurred. (Use this note for clinic transfers as well).
INEFFECTIVE PATIENT MASKS
- Please make sure that patients are not wearing ineffective masks.
- Masks ineffective at filtering COVID-19 include
- masks with exhalation valves
- neck gaiters
- bandanas
- Offer these patients surgical masks or a face shield if they refuse to remove their masks.
VIEWING LBVA IMAGING
- Thanks to Jonie for including this in the sharepoint Radiology FAQ page: https://dvagov.sharepoint.com/sites/VHAGLAMed/ed/Radiology/Home.aspx
- You can attempt to retrieve the images directly through IMPAX.
- Click on the Arrowhead all the way to the right and change the location from “system” to “enterprise”.
- This allows search access to VISN 22, which includes LBVA
- Once the correct patient/study is identified, right click the study and select “retrieve”
- It may take a few minutes to load
JLV IS FASTER IN CHROME
- JLV may now be used with Chrome browser and is FASTER
- You can do this by
- Changing your default browser from internet explorer to Chrome
- Creating a JLV bookmark in chrome. Address is https://jlv.med.va.gov/JLV/
- Creating a Chrome Shortcut to JLV on your Desktop
- After logging in on Chrome, click on Chrome settings icon
- Select More Tools Create Shortcut
- Do it the poor man’s way and copy/paste
- Jonie has added a link to the ED homepage
- Other JLV tidbits
- MUSE EKGs are available on JLV
- COVID status is visible at the top
- Self-Identified Gender Identity will display in the demographics widget
ICT SKILLS CLARIFICATION
- In the Main ED ICTs are not allowed to do any procedures and provide primarily as support for nursing
- In Fast Track, ICTs are allowed to do these procedures
- Ear lavage
- Subungual hematoma drainage
- Abscess I&D
- Adhesive wound repair
- Staple wound repair
- Suture wound repair
- Digital block
- Splinting
- 5 Sign-offs are required for each procedure by an attending or NP
- ICTs are not allowed to consent, even though they should be taught to understand and can explain the risks and benefits of each procedure
- Please let Sabrina know if you have any questions or concerns
- Keep in mind that when ICTs are able to perform a procedure independently, they are still doing so under the scope of your license and guidance
- They should be writing procedure notes for all procedures they perform with you as the co-signer
LANGUAGE TRANSLATION SERVICES
- We have language translation services available to us. This site gives us the instructions :
- Alternatively:
- Call 1-877-245-0386.
- Provide the Operator with your language request.
- State your client access code: 861846 (no pound needed)
DETOX CONSULTS
- All Core faculty will have DOA (Delegation of Authority) to approve of detox
- Previously, it was a select few of us who bore this responsibility
- You will see “COMMUNITY CARE-MH SUD DETOX” come up on your inbox
- To approve click on the consult
- Click on the toolbar Action Consult Tracking Receive
- Enter in comments “approve for 5 days” for etoh and 7 days for opiates
- Generally if you look at the consult, the SW will also post a time period (5 or 7 days) that they recommend
- Feel free to delete the ones that are not affiliated with the ED (you will see a lot of these come from inpatient or the clinics).
ED NURSING LEADERSHIP
- Have you met our wonderful ED nursing leadership? If not, their office is right across from Jonie’s office.
- ED Nurse Manager – Tuesday Majors (on detail for 90 days)
- ED Assistant Nurse Manager – Angie Baltazar (Acting ED Nurse Manager for 90 days)
- ED Assistant Nurse Manager – Colleen Ferguson
- ED Nurse Educator – Dorian Issac
AIRWAY REMINDERS
COVID AIRWAYS EXPECTATIONS
- If you are doing the COVID airway shift from 11-7, you are expected to do intubations UP UNTIL 7a.
- This means that if there’s an intubation at 6:45, you are responsible for it.
- Technically anesthesia airway coverage does not start until 7a.
- If the 11-7a person does not intubate, this would leave the ED unprotected if both the remaining physicians need to leave
- For the FB attendings, you will be compensated for any extra time you stay
- For the FTEE attendings, you’re given credit for two extra hours after your shift anyway
ED ATTENDING AIRWAYS
- We are still responsible for non-covid airways and crash airways in the ED or after 11p (triple night coverage).
- You get first dibs on any airway you want.
HOW TO CONTACT ANESTHESIA
- Daytime: Vocera "COVID AIRWAY" or the airway pager.
- After 11p: Use the call list on ED SharePoint (see below).
- To find the call list, follow these steps:
- Go to GLA home page
- Go to intranet on right side of page
- Go to Patient care on the top of the page
- Go to big red box "WLA VA on Call Schedule"
- Scroll down to anesthesia
- To find the call list, follow these steps:
AIRWAY GENERAL INFORMATION
- Treat All Intubations as PUIs:
- It is up to your discretion if you want to PAPR vs N95.
- Please wear the recommended level of PPE for aerosolizing procedures.
- Please remember to document your PPE in CPRS note.
- Anesthesia covers all inpatient airways including ED COVID airways from 7a-11p 7 days a week.
- Anesthesia can be called for impending COVID airways if 2 hours notice can be given.
- It is up to your discretion if you want to PAPR vs N95.
ED ATTENDING AIRWAY RESPONSIBILITIES
- Write an Intubation Note in CPRS
- Please hand off the pager to the responsible Airway Attending.
- Airway Team should restock cart and medications after each use.
- Report anything missing to Derrick, Miguel and COVID champions.
ED COVID AIRWAY TEAM
- Overnight:
- Intubating COVID: 11p-7a
- Buddy: A) 12a-8a B) 10p-6a
DAILY AIRWAY CART LOG
- The COVID Airway Shift Attending must check the Airway Carts x2 and new red Airway Box in the med room every day.
- The DAILY “Sign-off Log” and the “Item Checklist” are on separate clipboards on top of the Airway Cart.
- Best practice is to refill the cart after intubation because you know what is missing.
- This daily log is a double check/insurance.
- You also need to check that the COVID medication bags medications are NOT expired.
RESTOCKING CART
- If you need to restock the airway cart, most of the items should be available in the med room (bunny suits, hoods, etc.)
- However, if we are out (because Derrick and Miguel have been primarily stocking these), they would be in the med room or Jonie’s office (requires ED Chief or Nurse Manager key)
- Can ask Charge Nurse for help with missing items
AIRWAY RED BOX IN MED ROOM
- Stored in Med Room
- Check Daily (3 essential items)
- Glidescope Go (CHECK BATTERY)
- Grab and Go Bag (gather items from the Yellow duffel bag)
- COVID Medication Bag
AEROSOLIZING PROCEDURES
- Per Dr Goetz, aerosolizing procedures are okay in PUIs as long as patients are in a negative pressure room (all private rooms in the ED currently) and all staff entering the room is donning appropriate PPE. This means N95, eye protection, face shield, gown, and gloves. This includes:
- CPAP
- Nebulizer treatments
- High flow nasal cannula
- NP swabbing
UNUSED MEDICATION BAGS
- Please make sure all used med bags are discarded.
- Request a new bag from pharmacy.
- It's a violation of policy to leave medications in an undesignated location (this is why the intubation meds are stocked separately in a locked room).
- If you are concerned about waste and intubating in the ED, consider asking the nurse to grab the meds from the omnicell instead.
SECURING ETT VIDEOS
- Zahir and Derrick created a video on how to secure the airway tube
- If you have not done it, it's very difficult to do by yourself- so try it and please review videos.
- BASIC TECHNIQUE TO TEMPORARILY SECURING AN ET TUBE
{{#widget:YouTube|id=dMARECkwt7s}}
- SECURING AN ET TUBE WHILE USING AN AIRWAY BOX
{{#widget:YouTube|id=_CBRZfse9Hs}}
- DEMONSTRATION OF USING A PONCHO WHILE INTUBATING
{{#widget:YouTube|id=JP7V6pb9new}}
AEROSOL BOXES
- Moved to Jonie's office
- This is available for use and is not mandatory
- Added layer of protection (giant splash guard)
- We recommend you practice using it on simulation dummy before deploying for COVID19 airway
SUGGESTED WORKFLOW FOR AEROSOL BOX
- Remember to put what you need inside the box before intubating:
- BVM with HEPA filter, suction, vent tubing, glidescope, tube, tape to secure tube.
- You have the option of draping the other end (extra drapes available on the counter along with tape)
- After securing tube, attach the viral filter/BVM OR continuous capnometry if you have that set up.
- 2nd person (likely RN) will need to bag the patient with viral filter or connect directly to vent.
- Lift the box from the patient and leave it in the room for at least 30 minutes over sink (to allow aerosols to clear) then retrieve for cleaning.
- Sterilize after use with germicidal wipes thoroughly and allow it to dry.
- Buddy can clean this along with glidescope. Should wear full PPE.
AIRWAY MAIN PAGE
WLAVA: COVID-19 ED Airway Main
PPE REMINDERS
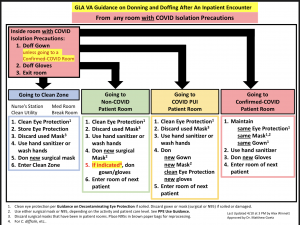
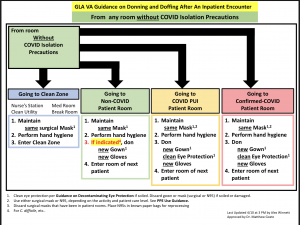
DONNING & DOFFING PPE
- Remember to Don and Doff PPE inside the patient room and only use the closed containers (a red biohazard bin).
- DO NOT place used PPE in the open trash can bins, particularly in the work areas.
- Please pass this on to the residents as well.
FACE SHIELDS
- Face shields are now recommended in addition to eye protection and masks in all patient encounters.
- Face shields are not required when you are not performing face-to-face activities with patients (e.g. while in non-clinical areas, desk, etc.). That is at your discretion if you prefer more PPE.
- Please contact one of the Chiefs to obtain your personal face shield
- Please store in a paper bag (either in your trunk, locker, or cabinet)
GLA UNIVERSAL MASKING POLICY
- Please wear a mask at all times.
- Please remind staff and patients to wear a mask appropriately.
- It is for our own good to prevent spread of employee transmission.
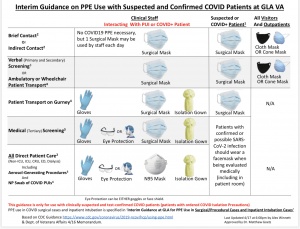
Patient Encounter Scenarios & Recommended PPE
For Patients WITH COVID-19 Isolation Precautions
For Patients WITHOUT COVID-19 Isolation Precautions
UPDATED GUIDANCE ON PPE
- Summary of COS Guidance Document:
- Since in the ED we won’t necessarily know the COVID status of a patient prior to doing a potentially aerosol-generating procedure on a patient (including things like peri-coronal or peri-apical abscess drainage, PTA drainage, nasal packing):
- Our best strategy in the ED is to wear PPE assuming that the patient is COVID+ (face shield, N-95 respirator, gown, gloves)
- Other salient points:
- All patients and staff should always wear a mask
- All patients and staff should maintain 6 feet of distance when possible
- Gloves should be worn in all patient encounters and changed in between encounters
- Hands should be washed (for 20 seconds) or hand sanitizer used after all patient encounters
- Since in the ED we won’t necessarily know the COVID status of a patient prior to doing a potentially aerosol-generating procedure on a patient (including things like peri-coronal or peri-apical abscess drainage, PTA drainage, nasal packing):
USE OF DISINFECTANT WIPES
- We are running low on Saniwipes and other disinfectant wipes
- Please use Saniwipes to clean medical equipment only – reusable PPE, ultrasound machine, etc.
- Do not use disinfectant wipes to clean work areas.
- For all work areas (areas not directly involved in patient care), EMS will be providing bottles of Virex Plus Disinfectant spray or a Glance General Purpose Cleaner along with disposable rags (white) or reusable rags (green) that can be deposited in the dirty linen bins. Please ask the charge where it is being kept.
- File:Disinfecting Procedures.pdf
FIT Testing
- Every Thursday room 3232, from 1p-3p
- Let us know if you still need to be fit tested for the newer masks
PAPR CLEANING
- After intubation or CODE with PAPR use, remind the charge nurse to call SPS to pick it up for cleaning.
- Place PAPR in the dirty utility room, on the cart instead of the floor. It may be assumed to be trash if on the ground.
- If SPS is not called, PAPR may not be cleaned for days and has a high chance of getting lost.
- If there are no more PAPRs left in the Med Room, notify the ED Nurse Managers or COVID Team ASAP.
PPE GENERAL INFORMATION
UPDATE ON MASK GUIDANCE BY COS
- COS published an update to the mask guidance
- All VA employees are not to wear masks with exhalation valves, including disposable and re-usable style masks
- Cloth masks can be worn when not doing direct clinical care
- See CDC recommendations for more information
- Appropriate disposable masks will be provided to clinical staff for patient care activities
PPE MAIN PAGE
- Check out Page below for PPE including PAPR Donning/Doffing Protocols and Videos
WLA VA PPE Main Information Page
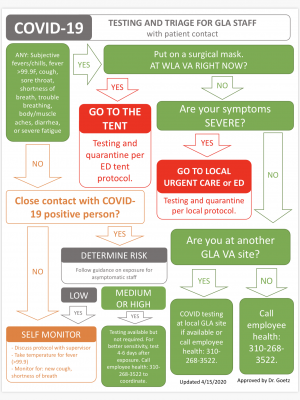
EMPLOYEE HEALTH & TENT REMINDERS
- Avoid having symptomatic patients enter Building 500 if they do not require emergency care.
- Try to accommodate their needs from the tent (i.e., page consult service if they came for appt, call pharmacy to prepare meds if came for refill, skype PCP, etc.)
TENT DISPO TOOL
- Please see the EST Provider Disposition Tool for EST workflow.
- This decision-making tool helps the Tent provider decide on patient disposition and follow up. Please disseminate to tent providers.
EMPLOYEE SELF-REFERRAL TOOL
- Please refer asymptomatic employees working NORTH of Wilshire to Employee Health.
- Please refer asymptomatic employees working SOUTH of Wilshire the tent.
- The Best time to test is 4-6 days after exposure so they can usually wait for an employee health appointment.
- Employee self-referral tool helps employees decide how to best manage their symptoms, when they can return to work, and when to get tested for COVID-19.
- We can use this tool, but mainly to assist other employees.
- Please use and distribute this so that people can present to the correct location (Employee Health, Tent, or ED) and so they know how to correctly self-triage their symptoms/exposures.
- GLA VA Employee Symptom Self-Referral Tool
SEROLOGICAL TESTING
- Getting the test:
- Free serological testing will be available to all employees on a voluntary basis
- Blood draw occurs through the outpatient lab
- Submit LEAF request (VA Intranet) PRIOR to blood draw
- Expect 1-2 day delay in processing prior to being able to show up at outpatient lab
- Serological testing results:
- Serology results are now available online.
- Click this link and you will be taken to this screen:
- Enter your DOB and click "apply"
- You will need both patient-level CPRS and your Network Username in VistA. Easiest way to do this would be at the VA.
- Contact Employee Health (310) 268-3522 if you do not see your results
- If you don't see the title "Covid-19 Employee Self-Lookup" after clicking the "Apply" button, please email VHAGLADataAnalysisHelp@va.gov with a screenshot of any other error message.
Employee COVID-19 PCR Triage Algorithm
Last Updated: 4/16/20
Employee Exposure Risk Determination Algorithm
Last Updated: 4/17/20
- Reviewing the exposure risk algorithm shows that this simple intervention keeps exposure risk low to medium.
- Second layer of defense is ensuring that you wear a face mask (NOT N95).
EMPLOYEE RETURN TO WORK GUIDANCE
Last Updated: 7/23/20
- Return to work for persons with mild to moderate illness who are not severely immunocompromised:
- At least 24 hours have passed since resolution of fever, if any (without the use of antipyretics) and
- There has been improvement in respiratory symptoms (e.g., cough, shortness of breath) and
- 10 days have passed since the onset of symptoms or time of diagnosis (whichever period is longer)
- All criteria must be satisfied prior to return to work.
- Return to work for persons with severe to critical illness (required O2 or admission) or who are severely immunocompromised:
- At least 24 hours have passed since resolution of fever, if any (without the use of antipyretics) and
- There has been improvement in respiratory symptoms (e.g., cough, shortness of breath) and
- 20 days have passed since the onset of symptoms or time of diagnosis (whichever period is longer)
- All criteria must be satisfied prior to return to work.
- Notes:
- After returning to work, persons with direct patient care responsibilities should always wear a facemask for source control while in the healthcare facility until all symptoms are completely resolved or at baseline. A facemask instead of a cloth face covering should be used by these HCP for source control during this time period while in the facility.
- Reference file:
TENT GENERAL INFORMATION
- EST open M-F 7:30a-4p excludes holidays and weekends.
UPDATED PRE-PROCEDURAL COVID TESTING FLOW
- See attached filed for updated preprocedural testing flow
- Update includes:
- No testing if positive COVID within 90 days
- Time course of when procedure is allowed to proceed
- Remember that in order to be seen in the pre-procedure testing, patients need to have an order and appointment 1-3 days prior to procedure. If they show up in the ED, it is probably because one of these two were not completed.
- File:PreProcedural OUTPATIENT COVID Testing process workflow_080720_final.pptx
PRE-PROCEDURE TENT
- The pre-procedure tent will be getting more volume as the hospital expands operations.
- If you haven't noticed, there are two sides to the tent - symptomatic tent and the pre-procedural tent for those needing surveillance screening prior to their operations, infusion, dialysis, etc.
- For patients to show up in the pre-procedure tent, they must have an appointment and order by the original provider.
- Some of these asymptomatic patients are being sent to the tent without orders or an appointment and then need to be seen in the symptomatic side because they need an order from the tent provider.
- If they end up being seen by the tent provider, please perform the test. Then try to locate the service/individual who sent them to provide directed feedback that they should be placing the order and having the patient make an appointment.
- If you are unable to locate the sending provider, email
vhawlaest@va.gov (or for any other tent issues) with the information so that the tent leadership can follow up.
- Our goal is to keep the pre-procedure patients (who are higher risk usually) separate from the symptomatic ones in the screening tent.
TENT MAIN PAGES
COVID WORKFLOW REMINDERS
WLA VA ID COVID-19 TESTING ALGORITHM
- Last Updated 6/26/20
- Reference file (for printing):
File:6.c.i.5_20200624_GLAVA_Algorithm_Triage_OutpatientBldg500.1.pdf
RE-TESTING PREVIOUSLY POSITIVE DOM PATIENTS
- DOM patients that were previously COVID positive do not need to be re-tested for surveillance until 90 days after the positive test.
- Patients may discontinue isolation and return to the DOM if mild/moderate disease in 10 days (20 days if severe disease)
- File:GLA ID COVID Discontinuation of Isolation Guidelines.pdf
NASAL SWABS
- As a reminder, Nasopharyngeal swabs are only for admitted patients. Please make sure you order the correct one and that the nurse knows to perform the correct one.
- Nasal swabs are for all other patients
- This is not considered an aerosol-generating procedure
- This decreases risk to swabbers
- There is no need to terminal clean
- Having more snot increases the accuracy
- NP swabs are more difficult to acquire and nasal swabs require the lab to prep some special media so it’s easier and cheaper to replenish
UNIVERSAL MASKING
- Please wear masks at all times while in the ED.
- No eating is allowed at MD workstations due to increased risk of transmission.
- Previously it was said that snacking was okay but due to constantly having to remove your masks for snacking, please avoid all food.
- Drinks are okay.
- Stagger breaks so that you can eat outside or in a private area.
- No more than 2 people should be in ED breakroom at a time.
- No potlucks, parties, or shared foods/drinks.
- Please reinforce this with the residents.
COVID-19 TRIAGE SCREEN
- Please make sure to review the COVID-19 Screen section of the ED RN Triage Note.
- ED Nurses are supposed to notify the Charge Nurse of any patient that screens positive (these patients should be placed in a private room with isolation orders).
- This information is supposed to be relayed to ED provider, but it may not be happening routinely (please let Manny know if it isn’t).
- If after you see the patient, you feel that their COVID-19 screen is actually negative (i.e., patient cough is chronic without acute change) please document that in your note.
4th MISSION (NONVETS) ONLY
- The VA will be absorbing some of the load from the community. This is for NON-VETS only. We are still trying to figure out the details and it is a work in progress. We will be accepting up to 6 med/surg and 7 ICU patients. All calls should come from Cal EMSA or the AATC
- Workflow:
- Step 1 - Confirm that it's not an ED directly calling you and it's coming from the AATC
- If an ED contacts you directly, have them call AATC 1855-301-2337 or our Transfer Office (M-F 7a-5p 31448)/OTS (after hours) x53568 or p99510
- Step 2 - Call the Transfer Center or OTS to confirm that we have a 4th mission bed available to for level of care needed
- If no bed available, reject the transfer
- Step 3 - Take report, ask for the expected level of service and review report to ensure that level requested makes sense
- Step 4 - Call admitting service to inform them of transfer
- If GMED, call MOD
- If PCU/ICU, call ICU team
- Step 5 - Accept the patient. When the patient arrives, stabilize and reassess, admit to appropriate level of care.
- Text Manny with any potential cases (619) 316-0640
- Step 1 - Confirm that it's not an ED directly calling you and it's coming from the AATC
- For regular vet transfers, proceed as usual. Refer to the transfer center (or OTS) first to ensure that the patient is a vet and that we have the bed availability. Once we have confirmed this, you are free to take the clinicals from the physician.
- Remember to write a transfer request note so that the oncoming physicians know why the patient is here.
ISOLATION FOR PUIs
- For high-risk PUIs, isolate the patients even if COVID is negative. Let the admission team decide if isolation should be removed.
TESTING ASYMPTOMATIC PATIENTS
- If a patient insists on being swabbed while being asymptomatic, please try your best to educate the patient about why it is not necessary.
- If the patient is still insistent and says they’ll get swabbed elsewhere (e.g. county), please just go ahead and swab them. We do not want our patients to be swabbed outside or system.
- Send the LB (Roche) tests on these people and NOT the CEPHEID
FAST TRACK PUIS
- Tent is CLOSED weekends, holidays, evening, nights (WHEN hours) so we will be seeing all the tent patients in FT.
- Usually Tent hours are M-F 7:30a-4p, but the last patient the tent will see is a 3:45 and we will be given a handoff for patients thereafter.
- Obtain a nasal swab (instead of NP swab) for all low acuity PUIs that are unlikely to be admitted. All other ED PUIs, get a CEPHIED.
- NP swabs require terminal clean of the room (technically AGP).
PATIENT CANT TOLERATE NP SWABS
- If the patient is unable to tolerate a nasopharyngeal swab (coughing, gagging, restlessness), it is fine to do a nasal or oropharyngeal swab. ** Make sure to edit the order to specify mode of collection.
NASAL SWABS
- Anterior nasal swab are used for all except pre-admission testing
- For admissions, obtain NP swab (if already obtained nasal swab do not need to re-test with NP swab)
COVID TESTING FOR TRANSFERS
- GLA's unwritten policy is that COVID testing is not a prerequisite for transfer of a patient to WLA from another facility
- If the patient is stable for transfer, then the transfer should occur
- COVID testing can be done in the ED and the patient's destination determined as a results
- Please let Manny know when this happens as he is keeping track of the volume of these patients
HOW TO ORDER CEPHEID (RAPID) TEST
- CEPHEID order in ED Order Menu Screen
CEPHEID REPEAT TESTING
- If a patient had a CEPHEID done for an anticipated admission, left AMA or eloped briefly and returned to the ED for admission, the COVID-19 test does not need to be repeated.
- COVID test is assumed good for 5 days provided that the patient is not newly symptomatic.
- We have not clarified other bouncebacks yet with the other services.
PATIENTS REFUSING COVID19 TEST
- If a psych patient is refusing a swab, DO NOT try to force them to get it done.
- This could endanger the staff.
- Medical Director (Dr. Braverman) believes that compelled testing is necessary in patients who are refusing swabs.
- After doing everything you can (de-escalation, etc) with patient, please notify one of us for further action.
- May need to admit to medicine, w/ isolation precautions, until a swab can be obtained.
NEGATIVE PRESSURE ROOMS
- Move patient to negative pressure room if plan to perform aerosolizing procedure.
CLARIFICATION ON NIPPV
- There is no absolute contraindication for NIPPV in COVID unknown patients. We do not have an institutional policy against it.
- However, we must continue to be very judicious with its use.
- It is generally not recommended in COVID PUIs and decision should be made with consideration for HCW exposure (risk higher with BIPAP vs HFNC).
- If suspicion for COVID is low and patient may benefit from NIPPV, have a discussion with care team (RN and RT) to weigh risks/benefits.
- Obtain CEPHEID early on these patients.
ED-TO-ED TRANSFERS
- Please CEPHEID retest ED-to-ED transfers for admissions EVEN if they have had a negative COVID testing <24 hours ago.
- The reasoning is that there are concerns that the sensitivity of the RT-PCR is 75-90% and due to past discrepant results from the long term care facilities.
DIRECT ADMISSIONS
- Direct admissions will not require COVID results.
- They can be admitted as a PUI and have it done on the ward.
- Therefore, you should not be receiving patients in the ED just to get COVID testing before going upstairs if direct admit.
PULSE OXIMETERS
- Veterans can now get home-use personal oximeters in high risk patients with confirmed or suspected COVID-19 that you are planning on sending home.
- Pulse ox devices are in the same locked cabinet as the ED iPads, key is in the red lockbox code 119.
- See Manny’s email from the same day for more information
- For more information or handouts see slack channel or ED SharePoint (Va intranet)
DEXAMETHASONE
- We are already using Dexamethasone in treatment guidelines on the inpatient side and in the ICU.
- Decision to start dex should be left to the admitting team.
- Be on the lookout for upcoming education update about this.
ED BREAKROOM
- No eating at MD workstations.
- No more than 2 people in ED breakroom.
- Eat outside or in private area.
- No potlucks, parties, shared food/drinks.
COVID WORKFLOW GENERAL INFORMATION
COVID-19 Quick Guide 4/24/20
- Last Updated: 4/24/20
POSSIBLE COVID-19 AFTERCARE
- For patients discharged with possible COVID:
- Please clearly inform them that regardless of the decision to test for COVID, they could still have the disease. Therefore, they will need home isolation instructions.
- Printouts of the LA County handout: "Home Care Instructions for People with Respiratory Instructions" are available in the wire rack next to the residents.
- A copy is uploaded on the Sharepoint under "ED Common Resources"
- Please distribute this and document you did so in the chart.
- Use the ED PACT tool for f/u for these patients
HOME ISOLATION/QUARANTINE RECOMMENDATIONS
- LA DPH home isolation handouts available in the wire rack.
- Please send all PUIs home with handout.
- Current advisement is to stay at home until at least 10 days after your symptoms first appeared AND 3 days after your symptoms have recovered.
- Recovery defined by:
- Resolution of fever for 72 hours without using antipyretics AND significant improvement in respiratory symptoms.
- This applies even if you had URI sx, were retested and had a negative COVID-19.
HOW TO PLACE ISOLATION PRECAUTIONS
- Please have a low threshold to place patients on isolation for COVID-19.
- Start a new note:
- Type in 'Isolation Note:'
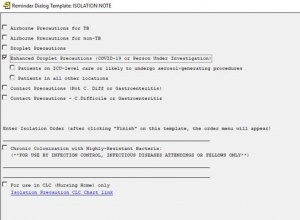
- Select Enhanced Droplet Precautions for COVID-19 patients:
- Once you finish the isolation note template, go to 'Orders' menu and sign the isolation order:
[[File:Iso order.jpg|thumb|center|Isolation Order]
DISCONTINUING ISOLATION PRECAUTIONS FOR PERSONS WITH COVID-19
- The test based strategy is no longer recommended to discontinue isolation, with rare exceptions (severely immune compromised). Previously, two negatives were suggested.
- The symptom based strategy is:
- At least 10 days have passed since symptoms first appeared
- Free from fever for 24 hours (changed from 72)
- Improvement of symptoms (changed from improvement of respiratory symptoms)
- For patients with severe or critical illness, duration is extended to 20 days from onset
- If patient did not have any symptoms, discontinuation will be 10 days after the date of collection of initial positive PCR
- The symptom based strategy is:
- Reasoning - persistent positive PCR test within the first 3 months is likely persistent viral RNA shedding instead or re-infection.
- Repeat testing is not recommended for 3 months after initial illness who remain asymptomatic.
- Repeat testing may be warranted if there is no alternative diagnosis patient develops new symptoms after close contact within 14 days.
- GLA will be adopting these policies but it shouldn’t change our practice in the ED much.
- You should still continue to order CEPHEIDs on all admits, obs, and psych patients for surveillance.
- This will affect how you counsel your patients about discontinuing isolation.
- Remember, these are LA DPH and CDC recommendations. There are still some employers, airlines, etc that will require a negative test. If the patient gives a reasonable request, go ahead and do the test.
COVID DEVICE CLEANING
- If you cannot find Sani Cloth AF3 (grey top), here are alternate ways to clean devices
- Glidescope:
- Super Sani-cloth (Purple top)
- Contact time: 2 minutes
- Ultrasound (new): Sonosite EDGE II:
- Monitor: Alcohol
- Transducer: Bleach wipes (leaves residue)
- Ultrasound (old): Turbo:
- Monitor: Alcohol
- Transducer: Super Sani-cloth (purple top)
- Reference document on approved disinfectants:
- Glidescope:
CODING COVID-19 ENCOUNTERS
- For Suspected or Exposure to COVID19 or Exposure: Z20.828
- For Confirmed COVID19: B97.29
- Other suggested ICD10 codes include (but not limited to):
- Acute Upper Respiratory Infection, J06.9
- Cough, R05
- Viral Infection unspecified, B34.9
- Fever unspecified, R50.9
SNF OUTBREAK
- Low threshold to place SNF patients on enhanced isolation (please wear appropriate PPE!).
- Asymptomatic patients, not able to isolate in SNF, will be directly admitted to inpatient. Symptomatic patients will go through the ED.
- Expect that these patients will come to the ED and have a low threshold to admit.
PSYCH ED PATIENTS
- Order a CEPHEID for any patient that is placed in the psych ED regardless of whether or not you believe they are going to be discharged
- There was a incident where a patient was asymptomatic and exposed multiple patients in the psych ED and therefore we are allowing CEPHEID for these patients specifically
OPENING OUTPATIENT SERVICES
- Hospital is delaying opening outpatient services to 5/26 (was previously 5/18).
INPATIENT VISITATION POLICY CHANGE
- Check your email for the policy document, highlights include:
- Inpatient visitation under a public health emergency with social-distancing guidance
- Visitation is prohibited with the exception of Veterans who are at the end-of-life, defined as having a prognosis of hours to short-term days.
- Compassionate visitation exceptions will be considered on a case-by-case basis only with recommendation from the Attending Physician or Nurse Manager, and concurrence of the Chief of Staff.
- The Attending Physician, in consultation with the Nurse Manager/Charge Nurse, will make the final decision as to whether a veteran patient may have visitors if there is conflict or concerns between staff.
- Inpatient visitation under a public health emergency with social-distancing guidance
PATIENT VISITATION POLICY (FROM COS)
- Children under the age of 18 years are not allowed to enter the facility.
- If you require an exception, contact the Chief of Staff or Associate Director for Patient Care Services.
- For Veterans who arrive at our facility for emergency care with children under the age of 18.
- The veteran should be admitted to the ER.
- GLA staff should make all reasonable efforts to assist the veteran in identifying a responsible adult who can care for the child during the emergency visit.
- Should efforts fail, VAPD should be notified to take the child into protective custody.
- VAPD should contact the LA County Child Protection Hotline (800) 540-4000.
VVC OUTREACH CONSULTS
- VVC will be used in the future for Telehealth. It would be useful to have all patients familiar with this but may be difficult given our generally elderly population who may have difficulties with technology.
- The VVC Outreach consults will have Telehealth Staff contact the patient to provide a VVC test call and education for the future.
- For those elderly patients who may have difficulties doing this on their own, please place a VVC Outreach consult if they have a future VVC appointment.
EDUCATION/SIMULATION REMINDERS
RECOVERY TRIAL (1,2,3)
- Randomized, controlled, open-label, adaptive, platform trial performed at 176 hospitals in the United Kingdom
- Pre-publication/not peer reviewed
- Usual care (4321 patients) Vs. Dexamethasone 6mg PO or IV qday for up to 10d (2104 patients)
- 28d morality overall: Usual care 24.6% Vs. Dex 21.6%
- 28d morality intubated patients: Usual care 40.7% Vs. Dex 29%
- 28d morality in pts on 02 (including NIPPV): Usual care 25% Vs. Dex 21.5%
- 28d morality in pts not needing 02: Usual care 13.2% Vs. Dex 17%
- Conclusion:
- Dex dramatically reduced 28d mortality in intubated patients. NNT 8.5
- Dex reduced 28d mortality in patients requiring supplemental 02/NIPPV. NNT 29
- Dex had a non-significant trend to harm in patients not requiring 02
- Applicability at GLA:
- At GLA the decision on dexamethasone is left up to the admitting team.
- There is no indication that early dex is better.
- In fact, patients with >7d of symptoms did better than those with <7d of symptoms.
- Theoretically it is effective in the inflammatory phase of illness, but possibly harmful in the viral phase
- In fact, patients with >7d of symptoms did better than those with <7d of symptoms.
- Looking forward: This trial actually had a ton of arms that compared 6 treatments in various combinations.
- Drugs studied included: dexamethasone, hydroxychloroquine, lopinavir-ritonavir, azithromycin, convalescent plasma, tocilizumab
- We have not heard the last from this data set
- For those of you interested in what’s hot and what’s not for inpatient covid19 treatment check out the attachment adapted from Adventist Health.
- References:
- 1. Horby PW et al. Effect of Dexamethasone in Hospitalized Patients With COVID-19 – Preliminary Report. medRxiv Preprint 2020. [Epub Ahead of Print]
- Rebel EM RECOVERY TRIAL Review Post
- EMCrit RECOVERY TRIAL Review Post
MOCK CODE DRILLS REMINDER
- Try to perform mock codes if clinical duties permit. DHS is expecting a second spike soon and nursing needs to be trained up in PPE and for these codes.
- In particular, make sure that the RNs are familiar with the donning/doffing procedure and practice it
- COMMUNICATION is the most challenging part of these scenarios:
- "Quiet voices" within INSIDE team while RN1 is the main communicator with charge RN (just need to practice this)
- Baby monitor or Vocera seem to be best
- Practice doing each role: MD1, MD2, Leading drill/observer; have the nurses also practice roles they haven't tried yet as well
- Be very familiar with Airway COVID cart/and box.
PROCTORING DOCTORS-IN-TRAINING
- Medical students returning, not allowed to see PUIs.
- Interns get oriented every Thursday at 10am of their new rotation.
- Please make sure that the interns are informed of COVID, where to get appropriate PPE, and how to don and doff.
- 8000 Masks are available from charge nurse
- 3D printed face shields are in the upper cabinets
- Hospital face shields are in the med room
- Goggles will be with nursing, although it is unclear if we have enough for everyone and this will be a shared resource between physicians and nurses.
- If the intern is not fit tested for the 8000 series, please tell them to coordinate with their chief resident.
- If the intern is not fitted for 8000 series, please advise him/her against seeing PUIs until tested.
- They would have to use the 1860/1870 masks and we have a limited number of those remaining and reserving those for staff that failed out of the 8000 masks.
CODE GENERAL INFO
- NRB hanging in front of beds 6& 7 (please replenish if used)
- LUCAS now available-->RN1 and RN2 in room while ICT/NA fully DONNED outside
- RN2 to PAPR if preferred (will be more available to assist MD with intubation/give meds)
- Will add EPI laminated sign to COVID cart
- If patient coming through EMS-MD fully donned meet them at the entrance to assess situation (if time allows)
- Reference Documents:
SIM LAB TRAINING
- Email Cindy Koh, Carol Lee or Sabrina Tom if you have not been signed off on airway PPE donning and doffing simulation.
FIT TESTING
- To clarify, you need to be FIT tested yearly at each facility you work because the brand and type of mask may be different. Your face may change shape with age/weight/pregnancy etc...
UPCOMING FIT TESTING DATES
- EVERY Thursday Room 3232 12-2
- FIT Testing Sessions:
- Please complete online form prior to testing:
- URL: http://respiratormedicalevaluation.com
- Organization Code: vala
- Please complete online form prior to testing:
GENERAL WORKFLOW REMINDERS
ICT FORMS
- The ICTs are required to maintain a record of 5 sign-offs for each procedure for which they received formal training.
- Some of the earlier trained ICTs have lost track of the procedure sign off forms. These are intended to be kept by the ICTs.
- If you happen to have one, please let Sabrina know or give them to one of the nurse managers.
RESIDENT NOTES
- Please make sure residents are writing the correct ED Note. (should be the one replacing 10-10). Some are writing the incorrect note.
PLATELET FUNCTION TESTING
- Effective August 4th, we are able to provide platelet function testing for patients taking aspirin and P2Y12 Inhibitors such as Plavix.
- To order this, you need to contact the blood bank at x53535 to request the testing form, which must be filled out and returned to the blood bank with the patient sample
- The specimen needs to be hand walked down, pneumatic tube will interfere with results
- This is not orderable by CPRS
- Test results will be available within 4 hours of collection
- File:Memo Platelet Function With VerifyNow.pdf
PHARMACY FRAUD ALERT
- Fake prescriptions are being faxed to providers for authorization that appear to come from legitimate pharmacies.
- The provider is asked to authorize the prescription by signing and returning
- These are seemingly benign prescriptions such as topical relief creams (lidocaine, diclofenac), diabetic upplies, or durable medical equipment.
- Red flags are prescriptions received by paper fax or from an out of state pharmacy.
- If you receive any of these, verify any outside communication as being consistent with the Veteran's medical history and don't sign any requests without prior verification.
- You can report any suspicious prescriptions by calling the CBI Helpline at (866) 842-4357, or email vhacbihelpline@va.gov.
- Please see attached advisory
ED IPAD PROGRAM
- Kat Yip is spearheading our iPad deployment program (SOP pending).
- Aims of the program:
- Allow Veterans to stay connected to family using video technology.
- To decrease unnecessary face-to-face time (F2F) while evaluating a patient with symptoms of COVID.
- Apple ID p/w (case sensitive): Covid2019**
- iPads are turned off by default (don't assume it is not charged) to preserve battery.
- Please clean, turn off after use (preserve battery), and return to locked cabinet.
- Key to locked cabinet is in red lock box (code 119) inside the ED Provider Workstation area.
- Email Manny and Kat for feedback/issues.
OBSTETRICS PATIENTS
- Given our increasingly diverse population, be prepared to see obstetric patients in the ED
- See the attached document regarding Pregnant patients and COVID-19
- Salient points are:
- Pregnant patients with mild or no symptoms can be tested and treated at the VA
- Pregnant patients with severe symptoms should be transferred out after initial stabilization
- There is very little data out there about having COVID-19 while pregnant or breastfeeding
- Advise pregnant patients to continue to practice usual precautions such as social distancing, handwashing, and avoidance of face touching as with other patients
GC/CT SAMPLES
- We can collect OP and anal samples for GC/CT.
- Collection document: File:Chlamydia Trachomatis and Neisseria Gonorrhea Collection.pdf
REVISED CARDIOLOGY ADMISSION CRITERIA
- Please note that the Cardiology team cannot care for ICU level patients. Patients requiring ICU level of care will be admitted by the MICU team with mandatory cardiology consult. This includes, but not limited to:
- Hemodynamically Unstable Arrhythmias:
- Atrial fibrillation / flutter requiring titratable gtts for rate control
- Ventricular tachycardia/VF electrical storm/multiple ICD shocks
- High degree/complete heart block (with or without temporary pacing wire)
- Cardiogenic shock, with or without mechanical support (ie. Impella), or heart failure requiring frequent titration of vasoactive gtts
- Acute Coronary Syndrome
- Unstable angina/NSTEMI that is hemodynamically unstable, requiring NTG gtt or other vasoactive gtts
- STEMI
- Hemodynamically Unstable Arrhythmias:
VANCO DOSING FOR MRSA
- In collaboration with our ID colleagues, pharmacy, and based off of 2020 ID Guidelines, Vancomycin dosing should be loaded on a weight-based dosing rather than the standard 1gram dosing in these patients:
- Those that require ICU-level care because of the severity of their infection.
- Acute septic arthritis.
- Possible/probable endocarditis.
- Other strong evidence of bacteremia.
- This DOES NOT apply to routine cellulitis/abscess/SSTI that you are giving a one time dose to or “failed oral abx therapy”.
- We will work on changing CPRS to “dose per pharmacy to load” or “dose per protocol” but in the meantime use these guidelines.
- Current 2020 guidelines state 20-35mg/kg loading dose in critically ill patients with suspected or documented serious MRSA infections. Due to our generally elderly population, err on loading 20mg/kg.
- The maximum dose should not exceed 3 grams.
- If you have any questions, please consult our ED pharmacist.
ED PHARMACIST
- We now have in house ED pharmacists: My "Phoung" Pham - program manager, Srjit "Surj" Singh, and William Duong
- They will be sitting next to Dexter (UR) for now
- They are available from 7a-7:30p (with 30 minute lunch)
- Please ask for any pharmacy/medication related issues
- They are also able to dispense naloxone from the ED and will help with patient education
- If questions or problems, ask Cindy Koh
MEDICAL RECORDS
- Try not to use the medical record to litigate administrative issues. Please try to make your documentation an objective record of the care you provided (including timestamps if appropriate), the consultants you spoke with, and their verbal recommendation (including name and timestamps if appropriate).
- If you encounter an administrative or interpersonal issue (i.e., the consultant did not page you back or was rude) try to keep that off the medical record. If you have issues with a consultant paging you back, please make sure to escalate up the chain of command in realtime. We should address any patient care delays in realtime, since documenting delays in care without going up the chain of command does not necessarily release anyone from liability. The escalation should be as follows:
- Resident on-call
- Attending on-call
- Service Chief
- ED Chief and MOD
- CoS
- If you come across any interpersonal issues or people making up fake policies, please email Manny a summary of the encounter and he will f/u with the corresponding service (use encryption if sending PHI).
NALOXONE NOTE
- When signing the Naloxone note, make sure you sign your ED Note FIRST.
- When you sign the Naloxone note first, it uses "Opioid Use Disorder" as a primary diagnosis and causes the encounter to fall out
- By signing the ED note first, you can fill out the encounter form appropriately and give the proper diagnosis.
PROSTHETICS CONSULTS FOR ITEMS DISPENSED IN THE ED
- If an item is dispensed from the ED, you still have to place a prosthetics consult
- Just note that it was dispensed from the ED
- This helps us keep track of items that patients are requesting, particularly canes
- Theoretically patients are being billed for it
RAPID ACCESS/DIRECT
- Please remember to have ED clerk obtain an appointment PRIOR to DC for any ED patient being sent to Endocrine for DM management for urgent/Rapid Access Follow-up.
- Please confirm that this actually happens before the patient leaves the ED. Our clerks must schedule an appointment prior to ED discharge for all Rapid Access/Direct Scheduling consults.
Mask Policy
- To mitigate exposure risk, please make sure that all ED patients (and staff) are complying with our universal masking policy. When evaluating any patient, at minimum wear eye protection and a face mask.
- Please see attached document that outlines indications and processes for prevention of COVID transmission in the outpatient setting.
SEE ALL PATIENTS PRESENTING TO ED
- Do Not Send Patients to the Tent from ED (EMTALA Violation).
- If patients present to the ED but should have been screened out to the tent or seen in the tent, please do not send patients back to tent from the ED.
- Our goal is to make sure to keep potential “walking well” COVID patients outside the hospital.
- However, once a patient has walked into the ED for one reason or another, please just see them. We do not want these patients moving around the hospital.
- This goes for all patients – once they have presented to the ED, we “own” them and should complete the encounter.
- This helps us as well in terms of increasing capture for the work we are doing.
CHAPERONE POLICY REMINDER
- Chaperones must be present for sensitive exams
- Chaperones must be the same gender as the patient identifies
- Chaperones cannot be residents, who are considered an 'extension' of the attending
- Document the name of the chaperone in the chart
- Males must be offered a chaperone. If they decline, document this in the chart
SHIFT SWAPS
- Scott Jacobs is managing all scheduling edits through July.
- Please email him directly with any proposed swaps.
UM Review
- Use ‘UM Review’ label on EDIS to communicate with UM.
- Here are ways to contact UM if you have questions:
- VA cell: 626 314 9774
- VA Pager *11 p73284
- Here are ways to contact UM if you have questions:
ADMINISTRATIVE/MISCELLANEOUS REMINDERS
ED REMODEL UPDATES
- ED pharmacist has been moved to the area next to the residents – Jonie as labeled this as “ED Pharmacist”.
- We have added one more computer there and rearranged some things.
- Attending cart is now next to the future gyn room across from the ED break room.
- Please do not put any carts or ultrasounds in the hallway in front of the MD station. That area is supposed to remain clear for traffic. The only thing that should be parked there is the smaller ultrasound machine, which has its own nook.
- Room H is not authorized for use yet. This will be our future gyn room.
ED PHONE EXTENSIONS & VOCERA
- Thanks to Jonie for creating this page (linked on sharepoint ED homepage). In case you haven’t noticed, it has been there for months.
- This has some tips on how to use Vocera, user names, and commands:
ED SCHEDULE
- Bytebloc schedule is not accurate for July, please check Onedrive Excel schedule link sent to your personal email
- We are returning to Bytebloc permanently starting October (please submit October requests by 8/2)
- Until we return to Bytebloc in October, please contact Scott Jacobs for August/Sept shift changes
- Once we use Bytebloc, all changes will be managed by the online program
TMS TRAINING (CORE FACULTY ONLY)
- Please complete TMS Peer Review Training VA #40695. All core faculty are being assigned this TMS and needs to be completed ASAP.
LACTATION ROOM
- Fast Track Physician Workroom (when not in use)
- The “Family Room” in the hospital chapel is our hospital designated Lactation Room
- Room 6628A (inside the side door of the Chapel)
- CODE: 3451
- Call Room on 6th floor EAST
- CODE: 2189
FACULTY CME REIMBURSEMENT
- Jonie has put the procedure here (sharepoint only)
- Submit your educational stipend requests asap. Deadline is Sept 30, 2020
- You will need to place the LEAF request early prior to any start date
- Aim for August 15, 2020
- You can purchase the product and send receipt with form ; make sure the start date is after purchase
- No travel will be approved due to COVID-19
- If you have any other questions, please call Patricia Moonyeen Gamboa/Patricia Cruz x43512
AT RISK RESIDENTS
- At-risk resident will be working on a WOW outside a room to socially isolate.
JONIE/BABY CHIEF OFFICE
- As a reminder, please do not eat in Jonie’s office or use it for clinical work. There was an open mug of coffee with spoiled milk on Jonie’s desk that spilled. It was gross and a pain to clean, and nearly destroyed a bunch of valuable PPE and the viral filters.
- If you need to finish charting, please use the 3rd-floor office
REMOTE ACCESS AND CHECKING VA EMAIL
- Detailed instructions on Slack (email Manuel for access).
- Please check your VA email while you are on shift.
- If you need remote access, apply through this link
- Click on “request access” and choose the “Rescute/CAG/GFE Mobile” option.
- You will need the CAG access (using personal computers to remotely log in).
PIV EXEMPTIONS
- There may be some problems with the mass PIV exemption. If you run into issues, you can try one of these avenues
call *14 - Enterprise Service Desk
- Dwight.Brown2@va.gov
- Shawn.Arnold@va.gov
- Incident/Ticket number is IVC1043797
UCLA BADGE & MEDNET EMAIL ACCOUNT
- For Full-time faculty: How to apply for UCLA badge and mednet email address
- Slack: gla-va-em.slack.com
- Under the left sidebar, you will see ucla-va-faculty-appointment-faq
- Slack: gla-va-em.slack.com
MS OFFICE & FREE APPS
- We get discounted Microsoft Office from the VA. Follow the link and an email will be sent to your work VA email.
- For full time faculty with a mednet email, we can get free zoom, box, Qualtrics, and office 2016.
ED FELLOWS
- We will be having rotating UCLA Fellows rotating through the ED as attendings a few shifts a month
- Max Berger - UCLA MedED Fellow
- Abdulkareem "Kareem" Agunbiade - UCLA Ultrasound Fellow
- They will be allowed to staff patients with residents
VA Scrubs
- Please see COVID-19 Update #15 email 'Scrubs' MS Word document for details on how to access ScrubEX.
- It took some effort but we finally secured enough scrubs to cover all ED/FT provider shifts each day.
- However, we have to make sure to return them at the end of each shift. If you do not return it then that means the provider coming in after you will not have scrubs.
GLA Showers
- No Lockers - Bring your own towel/clothes
- Ground Floor (Basement):
- Women’s Locker Room: Rm 0435 passcode 2169
- Men’s Locker Room: Rm 0403 passcode 2168
- 5th Floor (OR Showers):
- Women’s Locker Room: Rm 5076 passcode 5324
- Men’s Locker Room: Rm 5075 passcode 5321
Alternative Housing for Staff
- The Fisher house is available for those who are interested and need housing options away from family.
- Please contact Neil if interested and include exact dates and details.
- Preference to Distance > DEMPS > Risk at home > # Consecutive shifts.
Donations (PPE/Food Etc.)
- Please contact Alexia Lunningham, Chief of Voluntary Services at (310) 268-4350 or alexia.lunningham@va.gov to coordinate.
File:VA COVID-19 Donation Form 4-2020.pdf
GLA WEBSITES
- Links to GLA COVID19 documents and resources (https://dvagov.sharepoint.com/sites/VHAGLAMed/ed/default.aspx)
COVID-19 VA Cases Nationally
https://www.accesstocare.va.gov/Healthcare/COVID19NationalSummary
Emergency Alerting & Accountability System (EAAS)
- If you wish to receive alerts from the VA EAAS (https://alerts7.athoc.com/SelfService/VAEAAS)
- Any issue please contact Lonnie Miller at x40863
Other WLA VA Pages
- WLAVA: COVID19 ED Airway Main
- WLAVA: COVID19 PPE Main Information Page
- WLAVA: Enhanced Screening Tent
- WLAVA: EST Provider Orientation
- WLAVA: Enhanced Screening Tent Telehealth
- WLAVA: COVID19 Administrative
WLA VA COVID19 Page Listing