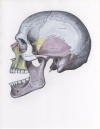
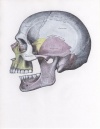
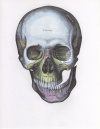
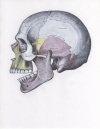
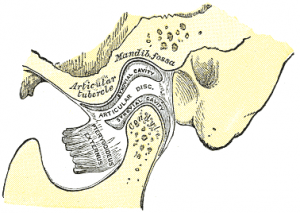
Mandible dislocation
(Redirected from Mandibular dislocation)
Background
| Dislocation Type | Frequency | Associated with trauma? | Mechanism | Additional Comments | Associated with fracture? | Image |
|---|---|---|---|---|---|---|
| Anterior |
|
|
|
|
|
|
| Posterior |
|
|
|
|
|
|
| Lateral |
|
|
|
|
|
|
| Superior |
|
|
|
|
|
Clinical Features
- Inability to close mouth
- Difficulty speaking or swallowing
- Malocclusion
- Pain localized anterior to the tragus
- Prominent-appearing lower jaw
- Preauricular depression
- Condylar head palpable in the temporal space (in lateral dislocation)
Posterior Dislocation
- Must examine the external auditory canal
Differential Diagnosis
Jaw Spasms
- Acute tetanus
- Akathisia
- Conversion disorder
- Drug toxicity (anticholinergic, phenytoin, valproate, carbamazepine)
- Dystonic reaction
- Electrolyte abnormality
- Hypocalcemic tetany
- Magnesium
- Mandible dislocation
- Meningitis
- Peritonsillar abscess
- Rabies
- Seizure
- Strychnine poisoning
- Stroke
- Temporomandibular disorder
- Torticollis
Evaluation
- Generally a clinical diagnosis
- For traumatic etiology, obtain CT face to evaluate for fracture
- Also obtain CT IAC if concern for posterior dislocation
- Examine external auditory canal, especially in posterior dislocation
- Evaluate the cranial nerves to rule out concomitant injury
Management
- If no concern for fracture, perform closed reduction in the emergency department (see techniques below)
- Often easiest to reduce one side at a time
- Provide pain control and anxiolysis as needed
- Consider procedural sedation, especially if the mandible has been dislocated for an extended period
- Local anesthetics may also be effective when injected into the preauricular depression just anterior to the tragus
Syringe Reduction Technique
- Have the patient place an empty 5 or 10 mL syringe between the upper and lower molars on one side of the mouth
- Direct the patient to roll the syringe back and forth until reduction is achieved
- If the opposite side does not spontaneously (it generally will), may repeat same technique on the opposite side
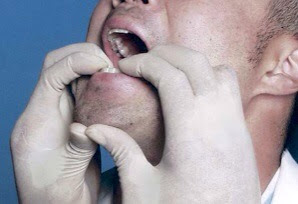
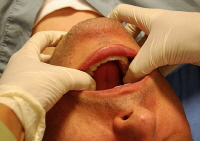
Extra-oral Reduction Technique[1]
- Place the patient in seated position
- Place one thumb on the one zygomatic arch, and the fingers of the same hand behind the mandible
- On the opposite side, place thumb on the coronoid process of the mandible
- Use the fingers of the first hand to pull the mandible forward while using the zygomatic arch to brace
- At the same time, apply firm and consistent pressure on the coronoid process with the second hand
- Once the first side is reduced, reverse hand positions and repeat the process on the second side
Intra-oral Reduction Techniques
Wrist Pivot Method[2]
- Place patient in seated position
- Face the patient and grasp the mandible with your thumbs at the apex of the mentum
- Place well-wrapped and gloved fingers on the occlusal surface of the inferior molars
- Apply cephalad force with the thumbs and caudal pressure with the fingers
- Pivot your wrists to reduce joint
Traditional Technique
- Place patient in seated position (anterior approach) or supine (posterior approach)
- Place well-wrapped and gloved thumbs over occlusal surface of inferior molars or lateral to molars in the buccal fold
- Apply caudal and posterior pressure to reduce joint
Disposition
- Generally may be discharged if uncomplicated and successfully reduced
- Instruct patient to use soft diet, not to open mouth wider than 2cm for 2 weeks, and to support mouth when yawning
- Admit for:
- Open dislocation
- Superior dislocation
- Fracture
- Nerve injury
- Inability to reduce
See Also
External Links
References
- ↑ http://sjrhem.ca/rcp-save-thumbs-extra-oral-reduction-anterior-mandibular-dislocations/
- ↑ Lowery LE, Beeson MS, Lum KK. The wrist pivot method, a novel technique for temporomandibular joint reduction. J Emerg Med. 2004 Aug;27(2):167-70. http://www.ncbi.nlm.nih.gov/pubmed/15261360