Greenstick fracture: Difference between revisions
Ostermayer (talk | contribs) (Text replacement - "Category:Ortho" to "Category:Orthopedics") |
|||
| (6 intermediate revisions by 4 users not shown) | |||
| Line 1: | Line 1: | ||
==Background== | ==Background== | ||
*Cortical disruption and periosteal tearing on convex side of bone only | *Cortical disruption and periosteal tearing on convex side of bone only | ||
*More stable / less painful than complete | *More stable / less painful than complete fracture | ||
==Clinical Features== | ==Clinical Features== | ||
| Line 11: | Line 11: | ||
*[[Torus fracture]] | *[[Torus fracture]] | ||
== | ==Evaluation== | ||
*Ultrasound scanning seems to be as sensitive as plain x-rays and may be better at demonstrating the degree of cortical deformity | *Ultrasound scanning seems to be as sensitive as plain x-rays and may be better at demonstrating the degree of cortical deformity | ||
== | ==Management== | ||
*Need for reduction determined by angulation, location, and age of child | *Need for reduction determined by angulation, location, and age of child | ||
*As a general rule, manipulation may be considered for deformity obvious to the naked eye or | *As a general rule, manipulation may be considered for deformity obvious to the naked eye or if more than the following acceptable angles<ref>Cadman, E. Wrist torus and greenstick fractures, Don't Forget the Bubbles, 2019. Available at: http://doi.org/10.31440/DFTB.21125</ref>: | ||
*Traditionally these fractures have been treated by immobilisation in plaster for a period of around 3 to 6 weeks | **>10 years old then < 10 degrees is acceptable. | ||
**<10 years old then < 15 degrees is acceptable. | |||
Traditionally these fractures have been treated by immobilisation in plaster for a period of around 3 to 6 weeks | |||
*Fractures not requiring manipulation have a universally good outcome regardless of treatment | *Fractures not requiring manipulation have a universally good outcome regardless of treatment | ||
*Higher levels of patient satisfaction with a Futura type splint | *Higher levels of patient satisfaction with a Futura type splint | ||
==Disposition== | ==Disposition== | ||
* Patients not requiring manipulation can be discharged with a backslab and advice to remove in 3 weeks or a Futura type splint and advice to remove when comfortable. There is no evidence that routine follow up is necessary. | *Patients not requiring manipulation can be discharged with a backslab and advice to remove in 3 weeks or a Futura type splint and advice to remove when comfortable. There is no evidence that routine follow up is necessary. | ||
==See Also== | ==See Also== | ||
==References== | ==References== | ||
<references/> | |||
[[Category: | [[Category:Pediatrics]] | ||
[[Category:Orthopedics]] | [[Category:Orthopedics]] | ||
Latest revision as of 20:31, 25 November 2019
Background
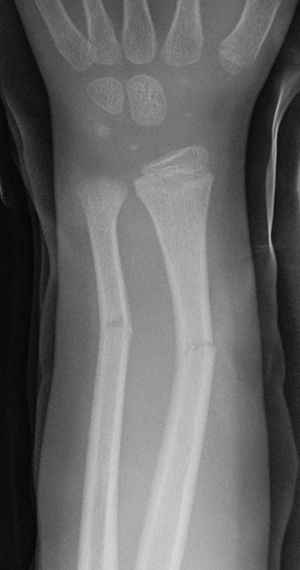
- Cortical disruption and periosteal tearing on convex side of bone only
- More stable / less painful than complete fracture
Clinical Features
- Pediatric fracture type
Differential Diagnosis
Evaluation
- Ultrasound scanning seems to be as sensitive as plain x-rays and may be better at demonstrating the degree of cortical deformity
Management
- Need for reduction determined by angulation, location, and age of child
- As a general rule, manipulation may be considered for deformity obvious to the naked eye or if more than the following acceptable angles[1]:
- >10 years old then < 10 degrees is acceptable.
- <10 years old then < 15 degrees is acceptable.
Traditionally these fractures have been treated by immobilisation in plaster for a period of around 3 to 6 weeks
- Fractures not requiring manipulation have a universally good outcome regardless of treatment
- Higher levels of patient satisfaction with a Futura type splint
Disposition
- Patients not requiring manipulation can be discharged with a backslab and advice to remove in 3 weeks or a Futura type splint and advice to remove when comfortable. There is no evidence that routine follow up is necessary.
See Also
References
- ↑ Cadman, E. Wrist torus and greenstick fractures, Don't Forget the Bubbles, 2019. Available at: http://doi.org/10.31440/DFTB.21125