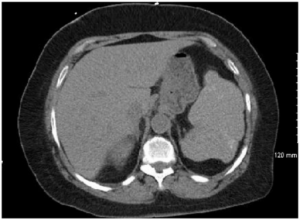
Splenic sequestration
Background
- Leading cause of pediatric mortality related to sickle cell disease[1]
- More common in pediatric patients as many adults with SCD have autoinfarcted their spleen
- Earliest life threatening complication of SCD with median age 1-43
- Red blood cells sickle, aggregate, and occlude splenic vasculature[2][3]
- Sequestering leads to splenomegaly
- Defined as splenomegaly and a 2g/dL drop in hemoglobin
- Some resources differentiate between major and minor episodes depending on the hgb drop
- Defined as splenomegaly and a 2g/dL drop in hemoglobin
- Lifelong prevalence 7-30%3
- Often precipitated by underlying infection (pneumonia, gastroenteritis)
Clinical Features
- Abdominal pain
- Fatigue
- Pallor
- Tachycardia
- Anemia
- Hypotension
- Circulatory collapse
- Splenomegaly
Differential Diagnosis
Sickle cell crisis
- Vaso-occlusive pain crisis
- Bony infarction
- Dactylitis
- Avascular necrosis of femoral head
- Acute chest syndrome
- Asthma
- Pulmonary hypertension
- Gallbladder disease
- Acute hepatic sequestration
- Infection
- Parvovirus B19
- Splenic sequestration
- CVA
- Cerebral aneurysm and ICH
- Priapism
- Papillary necrosis
Evaluation
Workup
- Labs
- CBC
- BMP
- LDH
- Reticulocyte count
- LFTs
- Blood cultures
Diagnosis
- Imaging not necessary to make diagnosis
Management
- Pain control
- IV fluid resuscitation and blood transfusion[4]
- Caution with IVF if anemia is severe
- Goal Hct 35% to avoid hyperviscosity syndrome3
- Treat underlying cause if found - infection common
- Possible splenectomy
- Recurrence rate is 50-75%1,2,3[5]
- Hematology consultation
Disposition
- Admission
Complications
See Also
External Links
References
- ↑ Brousse V et al. Acute splenic sequestration crisis in sickle cell disease: cohort study of 190 pediatric patients. British Journal of Haematology. 2012;156:643-648.
- ↑ Brousse V et al. The spleen and sickle cell disease: the sick(led) spleen. British Journal of Haematology. 2014;166:165-176.
- ↑ Lovett PB et al. Sickle Cell Disease in the Emergency Department. Emerg Med Clin N Am. 2014;32(3):629-647.
- ↑ Abboud MR. Standard management of sickle cell disease complications. Hematology/Oncology and Stem Cell Therapy. 2020;3(1):85-90.
- ↑ Kane I, Nagalli S. Splenic Sequestration Crisis. [Updated 2020 Jul 6]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK553164/